Month: October 2023
STOP BACK OFFICE THEFT

5 Tips to Help Stop Theft in Your Back Office
It’s unfortunate, but even in today’s era of two-factor authentication and hyper-alert security, we still hear stories of physicians being defrauded by their employees. To help protect yourself from financial fraud, consider adopting these five approaches in your practice.
1) Cross-Train Your Employees
The most common place for fraud to occur is in the back office of small businesses where only one person handles the cash and books. Train more than one person on the cash conversion cycle. Rotate people through the various processes, too, so that no single person operates in a silo. When multiple people know the process, they can check each other’s work for mistakes and anomalies. Cross-training employees helps to create an open and transparent environment. It also reduces the chance of theft by assuring no one person wields too much power. Ultimately, it would be best if you also knew the process, so you can be an effective leader and fiscally responsible business owner
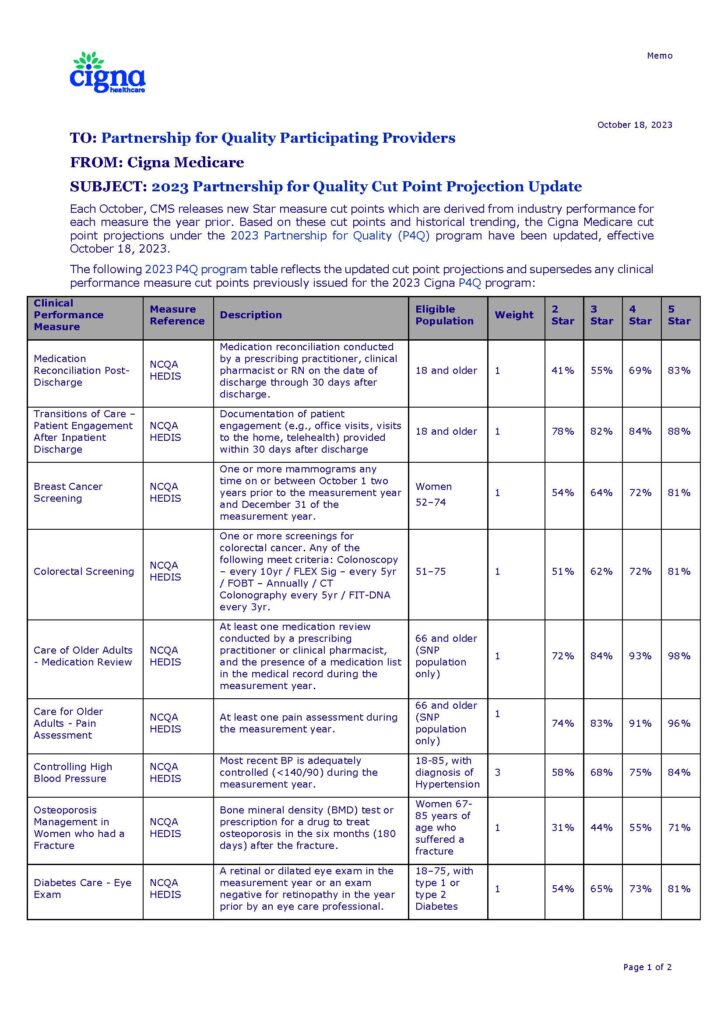
2023 P4Q Cut Point Projection Update
5 State and Federal Training Mandates

