As a result, Cigna Commercial and Cigna Medicare Advantage plan to make the following changes on May 12, 2023:
Tag: Public Health Emergency (PHE)
THE END IS NEAR

What’s Next for Telehealth?
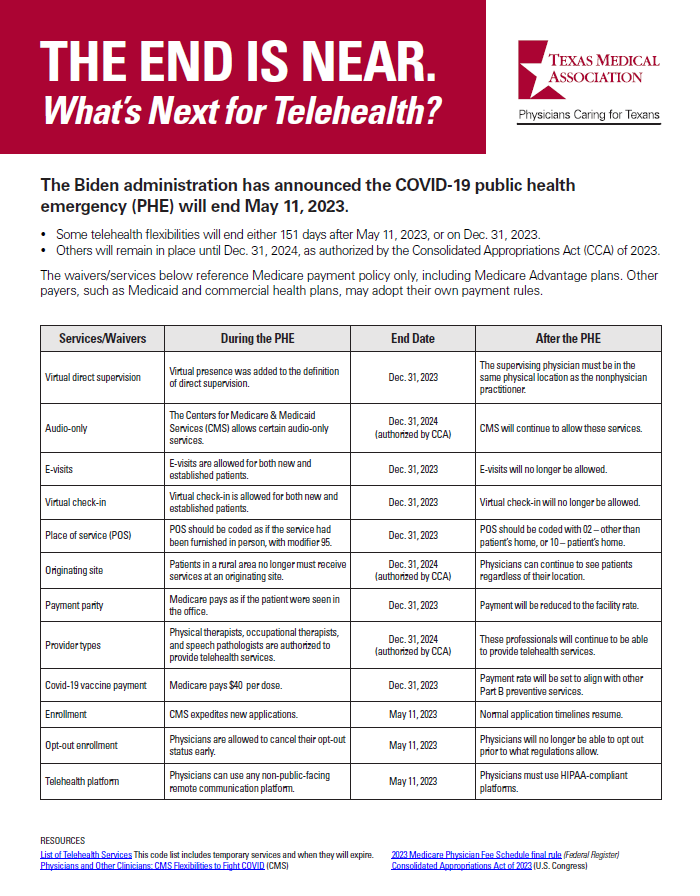
Big Changes, End of PHE
Cigna CoVid Coverage Changes
Author: Seymore Bones Published Date: April 13, 2023 Leave a Comment on Cigna CoVid Coverage Changes
Changes in coverage effective May 12, 2023
The White House has announced their intent to end both the CoVid-19 National Emergency and Public Health Emergency (PHE) on May 11, 2023.
- Authorizations for facility-to-facility transfers will again be required.
- Patient cost-share will apply to COVID-19 lab tests as well as antiviral and therapeutics approved by the U.S Food & Drug Administration (FDA).
- For most benefit plans, COVID-19 vaccines will be covered at 100 percent under the preventive benefit (same as the flu shot) when customers go to an in-network provider.
- Over-the-counter COVID-19 tests will no longer be covered.
Cigna Coverage Changes
ASK THE EXPERT
TMA RESOURCES |
Ask the Expert: End of the Public Health EmergencyOn March 29 via Zoom, join TMA experts in this interactive Q&A session as they discuss how best to prepare your practice for upcoming changes as the public health emergency winds down on May 11. They will discuss the impact on Medicaid coverage, telehealth, and COVID vaccines and treatments for which you can earn CME. Send your questions in advance. Register now. |
HHS Announces End of PHE
According to HHS.Gov Fact Sheet: COVID-19 Public Health Emergency Transition Road Map
The Public Health Emergency (PHE) for COVID-19 is scheduled to expire at the end of the day on May 22, 2023.
The Song That Doesn’t End
Please be advised the Public Health Emergency (PHE) for Coronavirus Disease (COVID) which expired October 13, 2022.has now been extended by the U.S. Department of Health & Human Services Secretary, Xavier Becerra.
The renewal of the PHE is effective October 13, 2022. Absent another renewal, the PHE is anticipated to expire at 11:59 pm on January 11, 2023.
Song Credits: Shari Lewis
Feds Clarify HIPAA Enforcement When PHE Ends
Author: Seymore Bones Published Date: August 22, 2022 Leave a Comment on Feds Clarify HIPAA Enforcement When PHE Ends
New federal guidance clarifies that relaxed HIPAA enforcement will end at the conclusion of the COVID-19 public health emergency (PHE), while offering instruction on how physicians and others covered by HIPAA can continue to use remote communication technologies to provide audio-only telehealth services.
Back at the start of the pandemic, the U.S. Department of Health and Human Services (HHS) Office for Civil Rights (OCR) said it would not “impose penalties for noncompliance with the regulatory requirements under the HIPAA Rules against covered health care providers in connection with the good faith provision of telehealth during the COVID-19 nationwide public health emergency.”
In the new guidance, OCR reiterated that this discretion remains in effect only until the HHS secretary determines the PHE no longer exists or when it expires, whichever occurs first. Congress previously granted a five-month extension for other COVID-related waivers following the conclusion of the PHE..
OCR issued the guidance in direct response to a December 2021 presidential executive order intended to help ensure patients can continue to benefit from audio-only telemedicine and telehealth services with protection of their personal health information.
The new guidance elaborates on types of technologies, business associate agreements with vendors, and ensuring HIPAA compliance when using audio-only technologies.
The Texas Medical Association has numerous resources designed to help physicians adopt and effectively use telemedicine. Visit TMA’s telemedicine page for more information.
Click on the blue highlighted text within the article for more information.
OR
Head to the Business End File and view articles on Telemedicine, and Telemedicine Policy, Procedure, and Form Templates
It Has to End Sometime. Doesn’t It?
Author: Seymore Bones Published Date: August 1, 2022 Leave a Comment on It Has to End Sometime. Doesn’t It?
What Will the End of the PHE Mean for Coverage?
The PHE has been extended 8 times since January 31st. We all have I fingers crossed that this is the last time. But there is a lot of uneasiness regarding the “WHAT IFs” of when it does.
To get some great insight check out this article from TMA.ED

Cigna Medicare HSConnect Portal
Author: Seymore Bones Published Date: July 20, 2022 Leave a Comment on Cigna Medicare HSConnect Portal
Cigna MA has reported two known issues with HSConnect.
- Referrals are pending unnecessarily.
- The procedure start and end date are defaulting to the same day.
An expected date for resolution has not been provided.

But there is good news (tongue in cheek) the PHE has been extended. Therefore, referrals are still waived. Those items requiring precertification will continue to need an authorization.
PHE Extended

July 15th, Secretary of Health and Human Services, Xavier Becerra renewed the determination that a public health emergency exists. This will add another 90 days, extending the PHE through October 13, 2022
PHE Extended
PHE Extended Through 7/15/2022
Author: Seymore Bones Published Date: April 18, 2022 Leave a Comment on PHE Extended Through 7/15/2022
Will the End of the PHE Impact Physicians Practices and Patient Coverage?

You Bet Your Rain Boots it Will!
PHE Extended through 7/15/2022
Recent Comments