Month: November 2024
TMA Webinar Helps Equip Physicians for 2025
Medicare Fee Schedule
With the Centers for Medicare & Medicaid Services’ (CMS’) 2025 Medicare Physician Fee Schedule set to take effect Jan. 1, the Texas Medical Association is preparing physicians for changes in payment and coding, telemedicine, and quality and value-based care arrangements, among other areas.
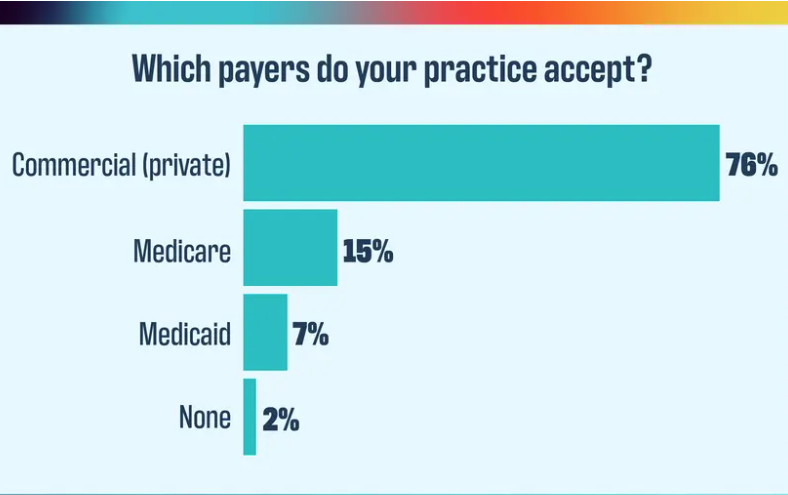
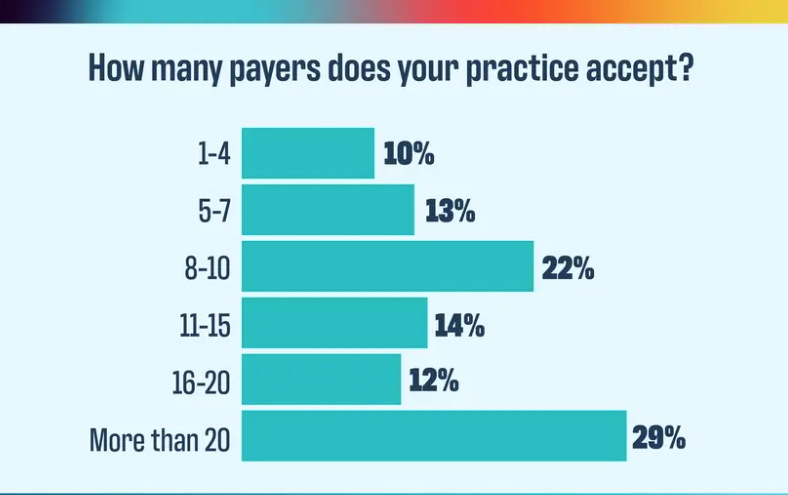
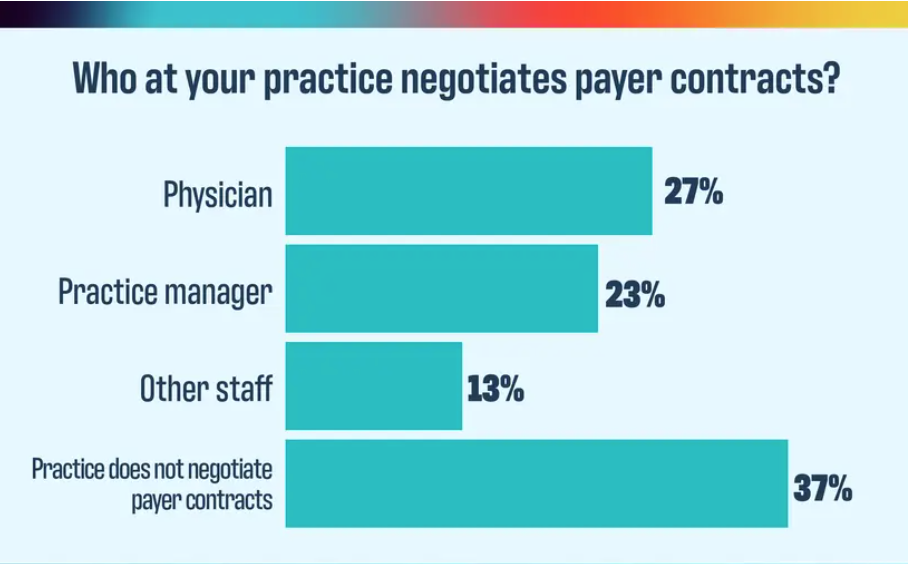
2024 Payer Scorecard: How payers are failing practices and patients
Physicians Practice: November 11, 2024, By Keith A Reynolds

How would you characterize your prior authorization experience in the last year?
