Tag: Texas Medical Association (TMA)
More Telehealth Waivers Set to Expire Dec. 31
As TMA monitors the government shutdown and the coinciding expiration of certain telehealth waivers as of Sept. 30, physicians should take notice of another series of telehealth waivers set to expire at the end of this year.
TMA staff note that Medicare Advantage plans don’t have to follow Medicare’s policy on the waiver expirations.
The following waivers enacted during the COVID-19 public health emergency (PHE) are currently expected to expire Dec. 31 unless Congress acts:
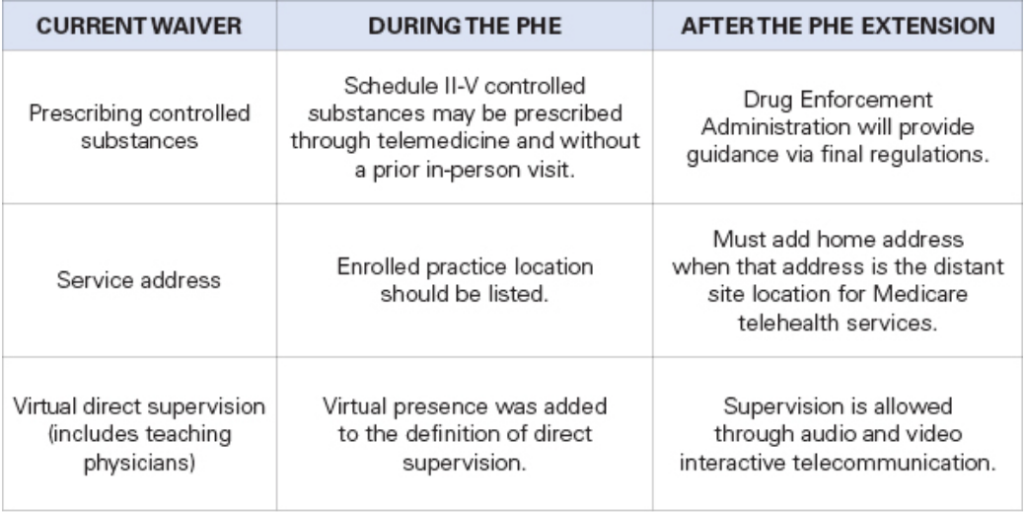
The following waivers have already expired:
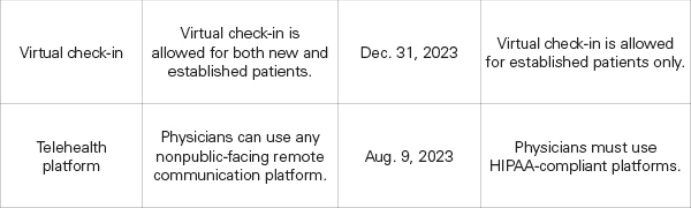
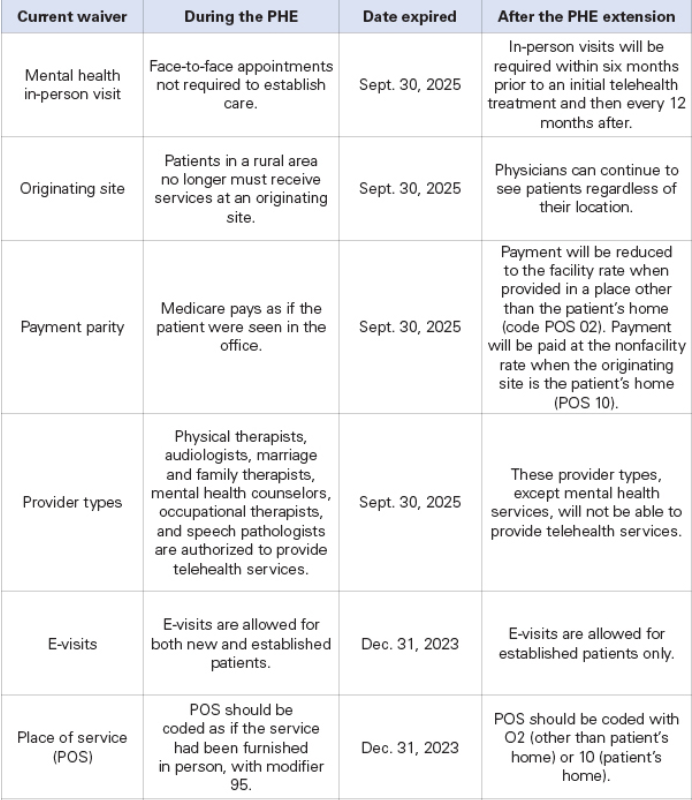

TMA Coming to Tyler
Local Medicine Matters Conference Tyler, Texas
October 24-25, 2025

The Local Medicine Matters Conference is a new regional event, part of the Texas Medical Association’s initiative to hold events beyond the Texas metro areas. This inaugural conference is being hosted by the Smith County Medical Society in conjunction with TMA. The one-day event features topics of broad interest across all physician members, including practical uses of augmented intelligence in medicine, updates to billing and coding, and how physicians fared following the 2025 Texas legislative session.
