2024 Payer Scorecard: How payers are failing practices and patients
Physicians Practice: November 11, 2024, By Keith A Reynolds

How would you characterize your prior authorization experience in the last year?
We’re doing more prior authorizations
74%
We’re doing fewer prior authorizations
4%
Prior authorizations are about the same
22%

Do you think there should be a CPT code requiring payers to reimburse for prior authorization work?
Yes
97%
No
3%



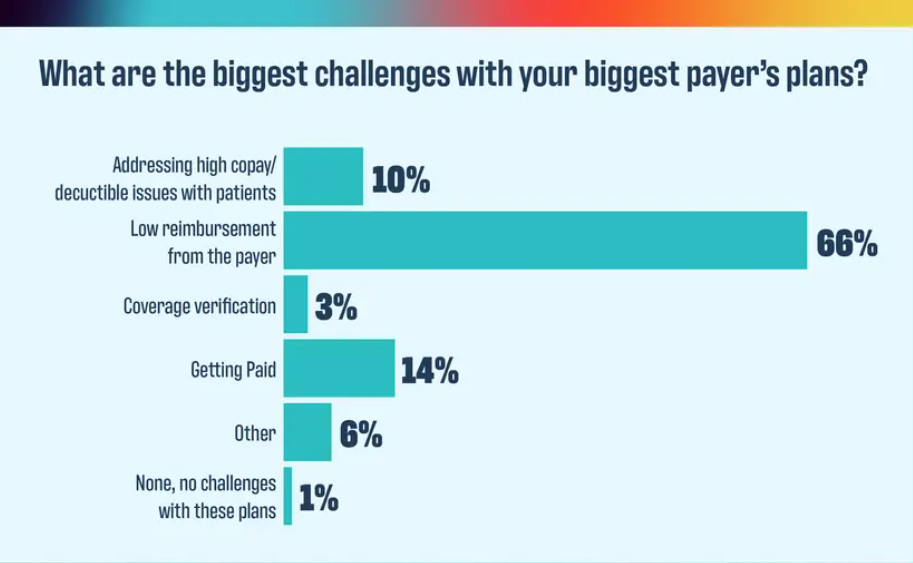
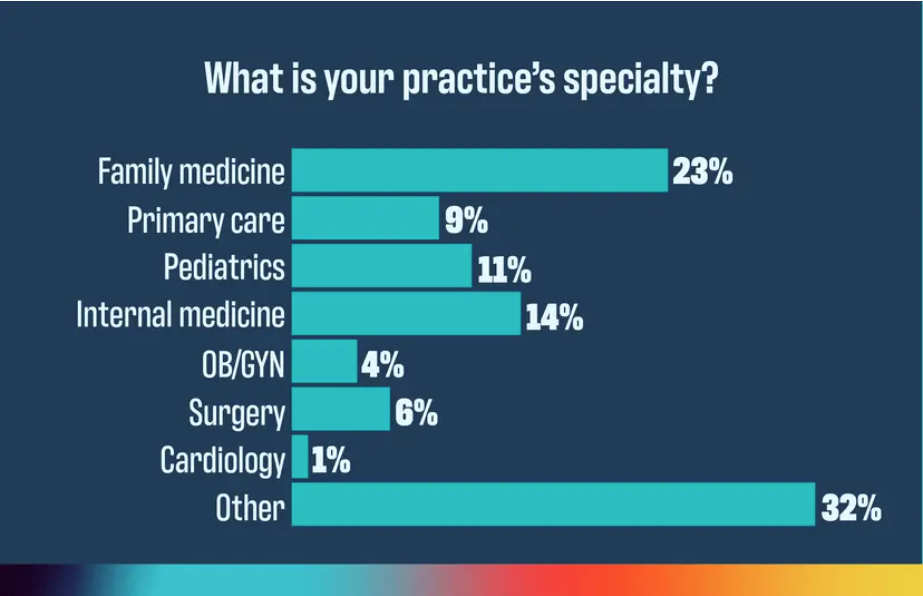
What is your biggest challenge with your biggest payer?
- Current systems don’t interact well with our billing systems requiring office staff to correct claims leading to delayed payment
- Reimbursement stinks. I Quit !!!!!!
- Staff the insurance companies contracted are mostly out of the country and do not know the issues we have and do not like to refer the questions or specific issues to any expert in the field.
- Small practice is ignored. They would not negotiate fees. For more than 15 years no increase in fees, only steady decrease. It is a shame, no respect any longer for providers.
- Prior authorizations waste so much time for what should be a simple process
- Lack of urgency or even motivation to provide basic service
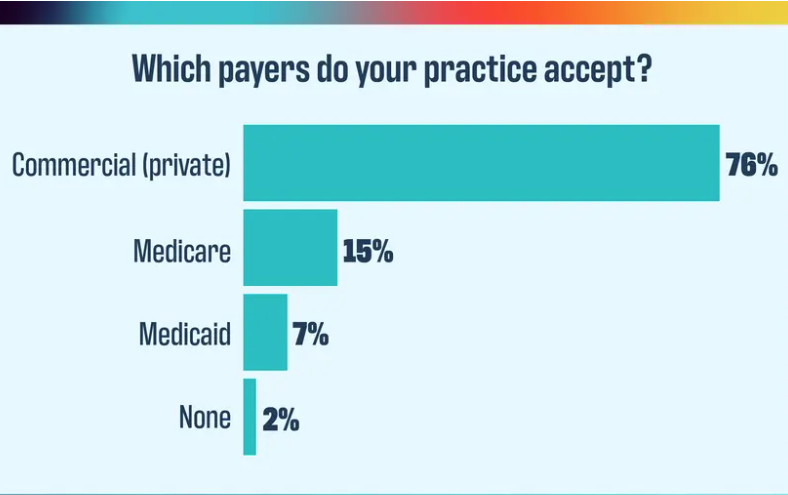
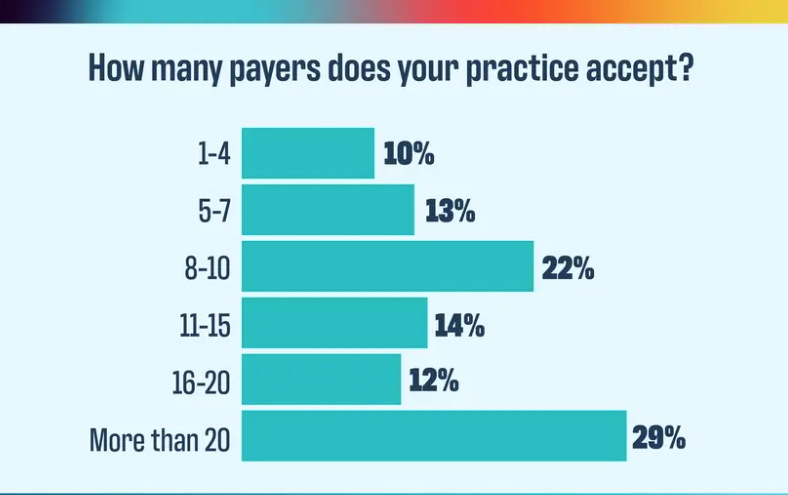
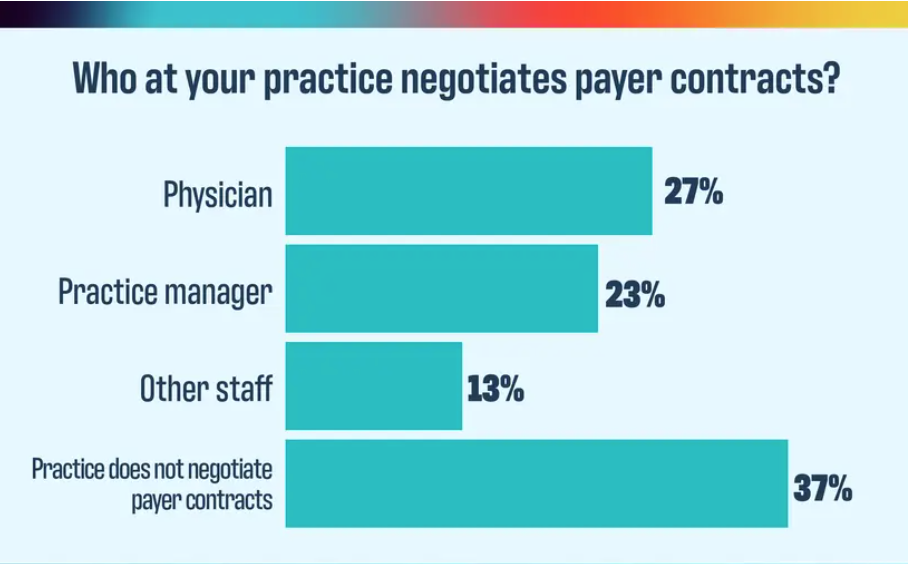
The verdict is in for how practices feel about their payers, and it isn’t good.
How can payers improve their relationship with practices?
- Streamline systems to allow for clean claims the first time
- Have a dedicated Provider Relations contact so we know who to talk to, and who to call to get responses to critical questions, not have to send emails to faceless representatives that have a low rate of resolution.
- Communicate. Show WHY they deny, and what EXACTLY can be done to help the patients who pay them. Do not simply deny with NO guidance.
- Pay us enough to survive. Instead, they raise hospital payments. Paying us more so we could hire more doctors and physicians assistants and keep people OUT of those hospitals.
