Tag: UnitedHealthcare (UHC)
UHC Provider Webinar February 26, 2026
- Learn about digital tools to simplify workflow
- Explore UHC plans
- Hear Policy Updates
UHC December Monthly Overview
Key changes for our Medicare Advantage plan
- In 2026, most UnitedHealthcare Medicare Advantage health maintenance organization (HMO) and point of service (POS) plans are referral plans. You can check plan referral requirements online.
- Starting Jan. 1, 2026, most members enrolled in UnitedHealthcare Medicare Advantage HMO/POS plans will be required to obtain a referral from their primary care provider (PCP) before accessing certain specialist services in outpatient, office or home settings. Referrals must be submitted by the PCP to UnitedHealthcare prior to the specialist visit. This also applies when members of HMO/POS plans are traveling and accessing the National Network. Learn more in our 2026 Medicare Advantage Referral Requirements Guideopen_in_new.
- Effective Jan. 1, 2026, new or existing members of UnitedHealthcare SNPs, including Chronic Special Needs Plans (C-SNP) and Dual Special Needs Plans (D-SNP), need a qualifying chronic condition to access benefits that cover healthy food and/or utilities. Providers may be contacted by UnitedHealthcare to verify a member has at least one qualifying condition to receive benefits. See 2026 Medicare Advantage, CSNP & DSNP Plan Overview Courseopen_in_new for more information.
UHC November Update
A list of recently approved, revised, and/or retired Medical Policies and/or Medical Benefit Drug Policies is provided below for your reference. For a comprehensive summary of the latest updates, refer to the Medical Policy Update Bulletin: November 2025.
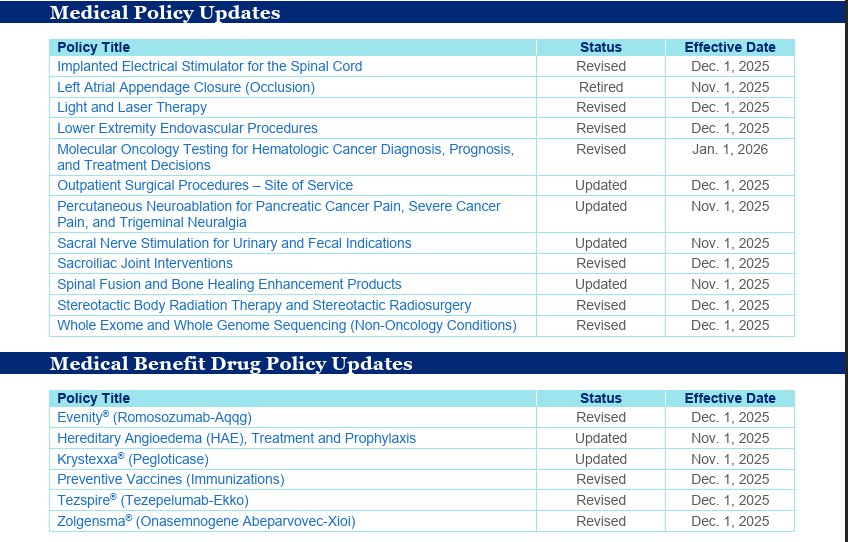
UHC “Check by Member” Authorization Tool
UHC says they have a smarter way to check prior authorization requirements.
Our upgraded Check by Member tool is now the most accurate and reliable way to confirm prior authorization requirements.
- Personalized results based on member-specific data
- Same trusted source as our phone advocates
- Instant answers with no hold time
TRS 2025-2026 Plan Year
Products for 2025-2026 Plan Year
Please be aware the Retiree Plans are Calendar Year
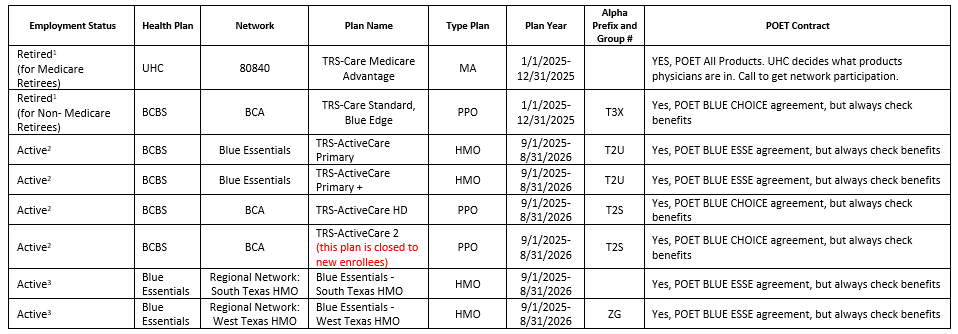
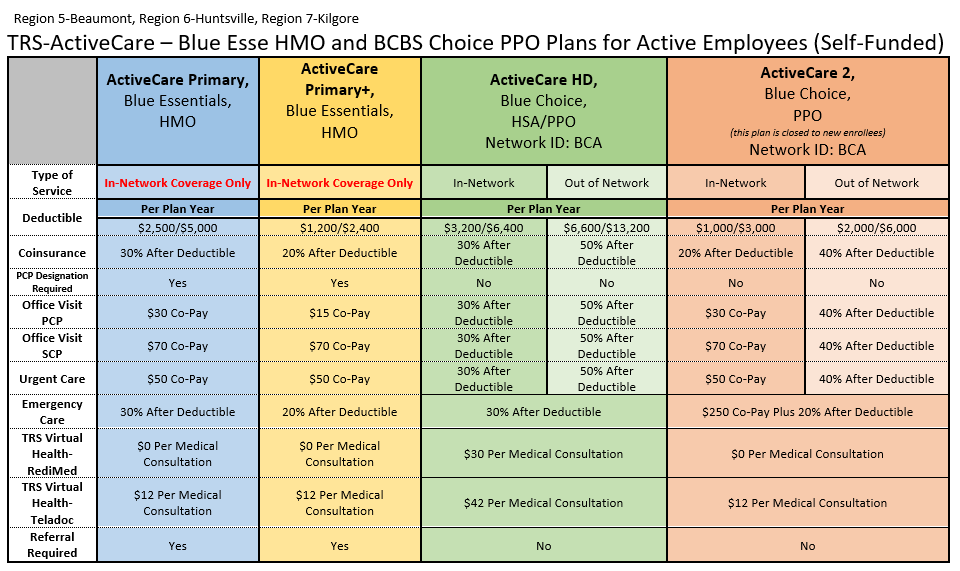
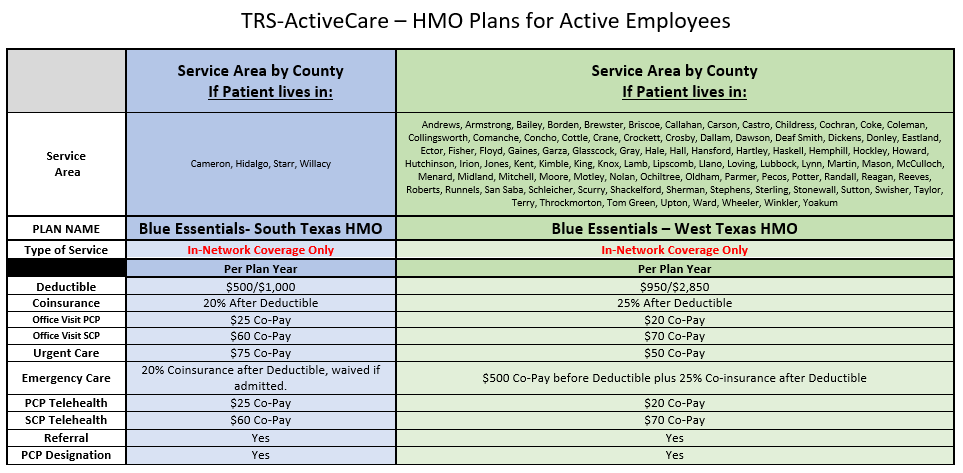
Health Plan Representatives Updated 8/4/2025
The Health Plan Representatives List has been updated. This is a good tool to print and have close by when you have an issue.
The biggest change for claims issues will be HealthSpring (HCSC) formerly Cigna MA. Here is how:
- Email ALL claims issues to [email protected]
2. HealthSpring has supplied the spreadsheet that MUST be used. A link is provided below, or you may call POET, we will be glad to email you an electronic copy.
Only the columns with Red Lettering, need to be filled out by the Physician’s office.
4. Always feel free to copy [email protected] if you would like POET to be in the loop.
5. If you have a time sensitive, special, or just an issue you would like to discuss with POET, please call (936) 637-7638.
Check Your Gold Card Eligibility