Friday Night Mixer Oct. 24th
5:00 PM – 7:PM
Guest and Members Free
Saturday Conference Oct. 25th
7:30 AM – 4:00 PM
TMA Members Free
Registration
Registration for TMA members, CMS and association staff, and Alliance members is FREE – one of the many benefits of annual membership!
A $25 registration fee will be charged for on-site registrants.
Registration Fees:
Nonmember physicians: $200
Guests of members and medical staff: $150
Conference Agenda
Friday, Oct. 24 | The Grove Kitchen and Gardens
5 pm – 7 pm | Regional Membership Happy Hour
Saturday, Oct. 25 | Brookshire Conference Center
7:30 am – 1:00 pm | Registration Open
8:00 am – 8:30 am | Walk-with-A-Doc in the Tyler Rose Garden
8:15 am – 9:00 am | Breakfast
9:00 am – 9:15 am | Opening Remarks
Jayesh Shah, MD, President, Texas Medical Association
9:15 am – 10:15 am | Augmented Intelligence: Policies, Procedures, and Preparation
Explore how augmented intelligence (AI) is being practically applied in medicine to enhance efficiency and ease for healthcare professionals.
Shannon Vogel, AVP, Health Information Technology, Texas Medical Association
10:25 am – 11:25 am | P.R.O.A.C.T.I.V.E
In billing, your best practice is to be proactive. When you are reactive, payment delays, denials, and loss of revenue are more likely to occur. This presentation will review key points and best practices for being proactive to assist with efficiency and minimize unnecessary delays.
Carra Benson, Director, Physician Payment Services, Texas Medical Association
11:30 am – 12:30 pm | Lunch
12:30 pm – 1:30 pm | 2025 Legislative Wins: Texas Edition
Jayesh “Jay” Shah, MD, President, Texas Medical Association
Matt Dowling, Director of Public Affairs, Lobbyist, Texas Medical Association
1:40 pm – 2:40 pm | Lawsuits and TMB Investigations: How to Avoid Them (Ethics CME)
Lajuana Acklin, JD, Senior Associate, Bertolino Law Firm
2:50 pm -5:00 pm | Media Training
Brent Annear, Associate Vice President, Media Relations and Leadership Advancement, Texas Medical Association
Goverment Shutdown: What you Need to Know
With the government shutdown in effect, the Texas Medical Association is in regular communication with federal colleagues at the American Medical Association on the impact to physician practices, as AMA remains in touch with senior officials at the Centers for Medicare & Medicaid Services (CMS).
The volatility in Washington, D.C. could mean the shutdown lasts days to weeks, and TMA will share additional information via Texas Medicine Today as the situation develops. Here is what physicians need to know so far:
Medicare/Medicaid: The CMS contingency plan states that during a lapse in funding, the Medicare program will continue. CMS also says it has sufficient funding for Medicaid to fund the first quarter of 2026 and is maintaining the staff necessary to make payments to eligible states for the Children’s Health Insurance Program.
