Category: Medicare
HS
Updates for HealthSpring providers | |
We’re changing prior authorization requirements that may apply to some HealthSpring Medicare Advantage members. Changes are based on updates from utilization management prior authorization assessment, Current Procedural Terminology (CPT®) code changes released by the American Medical Association or Healthcare Common Procedure Coding System code changes from the Centers for Medicare & Medicaid Services. For some services and members, prior authorization may be required through HealthSpring utilization management, and related services for Medicare Advantage members will be reviewed by HealthSpring and EviCore healthcare. | |
These changes begin July 1, 2026: · Implementation of Part B Step Therapy Program · Addition of orthotic codes to be reviewed by HealthSpring · Addition of new Medicare Advantage Prescription Drug plan codes to be reviewed by HealthSpring | |
For more information, refer to the prior authorization requirements list on the clinical review page. Always check eligibility and benefits first through Availity® Essentials or your preferred vendor prior to rendering services. This step will confirm prior authorization requirements and utilization management vendors, if applicable. Checking eligibility and/or benefit information and/or obtaining prior authorization is not a guarantee of payment. Benefits will be determined once a claim is received and will be based upon, among other things, the member’s eligibility, and the terms of the member’s evidence of coverage. If you have any questions, call the number on the member’s ID card. Services performed without required prior authorization or that do not meet medical necessity criteria may be denied for payment, and the rendering provider may not seek reimbursement from the member. | |
Thank you for your partnership. | |
CPT copyright 2025 American Medical Association. All rights reserved. CPT is a registered trademark of the AMA. | |
HealthSpring products and services are provided exclusively by or through operating subsidiaries of Health Care Service Corporation, a Mutual Legal Reserve Company. PO Box 20002, Nashville, TN 37202 © Copyright 2026 Health Care Service Corporation. All Rights Reserved. |
Arcadia 360 User Guide 4/2/26, HealthSpring

Effective 4/2/26, in accordance with HCSC’s coding policies and guidelines, the Arcadia 360 and Arcadia HMR have been updated to account for the required documentation of specified medications within the treatment plan of active conditions.
- Arcadia 360: upon selecting Active Condition in the 360, a “notes” field will appear. It will be required in addition to the one word treatment plan.
- If an end user selects “Medication” as the treatment plan, the notes field should be used to document the specific medication being used as treatment for that specific condition.
- If an end user selects any other option as the treatment plan, the notes field should be used to provide more MEAT criteria to substantiate the condition being actively treated.
- Arcadia HMR: the medication should be written in along with the selected treatment plan at the condition level. Instructions have been added to the HMR footer indicating this change beginning with the April run of the HMRs.
If you have any questions, please reach out to your HealthSpring Coding Educator for additional information and instruction. POET has reached out for this information.
HealthSpring Change in Prior Auths
Change in prior authorization administration for DME services, effective March 1, 2026 |
Effective March 1, 2026, HealthSpring will manage prior authorizations for durable medical equipment services, as well as orthotic and prosthetic codes. Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
EviCore healthcare will continue to manage prior authorizations for DME services through Feb. 28, 2026.
What this means to your patients through Feb. 28, 2026 · Submit prior authorization requests with dates of service before March 1, 2026, to EviCore as usual. · Continue to refer to EviCore for the most updated prior authorization code lists. · There are no changes to the claims submission or appeals processes.
|
Key changes effective March 1, 2026 · DME providers will submit prior authorization requests directly to HealthSpring. · Submit prior authorization requests to HealthSpring for dates of services beginning March 1, 2026. Request prior authorization through Availity Essentials™, our provider portal. · A list of procedural codes requiring prior authorization is available on the clinical review page of our provider website, HealthSpring.com/Providers. · Any authorization issued prior to March 1 will remain valid for those dates and services. That means, any authorizations approved by EviCore before March 1 will remain effective with HealthSpring. You do not need to submit a new prior authorization request.
|
How to request prior authorization Request prior authorization through our provider portal, Availity Essentials. This portal is the preferred and fastest method. Refer to Availity for instructions on setting up an account and navigating the portal. If you prefer, you can also call 1-800-914-8252 or fax 1-877-451-5541. |
Who Would’ve Thought?
Novitas Training on YouTube!
Novitas has made learning more convenient by offering helpful tutorials on YouTube. These short videos provide quick guidance on common Medicare topics, making it easier to find answers without having to attend a full webinar.