There are five topics that physicians and their staff must receive training on regularly per state and federal requirements, and the TMA Education Center offers programs to meet those mandates.
All these programs are free to members and their staff as a benefit of membership, saving members $200 or more per program or more than $2,000 combined. Find them in the TMA Education Center under the Opioid and Mandated Trainings topics.
State:
- Human trafficking: Meets all required Texas Health and Human Services Commission (HHSC) Human Trafficking Training Standards, is approved by HHSC in accordance with House Bill 2059 (2019), and addresses how to recognize, screen for, and report suspected human trafficking.
- Pain management and the prescribing and monitoring of controlled substances required by the Texas Medical Board: State requirement for a total of 2 hours of formal CME that count as ethics credit and addresses:
- Best practices, alternative treatment options, and multimodal approaches to pain management that may include physical therapy, psychotherapy, and other treatments;
- Safe and effective pain management related to the prescription of opioids and other controlled substances, including education regarding standards of care; identification of drug-seeking behavior in patients; and effectively communicating with patients about the prescription of an opioid or other controlled substances; and
- Prescribing and monitoring of controlled substances.
Federal:
- OSHA: Federal requirement for annual training for all health care workers.
- Treatment and management of patients with opioid or other substance use disorders required for all U.S. DEA-registered practitioners: Federal requirement, one-time 8 hours of specified training.
Federal and state:
- HIPAA and Texas medical privacy laws: Federal and state requirements annually, regularly, and/or within 90 days of hiring.
TMA’s Education Center also has dozens of other courses you can find anytime, available at no cost to members thanks to TMA Insurance Trust.
Disclaimer: Participation in this program in no way implies the participant has fully met the federally and state-mandated training requirements. Participants are solely responsible for ensuring any mandated training requirements are completed.
Superior Prior Auth Changes Eff. 1/1/2024

For some services, utilization review is necessary to determine the medical necessity and appropriateness of a covered health care service for Superior HealthPlan’s managed care members. For those services, utilization review is performed BEFORE (prior authorization), during (concurrent review) or after (retrospective review) the service is delivered.
MLN Connects News
2024 Medicare Part B Deductible.
The annual deductible for all Medicare Part B beneficiaries will be $240 in 2024, an increase of $14 from the annual deductible of $226 in 2023.
Discarded Drugs and Biologicals:
When to Use JW and JZ Modifiers.
Read updated JW and JZ Modifier FAQs for additional clarity on billing with these modifiers (see FAQs 7, 8, and 18–22). CMS posted a new list of billing and payment codes only used for single-dose containers that may require the modifiers, depending on the setting:
Aetna OfficeLink Updates, Oct. 1, 2023
Healthcare Common Procedure Coding System (HCPCS) modifiers FX and FY
Effective January 1, 2024, we will reduce payment for radiology procedures billed with modifiers FX and FY to align with the Centers for Medicare & Medicaid Services (CMS) guidelines.
• Modifier FX (X-ray taken using film): A 20% payment reduction applies to the technical component (and the technical component of the global fee).
• Modifier FY (computed radiography X-ray): A 10% payment reduction applies to the technical component (and the technical component of the global fee).
Reimbursement for code A9279
(monitoring feature/device)
Effective January 1, 2024, Aetna® will no longer reimburse for code A9279, since it is considered statutorily non-covered.
Cigna MA on CoVid Testing Coverage and Reimbursement.

The waiver for customer cost-share for physician visits for test (both in and out of network) ended May 11, 2023. However, laboratory tests for CoVid ordered by the provider will continue to be covered with no out-of-pocket costs following the end of the PHE on May 12, 2023.

Medicaid and CHIP Program Revalidation
IMPORTANT:
During the Public Health Emergency (PHE), Provider
Revalidation was waived by HHSC.
The PHE ended May 11, 2023
Beginning May 12, 2023, Provider Revalidation Requirements were resumed.
Providers must ensure Medicaid and/or CHIP enrollment revalidation is completed on or before the provider’s scheduled revalidation date.
Providers that do not complete the revalidation process by their deadline are DISENROLLED from all Texas state healthcare programs, including Medicaid and/or CHIP managed care programs.
Visit the Texas Medicaid & Healthcare Partnership (TMHP) Provider Enrollment webpage to view and confirm your upcoming Medicaid and /or CHIP program revalidation date, verify current enrollment is active and verify all information in the PEMS system is accurate.


Recent Comments