Month: March 2022
Aetna 3rd-Party Claim and Code Review
Beginning June 1, 2022, you may see new claim edits.
According to March 1, 2022 Aetna OfficeLink Updates: These are part of our Third-Party Claim and Code Review Program. These edits support our continuing effort to process claims accurately for our commercial, Medicare and Student Health members. You can view these edits on our Availity provider portal.*
You can view any of these edits on Aetna’s Availity® provider portal.
For coding changes, go to:
- Aetna Payer Space
- Resources
- Expanded Claim Edits
Except for Student Health, you’ll also have access to Aetna’s code edit lookup tools. To find out if our new claim edits will apply to your claim, log in to our Availity provider portal. You’ll need to know your Aetna® provider ID number (PIN) to access our code edit lookup tools
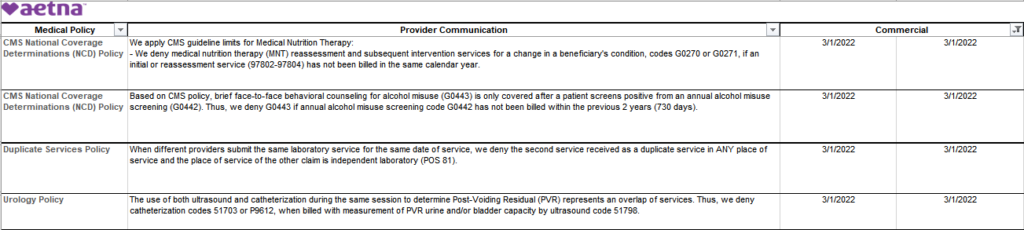
Here is what POET found with 2022 effective dates:
Reference Material for Your Staff that needs it.

Don’t cross your fingers or bring your rabbit foot.
Just download, print and keep a current copy of POET’s Provider Roster and Directory at your desk to make the Referral and Authorization process a bit easier.
File a Complaint
If a provider, believes a health plan isn’t complying with the dispute resolution process, then they may contact the No Surprises Help Desk at 1-800-985-3059 from 8 a.m. to 8 p.m. EST, 7 days a week, to submit a question or complaint. Or, they can submit a complaint online, below. Supporting documentation may be required. We’ll send a confirmation email to the provider when we receive their complaint to notify them of next steps and let them know if we need any additional information. To check on the status of a complaint, or to see what documentation is needed, contact the No Surprises Help Desk.
Recent Comments