Medicare Administrative Contractors (MACs) have been instructed to implement a temporary claims hold of 10 business days, which AMA says should have minimal impact on physicians due to the 14-day payment floor. “The hold prevents the need for reprocessing large volumes of claims should Congress act after the statutory expiration date,” states a CMS Medicare Learning Network Connects special edition email newsletter that, as of this writing, had not yet been publicly posted. Physicians may continue to submit claims during this period, but payment will not be released until the hold is lifted. For the latest information, AMA recommends physicians monitor their MAC’s website (Novitas in Texas) and this CMS webpage.
“In the past, Congress generally has restored lapsed policies back to the effective date of the shutdown. During the shutdown, the AMA is monitoring any potential delays in Medicare claims processing or other Medicare payment problems that could result from federal staffing reductions at CMS, including during the shutdown,” said AMA CEO and Executive Vice President John Whyte, MD, MPH.
Telehealth: Physicians who provide telehealth services to fee-for-service Medicare patients should be aware that the Medicare telehealth flexibilities lapsed on Sept. 30 for most care and congressional action is required to restore that waiver. The exceptions are patients being treated for mental health and/or behavioral health disorder (including substance use disorders), stroke, and monthly end-stage renal disease visits for home dialysis. Otherwise, telehealth services are limited to rural areas as they were before the COVID public health emergency, and patients cannot receive telehealth services in their homes. The ability to provide audio-only services to Medicare patients also lapsed, as did the Acute Hospital Care at Home program.
The CMS newsletter suggests “practitioners who choose to perform telehealth services that are not payable by Medicare on or after Oct. 1, 2025, may want to evaluate providing beneficiaries with an Advance Beneficiary Notice of Noncoverage.”
However, AMA notes physicians in certain Medicare Shared Savings Program accountable care organizations can continue to provide and be paid for telehealth services.
Other services: CMS says it is continuing federal insurance marketplace activities, such as eligibility verification. Other nondiscretionary activities including health care fraud and abuse control and Center for Medicare & Medicaid Innovation activities are also continuing.
However, AMA reports that funding extensions for community health centers, the National Health Service Corps, and teaching health centers that operate graduate medical education programs expired on Sept. 30, and the 1.0 work geographic practice cost index floor extension expired on Oct. 1. Additional programs that have lapsed include: special diabetes programs; public health emergency authorities (e.g., Public Health Emergency Fund); increased inpatient hospital payment adjustment for certain low-volume hospitals; the Medicare-Dependent Hospital program; quality measure endorsement, input, and selection; and outreach and assistance for low-income programs (e.g., area agencies on aging).
TMA wants to hear from you. If you or your practice staff experience Medicare payment delays, telehealth obstacles, or other concerns, please let us know through TMA’s Knowledge Center to help inform advocacy.
Amy Lynn Sorrel
Associate Vice President, Editorial Strategy & Programming
Division of Communications and Marketing
TMA Billing, Coding, and Payment Resources
TMA’s billing, coding, and payment page offers resources for physician practices, from one end of the continuum to the other. Educate yourself with our articles and tools, or get help with more complex questions.
Physician Payment Resource Center
TMA’s Physician Payment Resource Center (formerly known as the Hassle Factor Log and the Reimbursement, Review and Resolution Service) goes to bat for members by helping to resolve issues related to insurance payments.
TMA can help resolve issues with your payer network status, prompt-pay, and other reimbursement claims. Learn More
Billing and Coding Hotline
Speak directly with TMA’s certified coders and staff experts about regulatory compliance, billing and coding, payment, and licensure concerns.
(512) 370-1414
TMHP, New Provider Enrollment Tool
Addressing physician concerns about online Medicaid enrollment challenges, the Texas Medicaid and Healthcare Partnership (TMHP) has announced its new Provider Enrollment Assistant Tool (PEAT) is available for enrollment-related help.