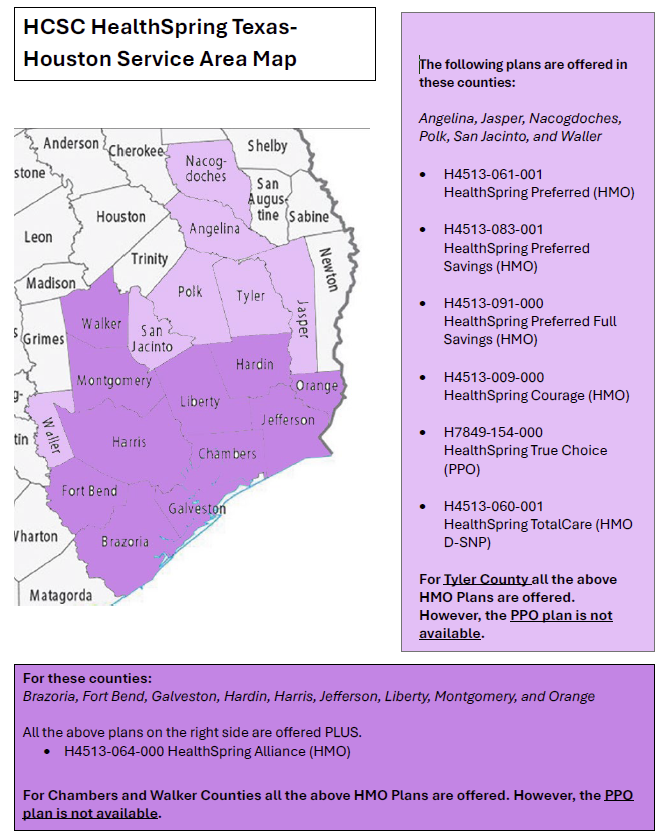
HealthSpring Plans by County
POET staff has done everything short of a full skeletal reconstruction to make the HealthSpring county page in the provider manual legible. They’ve stretched it. They’ve shrunk it. They’ve even converted it to Word and back to a PNG. It just didn’t have the backbone it needed.
If we were tibia honest, nothing worked.
So I, Sir Seymore Bones — resident WordPress writer and part-time osteo-optimizer — took pen in hand (metacarpals and all) to give everyone a little relief. When the formatting started rattling, I decided it was time to get to the bare bones of the issue.
I hope the map below helps you Sey-more, and make sense of the plans offered in our counties. We femur-ly believe this version is better. If it doesn’t… well, I promise I didn’t bone it up on purpose.
Stay humerus,
Sir Seymore Bones
Final 2026 Medicare Conversion Factors: What Providers Need to Know
Understanding the difference between QP and non-QP conversion factors
Each year, the Centers for Medicare & Medicaid Services (CMS) finalizes updates that impact Medicare reimbursement under the Physician Fee Schedule (PFS). One of the most important updates is the Medicare Conversion Factor (CF) — the dollar amount used to convert Relative Value Units (RVUs) into the final payment amount.
For Calendar Year (CY) 2026, CMS finalized two separate conversion factors:
One for Qualifying Participants (QPs) in Advanced Alternative Payment Models (Advanced APMs)
One for Non-Qualifying Participants (Non-QPs)
This distinction is important because it directly affects reimbursement rates depending on a provider’s participation status in the Quality Payment Program (QPP).
Qualifying Participants (QPs)
A provider becomes a QP by meeting specific thresholds for participation in Advanced APMs, such as having a certain percentage of payments or patients through eligible Advanced APM arrangements.
Key point: QPs receive a more favorable conversion factor update than non-QPs.
Non-Qualifying Participants (Non-QPs)
Providers who do not meet QP thresholds—or who participate in MIPS instead—fall into the non-QP category.
Bottom Line:
The Final 2026 Medicare Conversion Factors reinforce a major policy direction: CMS continues to differentiate payment updates based on participation in Advanced APMs.
Understanding whether your clinicians are QPs or non-QPs is essential for accurate reimbursement forecasting and strategic planning.
Conversion Factor:
- $33.57 for qualifying alternative payment model (APM) participants (QPs)
- $33.40 for non-QPs
- An increase of 3.77% for QPs and 3.26% for non-QPs over the 2025 rates
- Includes 0.75% increase for QPs and 0.25 for non-QPs
- 0.49% positive budget neutrality adjustment
- 2.50% increase from the OBBBA for 2026
HealthSpring Provider Manual 2026
Have you received your copy of the HealthSpring Provider Manual?
HealthSpring has a New Payor ID
PAYOR ID: 52192
Claims Address for paper claims: P.O. Box 23456 Chattanooga, TN. 37421
More on HealthSpring and CPL
Update: POET has been advised that the issue involving HealthSpring, CPL, and Polk County is related to a claims system error. HealthSpring has confirmed that they are currently in contract with CPL, and the issue is actively being worked on.
POET we keep you updated, as we receive information.
Recent Comments