Tag: Policy Updates
UHC Provider Webinar February 26, 2026
- Learn about digital tools to simplify workflow
- Explore UHC plans
- Hear Policy Updates
UHC December Monthly Overview
Key changes for our Medicare Advantage plan
- In 2026, most UnitedHealthcare Medicare Advantage health maintenance organization (HMO) and point of service (POS) plans are referral plans. You can check plan referral requirements online.
- Starting Jan. 1, 2026, most members enrolled in UnitedHealthcare Medicare Advantage HMO/POS plans will be required to obtain a referral from their primary care provider (PCP) before accessing certain specialist services in outpatient, office or home settings. Referrals must be submitted by the PCP to UnitedHealthcare prior to the specialist visit. This also applies when members of HMO/POS plans are traveling and accessing the National Network. Learn more in our 2026 Medicare Advantage Referral Requirements Guideopen_in_new.
- Effective Jan. 1, 2026, new or existing members of UnitedHealthcare SNPs, including Chronic Special Needs Plans (C-SNP) and Dual Special Needs Plans (D-SNP), need a qualifying chronic condition to access benefits that cover healthy food and/or utilities. Providers may be contacted by UnitedHealthcare to verify a member has at least one qualifying condition to receive benefits. See 2026 Medicare Advantage, CSNP & DSNP Plan Overview Courseopen_in_new for more information.
UHC November Update
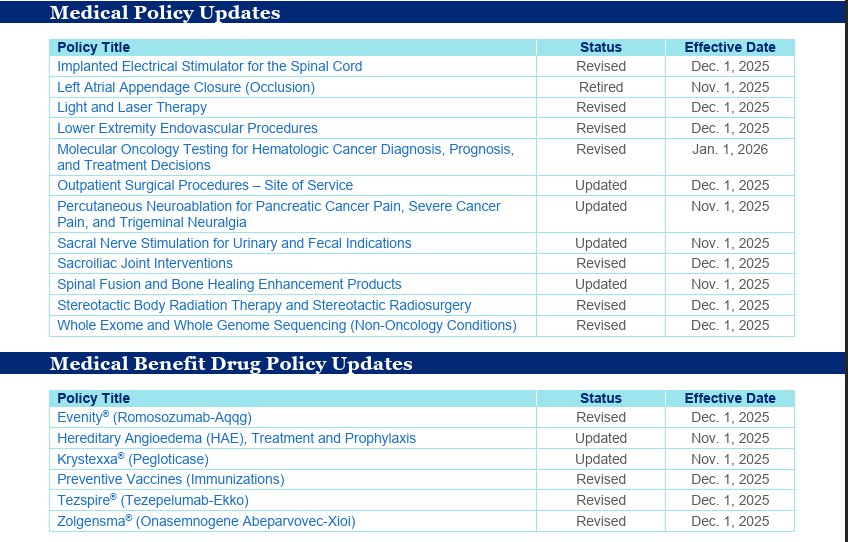
A list of recently approved, revised, and/or retired Medical Policies and/or Medical Benefit Drug Policies is provided below for your reference. For a comprehensive summary of the latest updates, refer to the Medical Policy Update Bulletin: November 2025.
UHC July Overview
Policy and protocol updates
Medical policy updates
Medical policy updates for July 2025 for the following plans: Medicare, Medicaid, Exchanges and commercial.
Reimbursement policy updates
See the latest updates for reimbursement policies.
Specialty Medical Injectable Drug program updates
See the latest updates to requirements for Specialty Medical Injectable Drugs for UnitedHealthcare members.
Pharmacy and clinical updates
Access upcoming new or revised clinical programs and implementation dates for UnitedHealthcare plans
Call Now to Reserve Your Seat
Limited Seating
2025 Washington Policy Mid-Year Update – MGMA Webinar
Where: POET Office
When: July 22, 2025, Tuesday
Time: 12 noon
Lunch will be served
Limited Seating Available
During this webinar, MGMA Government Affairs staff will provide an update on current and potential policy developments impacting medical group practices. The speaker will discuss the latest legislative and regulatory issues covering topics such as Medicare reimbursement, telehealth, quality reporting, and surprise medical billing.
This 60-minute webinar will provide you with the knowledge to:
Identify key regulatory developments
Discuss legislative issues impacting medical groups
Describe MGMA advocacy initiatives
Please call (936) 637-7638 or Email [email protected]
UHC Network News August Edition
To view these updates, click the blue button to the right.
Cigna Denies Claims without Z-Code
Starting July 14th
Cigna Healthcare will deny certain claims that are billed with a Z-code and without documentation. A move that could add to your administrative burden.
Cigna will deny claims when practices bill certain evaluation and management (E/M) codes (99202-99215) with a preventive service code and a supporting Z diagnosis code – but not supplemental medical record documentation.
Physicians will need to refer to multiple policies by the payer to utilize both preventive services and problem-oriented E/M services for new and established patients on the same date of service, which Texas Medical Association billing and code experts caution could add to practices’ workload. Moreover, these services will not be payable by Cigna when billed with a Z diagnosis code alone.
TMA experts recommend including supporting medical record documentation with the diagnosis code for the problem E/M claim to identify why a preventive service – like dietary counseling, for example – was performed.
Physicians can also check Cigna’s preventive services policy for examples of Z codes or refer to Cigna’s E/M Reimbursement Policy for more payment information from the payer.
Cigna Provider Newsroom
WEBINAR SCHEDULE FOR DIGITAL SOLUTIONS: You’re invited to join interactive, web-based demonstrations of the Cigna for Health Care Professionals website (CignaforHCP.com). Learn how to navigate the site and perform time-saving […] Read more >
CLINICAL, REIMBURSEMENT, AND ADMINISTRATIVE POLICY UPDATES: To support access to quality, cost-effective care for your patients with a medical plan administered by Cigna Healthcare, we routinely review clinical, reimbursement, and administrative […] Read more >
COORDINATION OF CARE: Coordination of care is the process by which a patient’s team of providers cooperatively help coordinate care management and ensure access to quality, cost-effective care. […] Read more >

Recent Comments