Last fall, UHC introduced the first national Gold Card program, reducing prior authorizations in favor of advance notification for provider groups consistently adhering to evidence-based care guidelines. They are happy to announce that in the 2nd year of the program, starting Oct. 1, 2025, additional provider groups will be eligible.
On Sept. 1, UHC will publish details on how to determine if your provider group has qualified for the program.
Check your Gold Card eligibility status starting Sept. 1
Provider groups can view their Gold Card program status in the UnitedHealthcare Provider Portal.
Renewing Oct. 1, 2025, the program simplifies the prior authorization process for qualifying providers and eligible services. Qualifying providers will need to submit advance notification, which confirms eligibility and network status, but no clinical information will be requested. We’ve updated the program protocol for the renewal period.
Visit our national Gold Card program page in September for detailed instructions on how to identify Gold Card status and access to an interactive guide that can help you navigate our resources.
UHC July Overview
Policy and protocol updates
Medical policy updates
Medical policy updates for July 2025 for the following plans: Medicare, Medicaid, Exchanges and commercial.
Reimbursement policy updates
See the latest updates for reimbursement policies.
Specialty Medical Injectable Drug program updates
See the latest updates to requirements for Specialty Medical Injectable Drugs for UnitedHealthcare members.
Pharmacy and clinical updates
Access upcoming new or revised clinical programs and implementation dates for UnitedHealthcare plans
UHC Claims their new API makes work easier.
UnitedHealthCare’s Application Program Interface (API) is a free digital solution that automates everyday work.
Benefits of using API
- Reduces phone calls and paper
- Automates transactions on your timetable
- Distributes data faster to where you need it
- Get real‑time information
- Supports standard formats and compatible with new technology
- Maximizes efficiency and productivity through workflow integration
Why add API to your practice?
- Flexibility: Allows you to choose the data and API that fit your needs.
- Automation: Incorporates seamlessly into your workflow.
- Security: Ensures data is accessed and transferred securely
UHC Major Data Breach
Just four months after the Change Cyberhack, UnitedHealth Care is hit again.
Community Health Centers (CHC), has disclosed a major data breach. CHC has revealed that a “substantial quantity of data” was stolen, impacting a “substantial proportion of people in America.” UnitedHealth’s CEO Andrew Witty estimated one-third of all Americans have been affected by the breach. That is over 111 million people.
“While CHC cannot confirm exactly what data has been affected for each impacted individual, information involved may have included contact information (such as first and last name, address, date of birth, phone number and email.
This means that millions of individuals could be at risk of identity theft and other forms of fraud.
Recent Comments