- Stop putting technology problems and carrier losses on the provider and their patients.
- Instead of looking at me as an expense, look at me as a tool to care for their beneficiaries.
- Stop requiring PAs for generic meds and obviously necessary medications.
Medicare Solidifies Pay Cut
In a final rule that solidifies a nearly 3% Medicare pay cut for physicians in 2025, the Centers for Medicare & Medicaid Services (CMS) also set the trajectory for physician practices over the next year with a mixed bag of changes related to telemedicine, coding and payment, and the Merit-Based Incentive Payment System (MIPS), among others. ~By Phil West
While TMA analyzes what it sees as some isolated, positive changes resulting from CMS’ finalization of the 2025 Medicare Physician Fee Schedule, it is also urging physicians to act now to show their support for House Resolution 10073
LAST CHANCE
Compliance Training
There is still room at the table for POET’s last compliance webinar, November 5th, Noon.
Two topics will be represented: “OSHA for Medical Practices” and “Establishing and Maintaining a Healthcare Compliance Program”.
Come network with other Physician office managers and staff.
Get a bite to eat (you will need to submit your order for Chick-fil-a).
And concur some of that compliance training you have on your to-do list.
Call POET (936) 637-7638
Is Your Plate Full?
Saving Time Playbook
This playbook will provide strategies to organizational leaders to enhance processes, implement time-saving workflows, increase the efficiency of their practice, and improve physician well-being
POINTS OF INTEREST:
- The Burnout Problem Is Organizational, Not Personal
- Stop the Unnecessary Work
- Getting Rid of Stupid Stuff
- Share the Necessary Work
- Advanced Rooming and Discharge
- Tasks Medical Assistants or Other Team Member Can Complete
- Make the Case to Leadership
- And Much, Much More: Graphs, podcast, practical tools, checklist, and toolkits
NOW YOU KNOW

