Month: March 2024
Termination of Employee
No matter how much time we spend vetting potential hires, eventually, someone isn’t going to work out.
Regardless of the reason, there will come a time when an employee needs to be let go. These decisions are difficult, but the change needs to be made for the long-term benefit of the practice and the other employees.

Reduced 2024 Medicare Physician Pay Cut Now in Effect.
Thanks to the passage of a new federal spending bill, the 3.4% Medicare physician pay cut that took effect on Jan. 1 was reduced to 1.68% as of March 9. This reduced cut and the corresponding new conversion factor of $33.2875 will remain in effect through Dec. 31.
Change Healthcare Update
In its latest update on the response to the cyberattack on Change Healthcare, UnitedHealth Group said that its largest clearinghouse, called Relay Exchange, will be back online by the end of the weekend and the company will begin processing $14 billion in medical claims.
“Once a critical mass of payer connectivity has been established, we will turn on claims processing for Assurance customers. That process will occur automatically for those Assurance customers when we trigger restart,” UnitedHealth said in its update. “Following activation of Assurance software customers, we will turn our attention to the reactivation of all other Relay Exchange claims submitters. Throughout the reactivation of these provider customer groups, we will continue to add additional payer connectivity to close any remaining gaps. We will start immediately with establishing payer connectivity so claims entering the clearinghouse have a destination.”
The company is targeting the week of April 1 to restore its clinical exchange service, payer connectivity and hosted payer services.
The following week, April 8, the company plans to restore its Risk Manager and Health QX products.
Change to Release Medical Claims Software
On March 18th UnitedHealth Group said they had begin to release medical claims preparation software, a move it says is a critical step in restoring services.
The software will be rolled out to thousands of customers in the next several days, according to the announcement. UHG said that it intends to have third-party attestations available before services are fully online.
Change Healthcare’s electronic payments platform was brought back online as of March 15, and UHG is now “proceeding with payer implementations.
The insurer has also suspended prior authorizations for outpatient care, and is reviewing similar steps for inpatient admissions in Medicare Advantage
Aetna March OfficeLink Updates
Changes in Aetna’s Commercial Drug List Begin on July 1, 2024.
Per Aetna, Changes may affect all drug lists, precertification, step therapy and quantity limit programs. Physician offices can view the changes as early as May 1, 2024. The changes can be found on Aetna’s Formularies and Pharmacy Clinical Policy Bulletins page.
Changes in Aetna’s National Precertification List (NPL)
This applies to both Aetna Commercial and Medicare Members. (POET does not have an Aetna Medicare contract at this time.) Per Aetna this change will also be effective July 1, 2024. They will require precertification for:
- Osteotomy posterolateral approach, thoracic
- Osteotomy anterior approach
- Knee meniscectomy-requires precertification for the Medicare Advantage members only.
Per Aetna, Be sure to submit precertification requests at least two weeks in advance. To save time, request precertification on line.
Optum Temporary Funding Assistance
The Temporary Funding Assistance Program is designed to help bridge the gap in short-term cash flow needs for providers impacted by the disruption of Change Healthcare’s services.
Eligible providers:
- Providers who receive payments from payers that are processed by Change Healthcare.
- UnitedHealthcare medical, dental and vision providers.
- Providers who have exhausted all available connection options or may be in the process of implementing technical workaround solutions and who work with a payer who has opted not to advance funds to providers during the period when Change Healthcare systems remain down
For questions contact (877) 702-3253
Your Mac is Novitas Solutions
Today, HHS is announcing immediate steps that the Centers for Medicare & Medicaid Services (CMS) is taking to assist providers to continue to serve patients. CMS will continue to communicate with the health care community and assist, as appropriate. Providers should continue to work with all their payers for the latest updates on how to receive timely payments.
Medicare providers needing to change clearinghouses that they use for claims processing during these outages should contact their Medicare Administrative Contractor (MAC) to request a new electronic data interchange (EDI) enrollment for the switch. The MAC will provide instructions based on the specific request to expedite the new EDI enrollment. CMS has instructed the MACs to expedite this process and move all provider and facility requests into production and ready to bill claims quickly. CMS is strongly encouraging other payers, including state Medicaid and Children’s Health Insurance Program (CHIP) agencies and Medicaid and CHIP managed care plans, to waive or expedite solutions for this requirement
CMS has contacted all of the MACs to make sure they are prepared to accept paper claims from providers who need to file them. While we recognize that electronic billing is preferable for everyone, the MACs must accept paper submissions if a provider needs to file claims in that method.
Novitas Phone # (855) 252-8782. Have your PTAN and the last 5 of your TIN.
Change HealthCare!

Looking for answers? So is POET. We are looking for work-arounds. Hopefully we will have some up before closing today.
POTENTIAL SCAM Regarding Cigna MA
If you receive a fax from Cigna MA , like either of the below,
DO NOT RESPOND

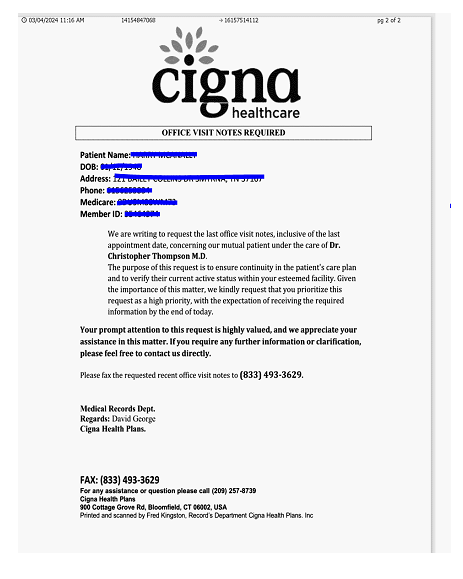
This is a scam.
If you do receive one, please send a short email to Jim with Cigna MA, to make him aware.




Recent Comments