Category: Uncategorized
ERISA Plan vs. Third-Party Administrator (TPA)
🎯 ERISA Plan vs. Third-Party Administrator (TPA)
They’re not the same thing — and mixing them up causes a LOT of confusion.
🌈 Think of it like this:
🏛️ ERISA Plan = The Rulebook
This is the actual health plan created by the employer.
It spells out:
✔️ What’s covered
✔️ What’s excluded
✔️ How claims should be paid
✔️ Who has final authority
📌 The employer owns the ERISA plan and carries the responsibility.
⚙️ Third-Party Administrator (TPA) = The Referee
They simply:
✔️ Process claims
✔️ Apply the plan rules
✔️ Handle paperwork & customer service
📌 The TPA follows the rules — they don’t make them
💡 Why this matters:
👉 An ERISA plan can change TPAs
👉 A TPA cannot change the ERISA plan
👉 Coverage decisions come from the plan document, not the administrator
✨ Bottom line:
🧠 ERISA Plan = The Authority
🛠️ TPA = The Administrator
Understanding the difference protects employers, providers, and members alike.
Disclaimer: The information provided in this blog is for general educational purposes only. While Ink strives to explain insurance concepts accurately and clearly, payer rules, contracts, and policies can vary widely by plan, state, and provider agreement—and they change frequently.
This content should not be interpreted as definitive guidance or a substitute for reviewing payer manuals, contracts, or official communications. Physician offices are encouraged to conduct their own research and verify requirements directly with the applicable insurance carriers before making operational or billing decisions
UHC Community Plan Policy Update Feb. 2026

For a comprehensive summary of the latest updates, refer to the Medical Policy Update Bulletin: February 2026
Medical Policy Updates:
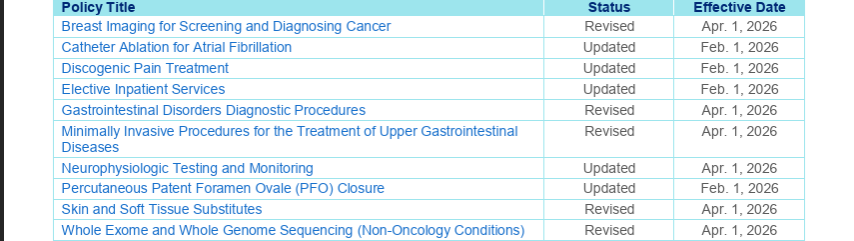
Medical Benefit Drug Policy Updates:

Sorry POST Missing
POET ask you to forgive us. The post in the “Latest Post” email titled “If you think 2024 was good” had to be taken down. The video of October 2024 festivities was causing a gliche.
BUT….. If you like old abandoned hospitals……

Come see 2025
HealthSpring Rollout
■ Important Updates for Physician Offices-New Plans Coming in 2026
New benefit plans under the HealthSpring name will roll out January 2026. For now, you can find articles about these changes on: MedicareProviders.Cigna.com …and in the Provider Newsroom.
■ Claims Contact Information
Jim Denman will no longer handle claims.
For more information, please call POET
■ Goodbye HSConnect – Hello Availity Essentials
Cigna MA has partnered with Availity Essentials for enhanced online tools. HSConnect and Cigna for HCP are no longer needed.
■ Verify eligibility & benefits
■ Verify primary care provider
■ View customer ID cards
■ View maximum-out-of-pocket amounts
■ Submit professional & institutional claims
■ Check claim status
■ View remittance advice
■ Access Cigna MA links (including prior authorizations & resources) via the Payer Space page

What is the Security Rule Anyway?
The Security Rule specifically sets out to ensure the “confidentiality, integrity,
and security” of electronic protected health information (ePHI). What does that mean?
• Confidentiality: ePHI is not available or disclosed to unauthorized persons.
• Integrity: ePHI is not altered or destroyed in an unauthorized manner.
• Availability: ePHI is accessible and usable on demand by an authorized person.
Physician Directory and Provider Roster Update

Help Yourself! Feel Free To Print!
Great Resource Tools!
- Click on the “files” tab.
- Open the “Current information” folder.
- Choose the document you would like to print.
- Click the arrow in the box (top right of document).
- When it opens tell it to print.
POET Phones Are Down
Please Email if you need us.
Updated 4/11/2024. We are back up and running. Please forgive us for any inconvenience.
Superior Formulary Changes
Medicaid and CHIP Program Revalidation
IMPORTANT:
During the Public Health Emergency (PHE), Provider
Revalidation was waived by HHSC.
The PHE ended May 11, 2023
Beginning May 12, 2023, Provider Revalidation Requirements were resumed.
Providers must ensure Medicaid and/or CHIP enrollment revalidation is completed on or before the provider’s scheduled revalidation date.
Providers that do not complete the revalidation process by their deadline are DISENROLLED from all Texas state healthcare programs, including Medicaid and/or CHIP managed care programs.
Visit the Texas Medicaid & Healthcare Partnership (TMHP) Provider Enrollment webpage to view and confirm your upcoming Medicaid and /or CHIP program revalidation date, verify current enrollment is active and verify all information in the PEMS system is accurate.

Recent Comments