Month: January 2023
Billing Codes Reported to Payor May Differ from Codes Authorized.
Have you ever requested authorization on a particular procedure (CPT Code) only to find out afterward there are additional codes or even a totally different CPT code than you requested?
It doesn’t help that only some payors allow for a retro authorization (auth)
and usually they have a short turnaround time.
Below are some tips from the MGMA Community.
From a Surgical Practice:
- Have the Surgical attendee to inform the Prior Auth. Manager or Coder as soon as the procedure is completed.
- The coder should compare procedure notes to the auth prior to billing.
From an ENT Practice:
- Have the physician give you all the possible CPT codes that could be performed and precert. them to be on the safe side.
From a Gastro Practice:
- Again request an auth. for all possible code combinations from the payor.
From an Ortho:
- Create a report that compares billed codes to approved codes.
- Then hold the claim for business days to make certain you have time to reach out to insurers and make adjustments.
- They have found that most insurers want it updated before they process the claim. Which is what the office wants also because it prevents refiling. Even if it takes additional months to get the prior auth. changed.
Summarized:
- Authorize all possible codes for the procedure.
Work with your insurance follow up team to identify our opportunities. This may lead to updates on how you order certain procedures. An update to both system and workflow.
- Timely charge capture. Because retro auth windows are short for some payors, it is imperative to understand if the codes being captured is different from codes authorized.
Same as #1. You have to assess how the charge lag is contributing to the denials.
- A process to compare codes being captured vs authorized and request retro auth.
This concept is for review before charges are submitted. Compare codes in charge sessions vs the codes authorized and flag sessions that have discrepancies so retro auth can be pursued.
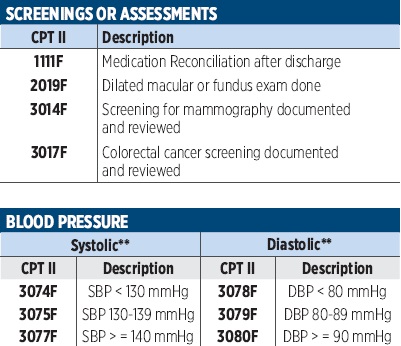
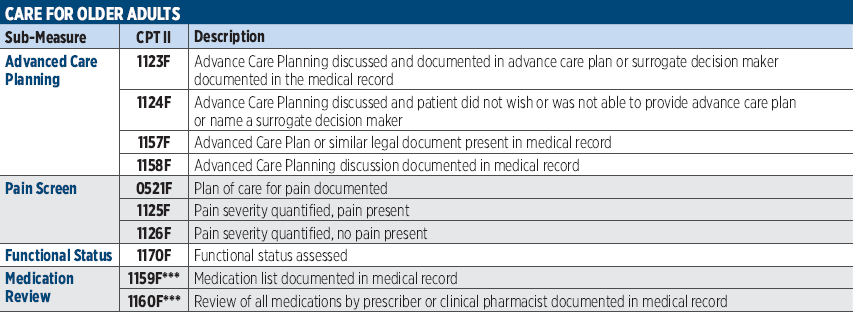
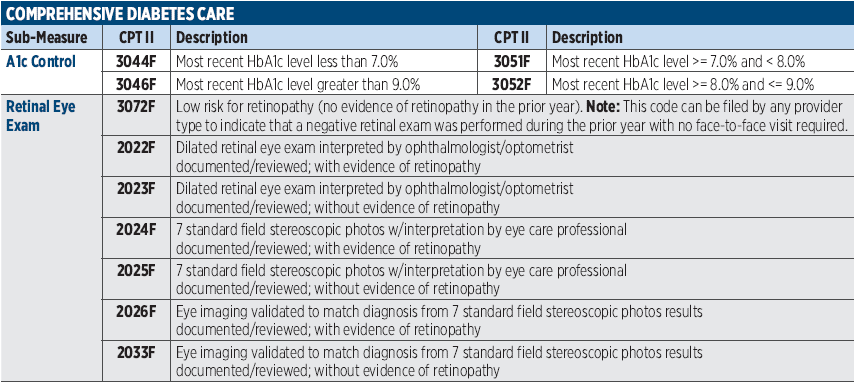
PRINT THIS!
For Easy Access
Click the blue box for a printable download.
Is CIOX a Pain?
If you are having issues with CIOX, please let POET know.
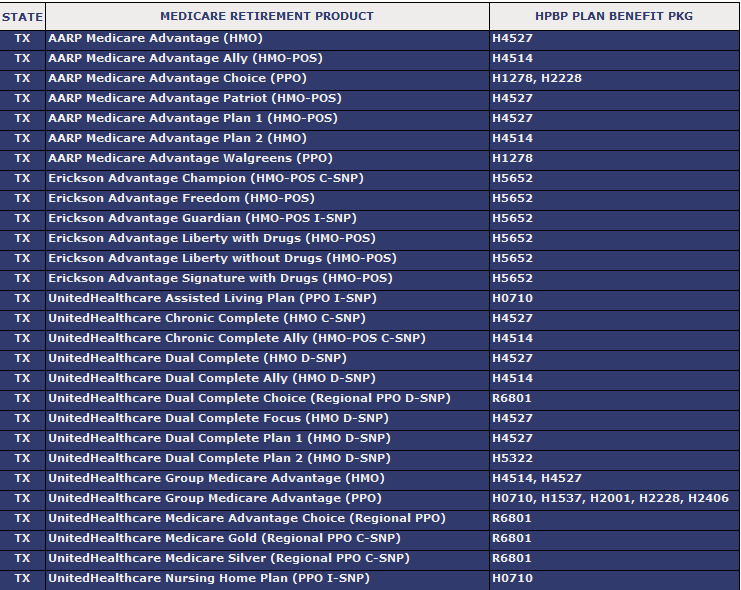
UHC MA Plans

