Month: September 2020
Medicaid Map Updated 09/24/2020
Are You Prepared for 2021 E/M Code Changes?
Cigna HealthSpring and CIOX Health
CIOX is here to help with the medical record retrieval and to work with the provider offices. Some options for the provider, depending on their specific needs/protocols are:
- For the staff to collect and submit the medical records
- To have CIOX come in to the clinic to collect the medical records in a designated work space and computer/laptop
- To set up remote EHR access for the CIOX representative to remote in to collect medical records

AND MEDICAL RECORD RETRIEVAL HELPS WITH RISK SCORES.
Provider Roster Updated 09/15/2020
Roster was updated to reflect UHC All Products effective 9/15/2020. Click to review.
Physician Directory Updated 09/14/2020
To view the updated Directory for changes.
Access to Medical Records of a Deceased Patient (TMA)
Aetna OfficeLink Updates, Published 9/1/2020
- Changes to the National Pre-Certification List
- Third Party Claim and Code Review Program
- And many interesting topics
AIM Specialty Health (AIM) to Perform Utilization Management for:
Participants with three-character prefixes of T2U and T2S (Group #3850X -last digit varies by plan) who are under 65 years of age and are active employees.
This is referring to TRS ActiveCare Patients.
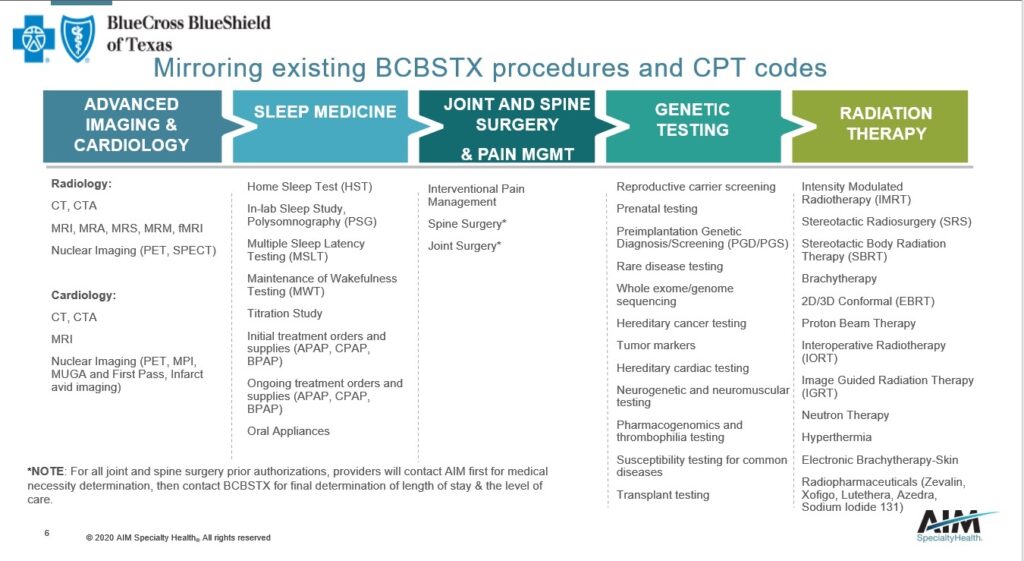
To log in to “AIM” click the blue text.
To review the “AIM” training slide deck, click here.
UPCOMING Provider/Portal Training Dates
- Advanced Imaging & Cardiology: Tuesday, Sept. 15 (10 AM-11 AM)
- Sleep Medicine: Wednesday, Sept. 16 (12 PM-1 PM)
- Joint and Spine Surgery:Thursday, Sept. 17 (12 PM-1PM)
- Pain Management: Tuesday, Sept. 15 (9 AM-10 AM)
- Radiation Therapy: Thursday, Sept. 17 (3 PM-4PM)
- Genetic Testing Services: Tuesday, Sept. 15 (12 PM -1 PM)
Welcome to Blue Cross and Blue Shield of Texas (BCBSTX) Provider Orientation Information
On May 13, we announced we were awarded the contract to administer medical and behavioral health benefits for the Teacher Retirement System of Texas (TRS), effective Sept. 1, 2020. TRS-ActiveCare participants will be offered health plans that use either the nationwide Blue Choice PPOSM or statewide Blue EssentialsSM provider networks.