Users can navigate to the help page in TMHP’s provider enrollment section to access the tool, which TMHP describes as “question-based software.” Typing in a question prompts PEAT to provide:
- Answers to revalidation questions, including due dates;
- Online appointment scheduling for personalized support with enrollment issues, including step-by-step guidance from a TMHP representative;
- Information about Provider Enrollment and Management System (PEMS) maintenance requests; and
- Instructions for new enrollments, re-enrollments, and updates to existing enrollments.
Before initiating a PEAT request, TMHP advises having at the ready your National Provider Identifier (NPI), ZIP code, taxonomy number (if applicable), and any contact information related to the NPI.
In addition to a PEAT info sheet accessible online, TMHP is offering walk-through sessions for those needing additional enrollment support, which can be scheduled via PEAT, and offers an online PEMS guide updated in March.
VA Seeking Refunds for Past CHAMPVA Claims
The U.S. Department of Veterans Affairs (VA) announced it aims to recover more than $41 million in “overpaid claims” paid to physicians and other health care professionals and entities through the Civilian Health and Medical Program of the Department of Veterans Affairs (CHAMPVA) program.
Texas Medical Association staff caution that physicians receiving CHAMPVA refund requests should take several steps to satisfy the VA request without immediately losing payment for care already delivered:
- Confirm the legitimacy of the request letter. As refund letters typically come from third-party companies, a practice may call CHAMPVA and ask them if the third-party company is one they contracted with to collect the overpayment;
- Check the letter for details on how to appeal, including any payment or appeal deadlines; and
- Check the letter for information about which insurer VA says is responsible for payment.
From there, physicians can choose one of two actions. If it appears the alleged overpayment has been identified in error, start the appeal process to try to keep the CHAMPVA payment already received. If not pursuing an appeal – or if an appeal is ultimately denied – refund the overpayment to VA and seek payment from the insurer VA says is responsible for payment. For a physician seeking payment from that insurer, TMA recommends including, as part of that request, the initial CHAMPVA explanation of benefits and any information from VA indicating that the insurer is the proper payer, especially if the filing deadline has passed.
For assistance with CHAMPVA refund requests or other payment matters, contact TMA’s Physician Payment Resource Center.
Separate Services, Same Date of Service
With health plans increasingly adopting payment protocols that hinder physicians from providing multiple services on the same day – despite previously covering such services – delegates adopted policy calling on TMA to “advocate for legislation or regulation that would prevent Medicaid and commercial payers from denying payment for distinct, separate services provided on the same day.”
Delegates agreed with physicians’ concerns that these payer practices often force patients to forego care.
“This especially hurts patients who either have to travel long distances to see their physician or have transportation issues that prevent them from making multiple trips,” Odessa allergist and immunologist Vivek Rao, MD, wrote in online testimony on behalf of the Lone Star Caucus
Other measures adopted by the house to eliminate payment-related barriers to patient care direct TMA to pursue state-level legislation or regulation that:
- Prohibits insurers, plan sponsors, third party administrators, and other contracted identities from recouping previously paid claims due to retroactive termination of patient coverage;
- Imposes payer communication standards – with penalties – that provide patients, physicians, and others with timely access to a live representative; and
- Expedites prior authorization approvals for hospice care in emergency and acute care settings, eliminates deductibles for hospice care, and provides clear disclosures detailing hospice care benefits in policy documents as well as online.
Mandated CME Requirements Are Shifting
A recent reorganization of Texas Medical Board (TMB) rules has removed certain universal CME obligations. The removal of universal CME requirements could result in a lighter load for physicians but may make it more challenging to determine what is required and when.
Please click the button below to view the entire article from Texas Medical Assocation.
Check Your BCBS Flu Test Claims
BCBSTX explained in correspondence with TMA’s Physician Payment Resource Center (PPRC) – which reached out for clarification earlier this month on the payer’s new flu testing policy – that some claims for certain labs, including those offering flu testing, were unintentionally denied due to a vendor error.
TMA’s Director of Physician Payment Services Carra Benson says physicians do not need to take action to receive payment. However, she recommends physicians review flu testing claims filed between Jan. 1 and Feb. 13 to ensure correct reprocessing.


Recent Comments