The below list is for Provider use only. Not to be distributed to Patients.
Information Provided by Melissa Boyd, UHC Network Account Manager
Cigna MA Plans for 2023

The below list is for Provider use only. Not to be distributed to Patients.
Know your “H” numbers.
HMO Customer Benefit Plans for Our Service Area
PPO Customer Benefit Plans for Our Service Area
Cigna Preferred Medicare HMO, H4513-061
Cigna True Choice Medicare PPO, H7849-038
Cigna Preferred Savings Medicare HMO, H4513-066
Cigna Tru Choice Medicare PPO, H7849-062
Cigna Courage Medicare HMO, H4513-009
Cigna TotalCare HMO D-SNP, H4513-060
Great News for Insulin Dependent Medicare Patients
In August 2022, the Inflation Reduction Act (IRA) was passed. Among other items it will lower prescription Drug Costs for Seniors.
The Inflation Reduction Act (IRA) will help close the gap in access to medication by improving prescription drug coverage and lowering drug prices in Medicare.
The Law:
- Caps the amount that seniors will have to pay for prescription drugs they buy at the pharmacy at $2000 a year.
- Caps the amount that seniors will pay for insulin at $35 for a month’s supply.
- Provides access to a number of additional free vaccines, including the shingles vaccine, for Medicare beneficiaries.
- Will further lower prescription drug costs for seniors by allowing Medicare to negotiate the price of high-cost drugs and requiring drug manufacturers to pay Medicare a rebate when they raise prices faster than inflation.
From CMS.gov/newsroom, People with Medicare drug coverage will pay nothing out-of-pocket for adult vaccines recommended by the Advisory Committee on Immunization Practices (ACIP), including the shingles and Tetanus-Diphtheria-Whooping Cough vaccines, starting in 2023.
Have You Downloaded 2023 Provider Roster?
This is a great tool for the person in your office that has the responsibility of referrals.
2023 Arcadia 360 Is Up and Running

Medicare Advantage
- The 2023 Arcadia 360 is ready and available for providers. There are no form content changes for 2023 at this time. (Providers have already begun submitting 360s through Arcadia for 2023.)
- One known issue: pre-population from 2022 forms into 2023 forms is not currently working. This will be resolved with a new release coming this week. Exact release details and timing will be communicated once tested and confirmed. This applies to the following fields: past medical history, surgical history, allergies, medications, family history.
- The conditions tab and measures tab will populate with data as expected, if applicable.
Imagine 360 – POET Alert!
Please notify POET if you are having issues of any kind with claims from Imagine 360.
If you have submitted paper or electronic claims to Imagine 360, please check to see if they have been received by them.
Thank You.
Recent Comments