We’re doing more prior authorizations
74%
We’re doing fewer prior authorizations
4%
Prior authorizations are about the same
22%

Do you think there should be a CPT code requiring payers to reimburse for prior authorization work?
Yes
97%
No
3%



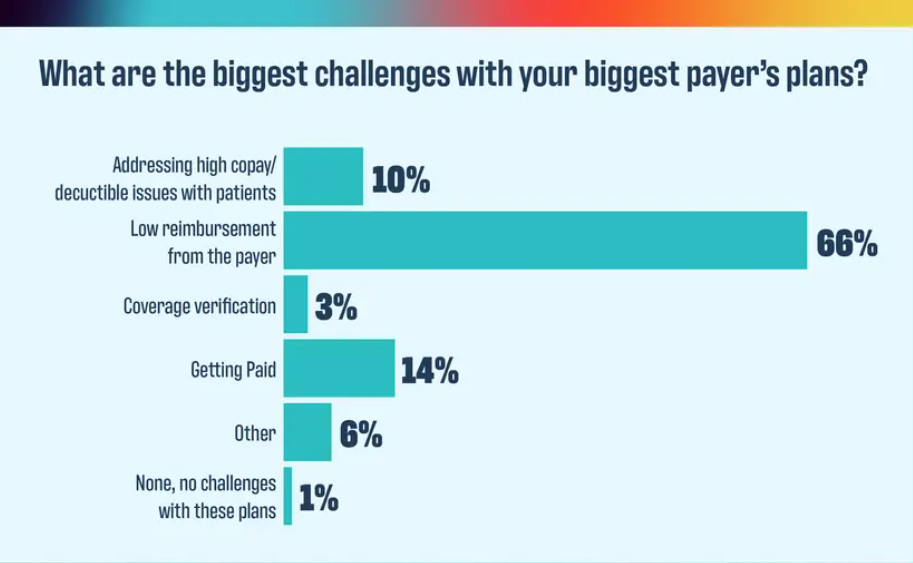
What is your biggest challenge with your biggest payer?
- Current systems don’t interact well with our billing systems requiring office staff to correct claims leading to delayed payment
- Reimbursement stinks. I Quit !!!!!!
- Staff the insurance companies contracted are mostly out of the country and do not know the issues we have and do not like to refer the questions or specific issues to any expert in the field.
- Small practice is ignored. They would not negotiate fees. For more than 15 years no increase in fees, only steady decrease. It is a shame, no respect any longer for providers.
- Prior authorizations waste so much time for what should be a simple process
- Lack of urgency or even motivation to provide basic service
The verdict is in for how practices feel about their payers, and it isn’t good.
How can payers improve their relationship with practices?
- Streamline systems to allow for clean claims the first time
- Have a dedicated Provider Relations contact so we know who to talk to, and who to call to get responses to critical questions, not have to send emails to faceless representatives that have a low rate of resolution.
- Communicate. Show WHY they deny, and what EXACTLY can be done to help the patients who pay them. Do not simply deny with NO guidance.
- Pay us enough to survive. Instead, they raise hospital payments. Paying us more so we could hire more doctors and physicians assistants and keep people OUT of those hospitals.
