Category: Business
BCBS June 1, 2023 HCPCS Update
POET has had a number of request regarding the BCBS Quarterly HCPCs Update.
You may use Ctrl + F to search or download the entire document.
How’d You Score?
Did you take Betsy Nicoletti’s Quiz on Modifier 25?
Let’s Explore the Facts or Rules Behind the Answers.
#1. The definition and rules for modifier 25 did not change in 2023. “In the March edition of the CPT Assistant it says that while the rules weren’t changed in the 2023 code set “confusion exists regarding its appropriate use.”
#2. What does a modifier added to a CPT or HCPCS code do? The answer is b) Indicates the service or procedure was altered by specific circumstances.
Some modifiers affect payment (like modifier 25) and some are informational only (those appended to teaching physician services). CPT modifiers may be used on HCPCS codes and HCPCS modifiers on CPT codes. A modifier doesn’t change the definition of the code, but indicates that the service or procedure was altered in some way.
#3. When using modifier 25 when reporting an E/M services and a minor procedure, do you need a different diagnosis for the E/M and the Procedure? The answer is NO.
“As such, different diagnoses are not required for reporting of the E/M services on the same date”. CMS says, “If a significant separately identifiable evaluation and management service is performed, the appropriate E&M code should be reported utilizing modifier 25 in addition to the chemotherapy administration or nonchemotherapy injection and infusion service. For an evaluation and Management service provided on the same day, a different diagnosis is not required.” Medicare Claims Processing Manual, CH. 12 30.5.C
#4. When performing a minor procedure, usual preoperative and postoperative activities are included i in the work of the procedure and should not be reported with an E/M service. Which of these activities are considered usual preoperative and postoperative activities? (List may not be complete). Answer is d) All of the above.
The March 2023 CPT Assistant lists the services that are considered part of the procedure—paid for within the fee for the procedure—and should not be counted as a separate E/M.
Pre- and post-operative services typically associated with a procedure include the following and cannot be reported with a separate E/M services code:
• Review of patient’s relevant past medical history,
• Assessment of the problem area to be treated by surgical or other service,
• Formulation and explanation of the clinical diagnosis,
• Review and explanation of the procedure to the patient, family, or caregiver,
• Discussion of alternative treatments or diagnostic options,
• Obtaining informed consent,
• Providing postoperative care instructions,
• Discussion of any further treatment and follow up after the procedure
5) When performing a preventive medicine service or wellness visit, the practitioner also assesses and manages the patient’s chronic conditions, reviews labs, and renews multiple prescriptions. How is this billed? The Answer is b) Preventive medicine or wellness visit and a problem-oriented visit, with modifier 25 on the problem-oriented visit
Medicare Claims Processing Manual, Ch 12. 30.6.1.1.2.H
“When the physician or qualified NPP, or for AWV the health professional, provides a significant, separately identifiable medically necessary E/M service in addition to the IPPE or an AWV, CPT codes 99201 – 99215 may be reported depending on the clinical appropriateness of the circumstances. CPT Modifier -25 shall be appended to the medically necessary E/M service identifying this service as a significant, separately identifiable service from the IPPE or AWV code reported (HCPCS code G0344 or G0402, whichever applies based on the date the IPPE is performed, or HCPCS code G0438 or G0439 whichever AWV code applies).”CPT Professional Ed., 2023, page 32

Cheers to knowledge
Check Your Modifier 25 Knowledge

Our Friend Betsy Nicoletti founder of CodingIntel, says “It’s hard for me to think of a topic that invites so much disagreement between coders and auditors, between practices and payers and with our practitioners.”
She has put together a short little quiz on the topic (below). Tell us how you did.
DEA Registration Requires Training
Physicians who must register or renew their registration for a Drug Enforcement Administration license will face a new requirement as of June 27:
To register, they will have to attest to taking a one-time, eight-hour training on how to treat patients with opioid or other substance use disorders.
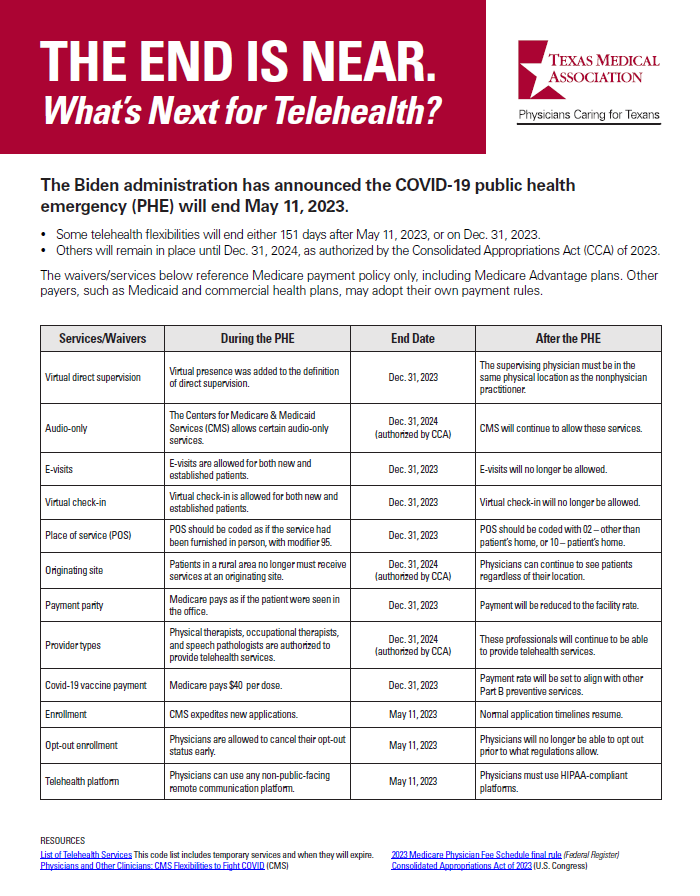
THE END IS NEAR