TRS-ActiveCare Plans
Statewide Blue Essentials network – providers who are contracted under the Blue Essential network can see participants on these plans:
- TRS-ActiveCare Primary and TRS-ActiveCare Primary+
- Copays for doctor visits before meeting deductibles.
- Primary care provider (PCP) selection and referrals to specialists are required.
- No out-of-network coverage, except for true emergencies.
Nationwide Blue Choice PPO network plans – providers who are contracted under the Blue Choice PPO network can see participants on these plans:
- TRS-ActiveCare HD
- High deductible plan which may include a health savings account (HSA) to pay for medical care.
- Does not require PCP selection or referrals.
- Deductibles must be met before the plan pays for diagnostic care.
- Includes out-of-network coverage. Participants have a lower cost share when using in-network providers.
- TRS-ActiveCare 2
- Copays for doctor visits before meeting deductibles.
- Does not require PCP selection or referrals.
- Includes out-of-network coverage. Participants have a lower cost share when using in-network providers.
Identifying TRS-ActiveCare Participants
TRS-ActiveCare participants can be identified by the following on their BCBSTX ID card:
- The TRS-ActiveCare logo will be displayed on the participants’ ID card.
- TRS-ActiveCare Primary and TRS-ActiveCare Primary+ plan holders will have ID cards with a three-character prefix of T2U.
- TRS-ActiveCare HD and TRS-ActiveCare 2 plan holders will have ID cards with a three-character prefix of T2S and a network ID of BCA.
For patients on TRS-ActiveCare Primary and TRS-ActiveCare Primary+, you must be their assigned provider to provide primary care services. Patient eligibility and benefits should be checked using Availity® or your preferred vendor before every scheduled appointment. Eligibility and benefit quotes include patients’ coverage status and other important information, such as applicable copays, coinsurance and deductibles. It’s strongly recommended that providers ask to see patients’ ID card and photo ID to guard against medical identity theft. If services may not be covered, patients should be notified that they may be billed directly.
Prior Authorization
You can check the Prior Authorization and Predeterminations page for the list of Administrative Services Only (ASO) services and procedure codes that require prior authorization for TRS participants. Refer to How to Submit a Prior Authorization or Prenotification to learn about submission processes.
Reminders
TRS will continue to use CVS Caremark as their pharmacy benefit manager. We encourage you to attend provider training sessions related to TRS-ActiveCare benefits, prior authorization requirements and ID cards. Continue to watch News and Updates and our Blue Review newsletter for more details on TRS-ActiveCare.
If you have any questions, please contact your BCBSTX Network Management Representative.
As a reminder, it is important to check eligibility and benefits before rendering services. This step will help you determine if prior authorization is required for a participant. For additional information, such as definitions and links to helpful resources, refer to the Eligibility and Benefits section on BCBSTX’s provider website.
Please note that checking eligibility and benefits, and/or the fact that a service or treatment has been prior authorized or predetermined for benefits are not a guarantee of payment. Benefits will be determined once a claim is received and will be based upon, among other things the participant’s eligibility and the terms of the member’s certificate of coverage applicable on the date services were rendered. If you have questions, contact the number on the ID card.
Availity is a trademark of Availity, LLC, a separate company that operates a health information network to provide electronic information exchange services to medical professionals. Availity provides administrative services to BCBSTX. BCBSTX makes no endorsement, representations or warranties regarding any products or services provided by third party vendors such as Availity. If you have any questions about the products or services provided by such vendors, you should contact the vendor(s) directly.
Click to view the training declk “AIM Provider Training for Prefixs T2U and T2S”
Click to view the training slide deck called “Introduction to TRS-ActiveCare”

Recent Comments