Month: May 2022
Hospitals Are Required
Per TMA Article Published 5/25/2022
Hospitals are required to let you know when they’ve seen your patient via an admit, discharge, or transfer (ADT) notice. To ensure that happens, physicians are required to make sure their digital contact information in a federal database is up to date.
As part of the same federal rule, physicians are required to update their digital contact information in the National Plan and Provider Enumeration System (NPPES) so hospitals have the information they need to electronically send the ADT notices.
Your digital contact information should not be a standard email address, rather a direct protocol or similar HIPAA-compliant address. The Texas Health Services Authority direct protocol workgroup has developed practical instructions on how to add your digital address to NPPES
For More Information Check out these links:
Interoperability and Patient Access final rule.
Cigna New Medical Records Nightmare

Starting Aug. 13, Cigna commercial payer will request patients’ medical records when billed for an office or other outpatient visit where a minor procedure also occurred, according to a letter sent to physicians and other health care professionals.
The Texas Medical Association and American Medical Association are monitoring the issue.
Carra Benson, TMA’s manager of practice management and reimbursement, says this new policy – and similar ones from other commercial payers – could prove to be “an administrative nightmare” given the ubiquity of office visits that include a minor procedure.
For instance, a dermatologist may discover a concerning mole and remove it during the same routine office visit. Likewise, a family medicine physician may see a patient for a scheduled joint injection and learn the patient has been experiencing chest pain and shortness of breath. If the physician sends the patient for a chest X-ray and electrocardiogram, then the physician would bill for the office visit related to the acute symptoms as well as the originally scheduled minor procedure, according to the American Academy of Professional Coders.
In coding terms, this policy change applies to evaluation and management codes 99212 through 99215, when billed with a modifier 25. That modifier is used to indicate a minor procedure, of which there are more than 1,600.
Ms. Benson says practices that often bill for such visits could find themselves overwhelmed by medical records requests from Cigna. This burden would fall especially hard on solo and small practices, which have limited staff to meet such demand, she adds.
Practices may opt to schedule follow-up visits for the minor procedure or to sever their relationship with Cigna to get around this administrative burden, Ms. Benson says. Both options constrain patients’ access to timely, continuous care.
She adds that if physicians choose to respond to Cigna’s records requests, they may be financially penalized – in the form of a refund request – for inadequately documenting the reason for the minor procedure.
Cigna did not provide a reason for the policy change in its notification letter to physicians and other health care professionals.
Blue Cross and Blue Shield of Texas also may request medical records and itemized bills from physicians and other health care professionals “to validate the site of service, level of care rendered, and services billed were accurately reported,” according to its clinical payment and coding policy.
UnitedHealthcare policy doesn’t mention medical record requests in the context of office visits with a minor procedure, but Ms. Benson says practices may still see the issue arise.
Practices that have received notice from Cigna or are dealing with negative ramifications related to similar policies can request a coding and documentation review from TMA Practice Consulting. The service includes an in-depth review of medical record documentation and claims coding that identifies deficiencies and areas of risk.
Cigna MA Stars 101 Webinar
NEED A REFRESHER
Register to Join
Cigna MA
Overview of the Stars Program
Cigna’s West Region Stars Team will provide an overview of the Stars Program and available reporting and resources:
- What is the Star Rating and why is it important
- Components of the Star Rating
- A review of available reporting related to Stars
- Tools and Resources available for your office
Event Number: 179 385 5641
Event Password: stars
June 9th, 1:30 CST
Virtual Insurance Cards
With Virtual Insurance Cards on the rise, it can become an issue for your staff at check in.
The usual method of scanning in the insurance card, is not an option with virtual cards.
This may open up the possibility for human error in capturing the data off the card.
One office suggest you have the patient email the card from their phone to the office.
Then the card can be uploaded into the patient chart.
There is a New Player in the Game


EMI Health is proud to provide access to the Aetna network.
Each member will have a medical identification card with the EMI Health and Aetna logos.
Submitting Claim Appeals to Humana

Learn how to use Availity Essentials’ Appeals function to submit appeals and disputes. You can upload needed documentation and check the status of requests that were submitted online.
UHC User Friendly Self Service Resource Guide.

Feel Free to Print and Keep at Your Desk.
The Most Asked Questions About Medical Coding Audits Following the 2021 E/M and MDM Changes ~MGMA
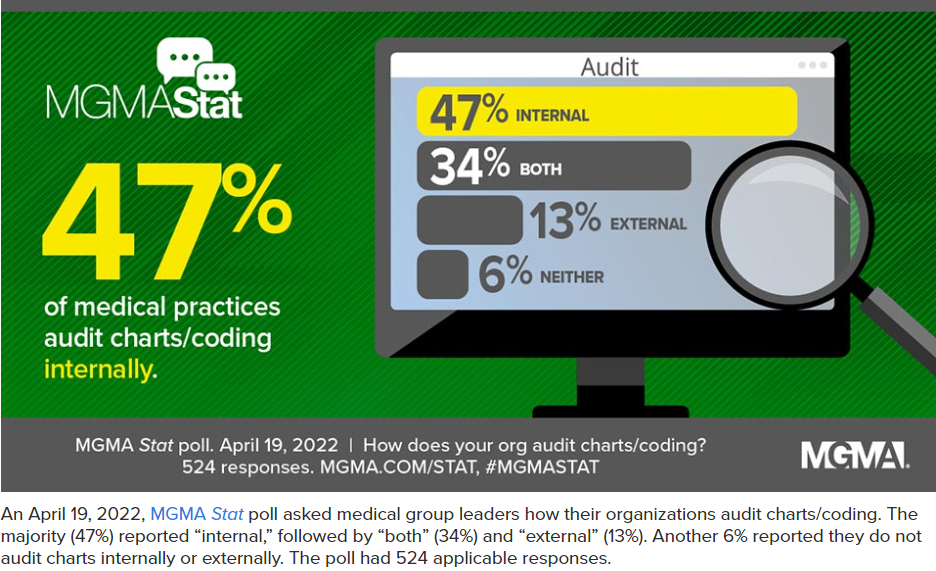
In the above linked article you will find:
- What E/M Updates to Watch
The definition of “external” for purposes of reviewing data as part of MDM.
What is time-based coding?
Documentation Tips
- And More



Recent Comments