Tag: Superior
Superior PCP Change Request Form

I didn’t know?
How was I supposed to know?
We all know it is going to happen. The PCP on the card is not yours. And know one knew.
But Superior has made it a little easier. No setting on hold.
Help the patient fill it out.
For Star Health, fax the completed form to (866) 626-6069.
For all others, fax to (866) 918-4447.
Superior HealthPlan Billing Changes
Important Provider Update
Effective September 1, 2025
The Texas Health and Human Services Commission (HHSC) will transition Medicaid-only services for dually eligible clients (eligible for both Medicare and Medicaid) from Fee-for-Service (FFS) to a Managed Care service delivery system.
Superior HealthPlan will be responsible for adjudicating these claims.
Provider Responsibilities
Submit claims for Medicaid-only services for dual eligible clients directly to the Managed Care Organization (MCO).
If a Claim is Sent to TMHP in Error:
TMHP will forward the claim to the correct MCO.
The TMHP response will only confirm forwarding – no ER&S report will be issued.
Claims with dates of service on or after Sept. 1, 2025 will not be adjudicated by TMHP.
Provider Action Steps
✅ Submit Medicaid-only service claims directly to the MCO.
✅ Contact the MCO for claim status and adjudication questions.
✅ Review the Rider 32 Procedure Code List (PDF) for impacted services.
✅ Reach out to your Provider Representative via the Find My Provider Representative webpage.
Need Help?
Contact your dedicated Provider Representative

Health Plan Representatives Updated 8/4/2025
The Health Plan Representatives List has been updated. This is a good tool to print and have close by when you have an issue.
The biggest change for claims issues will be HealthSpring (HCSC) formerly Cigna MA. Here is how:
- Email ALL claims issues to [email protected]
2. HealthSpring has supplied the spreadsheet that MUST be used. A link is provided below, or you may call POET, we will be glad to email you an electronic copy.
Only the columns with Red Lettering, need to be filled out by the Physician’s office.
4. Always feel free to copy [email protected] if you would like POET to be in the loop.
5. If you have a time sensitive, special, or just an issue you would like to discuss with POET, please call (936) 637-7638.
Superior: New Availity Claim Features and Webinars.
|
Superior: Appeal Submissions
IMPORTANT: Post-Service Medical Necessity Appeal Submissions
Superior HealthPlan would like to remind providers that post-service Medical Necessity Appeals must be mailed or faxed using the submission information below. Submissions must include the reason for appeal and any additional clinical information for appeal review..
Centene Management Company
ATTN: Medical Management Appeals
5900 E. Ben White Blvd
Austin, Texas 78741
Fax number: 1-866-918-2266
Post-service appeals for reconsideration of a Medical Necessity Denial on behalf of a member should not be sent to the Claims Appeal address.
For questions about post-service Medical Necessity Appeals, providers can contact 1-877-398-9461.
Prior Auth for Certain Sleep Studies, No Longer Required by Superior as of April 1, 2025.
For all Medicaid (STAR, STAR Health, STAR Kids, STAR+PLUS), CHIP and Ambetter from Superior HealthPlan members, Superior will no longer require prior authorization for the following Current Procedural Terminology (CPT) codes:
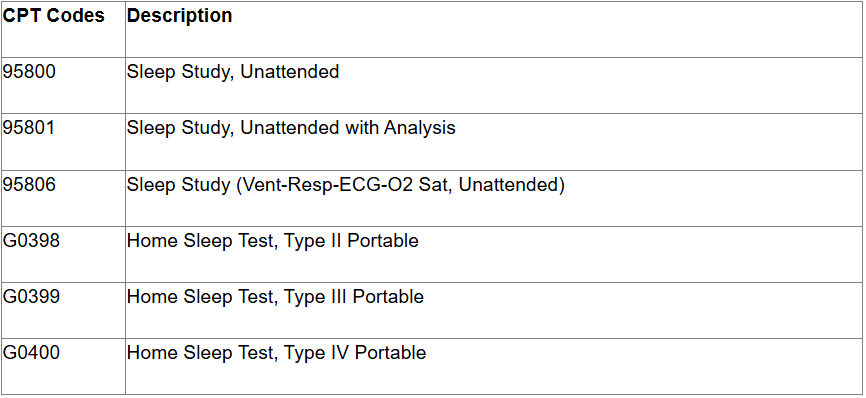
For Medicaid, CHIP and Ambetter members 17 years of age and younger, Superior will no longer require prior authorization for the following CPT codes:

Co-pays Resuming for Certain Services

Effective 10/1/24: Co-pays will Resume for CHIP CoVid19 Services.
During the COVID-19 public health emergency, the Texas Health and Human Services Commission (HHSC) waived co-pays for COVID-19 vaccines, testing, and treatment for Children’s Health Insurance Program (CHIP) members. This waiver will end on September 30, 2024
Providers may begin collecting co-pays for COVID-19 vaccines, testing, and treatment rendered to CHIP eligible members for dates of service on or after October 1, 2024.
Providers may not charge co-pays for mental health and substance use disorder outpatient office visits
Co-pays have been permanently removed for mental health and substance use disorder outpatient office visits to comply with federal regulations.
Superior Records Retrieval Project
It is always good to know things before they occur. But often we are scrambling for information after the fact.
NOT THIS TIME
Superior gives us a Heads Up.
Superior is requesting your cooperation in providing access to specific member records to facilitate a Risk Adjustment chart review. Risk Adjustment is the payment methodology used by CMS and HHS for Wellcare By Allwell and STAR+PLUS Medicare-Medicaid Plan.
The purpose of these chart reviews is to verify that information reported to Superior, and ultimately to CMS and HHS via claims or encounter data, includes all pertinent diagnosis codes at accurate levels of specificity.
Please Note: Superior has executed a Business Associate Agreement with both Advantmed and Datavant (formerly CIOX Health).
Advantmed and Datavant have been engaged by Superior to retrieve medical records selected as part of this chart review. Any information shared during this review will be kept in the strictest of confidence, in accordance with all applicable state and federal laws regarding the confidentiality of patient records, including current HIPAA requirements. Superior appreciates your cooperation with this and will work with you to minimize disruptions in member care.
You will have the option to submit medical records in the following ways:
- Secure email
- Fax
- FedEx
- Remote Electronic Medical Record (EMR) download
AND
- Onsite scanning performed by an Advantmed medical record technician
Tell your staff to anticipate a call or fax from Advantmed or Datavant to schedule the medical record retrieval in the upcoming weeks.
For any questions, please email [email protected]
Recent Comments