- Stop putting technology problems and carrier losses on the provider and their patients.
- Instead of looking at me as an expense, look at me as a tool to care for their beneficiaries.
- Stop requiring PAs for generic meds and obviously necessary medications.
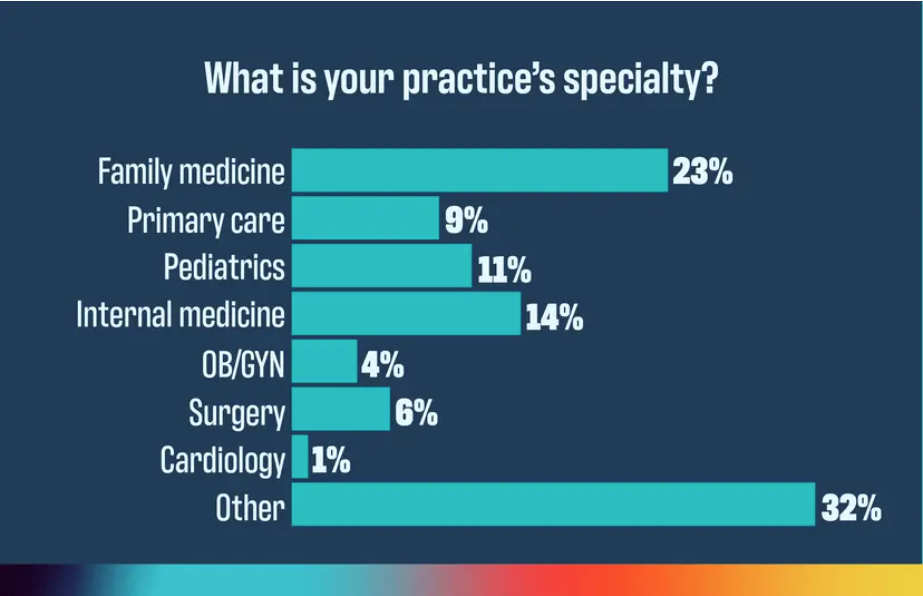
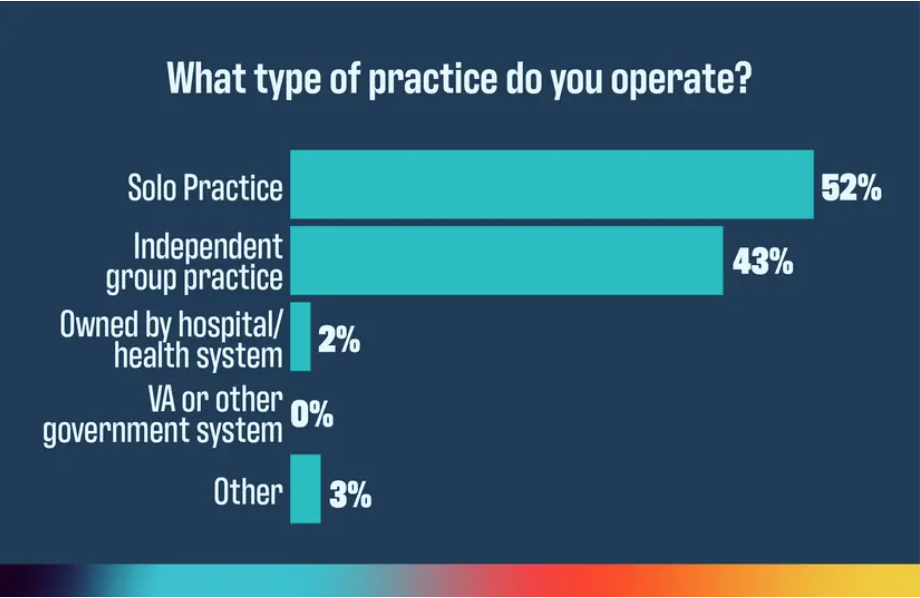
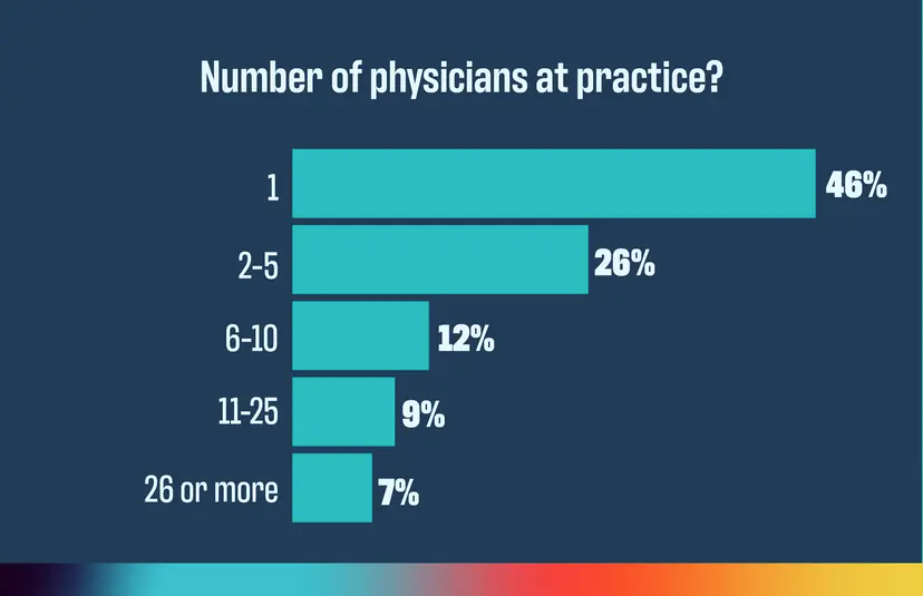
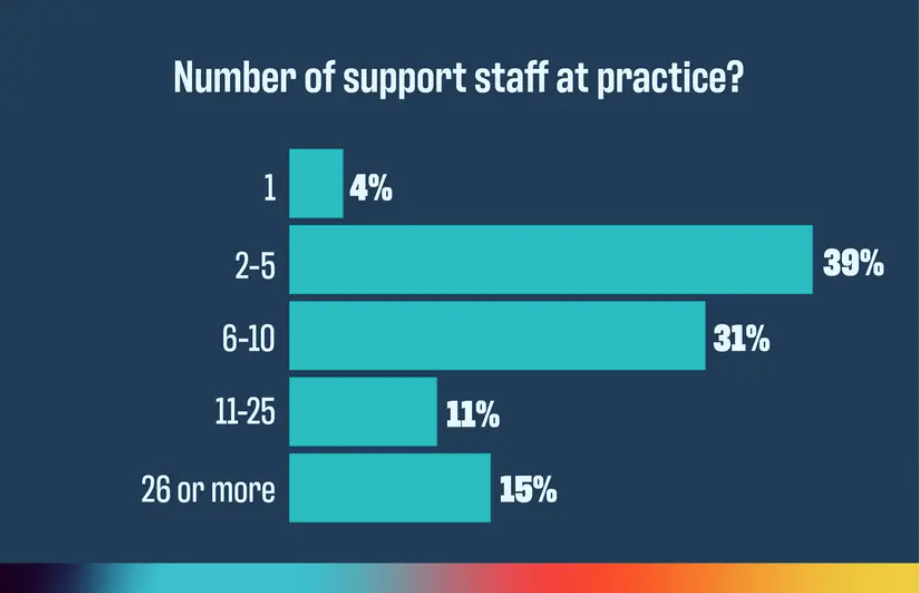
Medicare Solidifies Pay Cut
In a final rule that solidifies a nearly 3% Medicare pay cut for physicians in 2025, the Centers for Medicare & Medicaid Services (CMS) also set the trajectory for physician practices over the next year with a mixed bag of changes related to telemedicine, coding and payment, and the Merit-Based Incentive Payment System (MIPS), among others. ~By Phil West
While TMA analyzes what it sees as some isolated, positive changes resulting from CMS’ finalization of the 2025 Medicare Physician Fee Schedule, it is also urging physicians to act now to show their support for House Resolution 10073
Recent Comments