Category: Medicaid
Superior PCP Change Request Form

I didn’t know?
How was I supposed to know?
We all know it is going to happen. The PCP on the card is not yours. And know one knew.
But Superior has made it a little easier. No setting on hold.
Help the patient fill it out.
For Star Health, fax the completed form to (866) 626-6069.
For all others, fax to (866) 918-4447.
Superior HealthPlan Billing Changes
Important Provider Update
Effective September 1, 2025
The Texas Health and Human Services Commission (HHSC) will transition Medicaid-only services for dually eligible clients (eligible for both Medicare and Medicaid) from Fee-for-Service (FFS) to a Managed Care service delivery system.
Superior HealthPlan will be responsible for adjudicating these claims.
Provider Responsibilities
Submit claims for Medicaid-only services for dual eligible clients directly to the Managed Care Organization (MCO).
If a Claim is Sent to TMHP in Error:
TMHP will forward the claim to the correct MCO.
The TMHP response will only confirm forwarding – no ER&S report will be issued.
Claims with dates of service on or after Sept. 1, 2025 will not be adjudicated by TMHP.
Provider Action Steps
✅ Submit Medicaid-only service claims directly to the MCO.
✅ Contact the MCO for claim status and adjudication questions.
✅ Review the Rider 32 Procedure Code List (PDF) for impacted services.
✅ Reach out to your Provider Representative via the Find My Provider Representative webpage.
Need Help?
Contact your dedicated Provider Representative

TMHP, New Provider Enrollment Tool
Addressing physician concerns about online Medicaid enrollment challenges, the Texas Medicaid and Healthcare Partnership (TMHP) has announced its new Provider Enrollment Assistant Tool (PEAT) is available for enrollment-related help.
Users can navigate to the help page in TMHP’s provider enrollment section to access the tool, which TMHP describes as “question-based software.” Typing in a question prompts PEAT to provide:
- Answers to revalidation questions, including due dates;
- Online appointment scheduling for personalized support with enrollment issues, including step-by-step guidance from a TMHP representative;
- Information about Provider Enrollment and Management System (PEMS) maintenance requests; and
- Instructions for new enrollments, re-enrollments, and updates to existing enrollments.
Before initiating a PEAT request, TMHP advises having at the ready your National Provider Identifier (NPI), ZIP code, taxonomy number (if applicable), and any contact information related to the NPI.
In addition to a PEAT info sheet accessible online, TMHP is offering walk-through sessions for those needing additional enrollment support, which can be scheduled via PEAT, and offers an online PEMS guide updated in March.
UHC July Overview
Policy and protocol updates
Medical policy updates
Medical policy updates for July 2025 for the following plans: Medicare, Medicaid, Exchanges and commercial.
Reimbursement policy updates
See the latest updates for reimbursement policies.
Specialty Medical Injectable Drug program updates
See the latest updates to requirements for Specialty Medical Injectable Drugs for UnitedHealthcare members.
Pharmacy and clinical updates
Access upcoming new or revised clinical programs and implementation dates for UnitedHealthcare plans
HEADS UP! Rider 32 Transition
Effective September 1, 2025
Texas Health and Human Services Commission will implement Rider 32, which will transition Medicaid only services for dually eligible members from a fee-for-service model to a managed care delivery system.
This change affects services provided to members who are eligible for both Medicaid and Medicare. It applies only to those Medicaid services not covered by Medicare.
Providers will bill the MCO for Medicaid wrap-around services provided to dually eligible members.
Wrap-around services include all Medicaid services not covered by Medicare. They are limited to those already covered under managed care for Medicaid-only members.
Superior: New Availity Claim Features and Webinars.
|
Superior: Appeal Submissions
IMPORTANT: Post-Service Medical Necessity Appeal Submissions
Superior HealthPlan would like to remind providers that post-service Medical Necessity Appeals must be mailed or faxed using the submission information below. Submissions must include the reason for appeal and any additional clinical information for appeal review..
Centene Management Company
ATTN: Medical Management Appeals
5900 E. Ben White Blvd
Austin, Texas 78741
Fax number: 1-866-918-2266
Post-service appeals for reconsideration of a Medical Necessity Denial on behalf of a member should not be sent to the Claims Appeal address.
For questions about post-service Medical Necessity Appeals, providers can contact 1-877-398-9461.
Prior Auth for Certain Sleep Studies, No Longer Required by Superior as of April 1, 2025.
For all Medicaid (STAR, STAR Health, STAR Kids, STAR+PLUS), CHIP and Ambetter from Superior HealthPlan members, Superior will no longer require prior authorization for the following Current Procedural Terminology (CPT) codes:
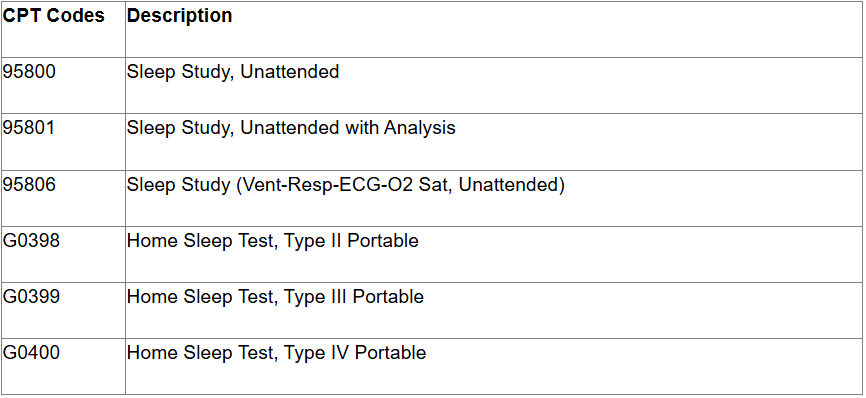
For Medicaid, CHIP and Ambetter members 17 years of age and younger, Superior will no longer require prior authorization for the following CPT codes:


Recent Comments