What’s Next for Telehealth?
UHC April Monthly Overview

For Texas:
Starting June 1, 2023, Optum will manage prior authorization and step therapy requests for prescription medications for Texas residents with pharmacy coverage.
Medicare vs Inflation
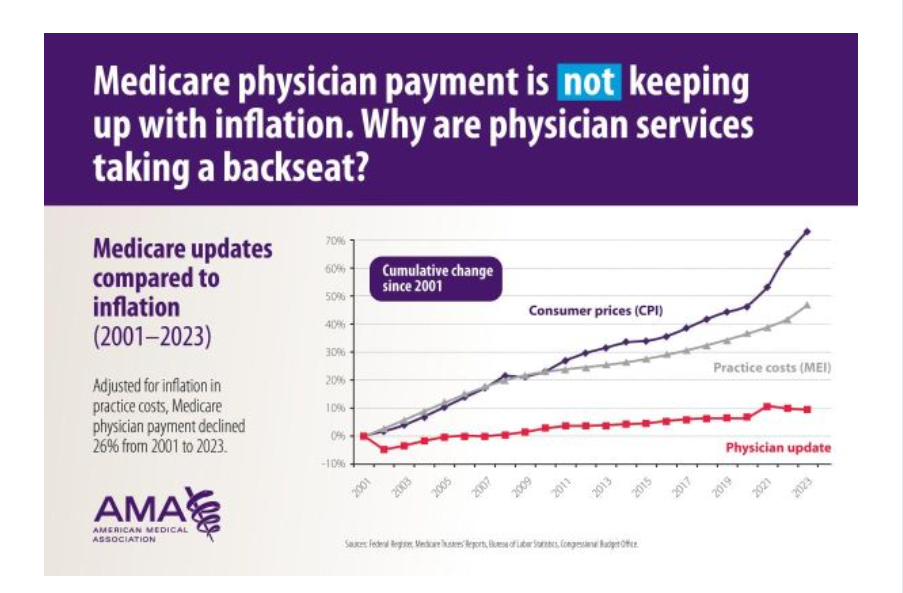
As part of a broader push for Medicare payment reform, the Texas Medical Association, along with the American Medical Association and 133 national specialty and state medical associations, recently called on Congress to index Medicare physician payments to inflation.
More on UHC Electronic Submissions

Get to know the basics of electronic submissions
Now that claim reconsiderations and appeals must be submitted electronically,* we want to help make sure you have the how-to information you need to manage them with ease.
How to submit electronically
You have 2 electronic submission options — through the UnitedHealthcare Provider Portal or Application Programming Interface (API). See the Online Reconsiderations and Appeals interactive guide for step-by-step instructions on how to submit reconsiderations and appeals electronically.
TIPS:
- Check the TrackIt Action Required bar regularly to see the status of claims, reconsideration requests and more
- To take action on a specific claim in the portal, go to Claims & Payments and search for a claim. Once you’ve searched for a claim and selected Act on a Claim, a list of actions will appear (e.g., View Claim Reconsideration, File Appeal/Dispute). Based upon the current status of the claim or previously taken actions, the buttons will either be blue or grayed out. If grayed out, that specific action is unavailable.
- Please note: Available actions may vary based on the member’s plan type, provider’s participation status and regulations
- If a claim(s) from your claim search results shows an “Acknowledgement” status, it hasn’t been processed. You’ll be unable to submit requests related to this claim.
- Reminder: Appeal response letters are no longer mailed, but you can view and print them through the portal using Document Library
ASK THE EXPERT
TMA RESOURCES |
Ask the Expert: End of the Public Health EmergencyOn March 29 via Zoom, join TMA experts in this interactive Q&A session as they discuss how best to prepare your practice for upcoming changes as the public health emergency winds down on May 11. They will discuss the impact on Medicaid coverage, telehealth, and COVID vaccines and treatments for which you can earn CME. Send your questions in advance. Register now. |
Health Plan – Representative Update

Please print this updated list. Keep it handy for working claim issues. Many have changed.

Recent Comments