Every business, especially a medical practice, needs to run like a well-oiled machine
Just as oil prevents an engine from drying out and freezing up, your medical practice must have a well-developed denial management program in place. This is the first proactive step.
Security Training Tips for Frontline Employees
The shift towards digital solutions has had a profound impact and benefit. However, it has also introduced new challenges, particularly concerning security, which is why your frontline employees need to be properly trained to ensure your business and customers are protected.
As frontline sectors continue to embrace technology, the dependency on digital tools and platforms grows. Employees now rely on various devices and software to perform their duties, from processing transactions and managing customer interactions to accessing sensitive information. Point-of-sale systems, digital customer service platforms, electronic health records, and mobile apps are now standard tools in these environments.
The Importance of Security Training for Frontline Workers
Frontline workers extend beyond emergency responders. It’s an encompassing term to describe individuals who are the first point-of-contact between a company and its customers. They can handle sensitive information, greet patrons as they enter facilities, or provide direct support when needed
Why is front line training so vital?
- Direct Customer Interaction
- Protecting Sensitive Information
- Identifying Threats
- Compliance with Regulations
- Building Customer Trust
For Additional Helps and Tips Visit: Vector Security’s Security Blog.
CMS Increased Payment for Influenza Vaccines
On August 1, the Centers of Medicare and Medicaid Services (CMS) increased payments to physicians for influenza vaccines and updated which codes physicians should use when billing for the service during the 2024-25 flu season.
Texas Medical Association billing and coding staff caution that to receive payment, physicians also will need to use a national drug code (NDC) associated with the current period.
Follow this link for proper CPT codes and more vaccine information.
Revisions to Medicare Part B Coverage of Pneumococcal Vaccinations Policy
Co-pays Resuming for Certain Services

Effective 10/1/24: Co-pays will Resume for CHIP CoVid19 Services.
During the COVID-19 public health emergency, the Texas Health and Human Services Commission (HHSC) waived co-pays for COVID-19 vaccines, testing, and treatment for Children’s Health Insurance Program (CHIP) members. This waiver will end on September 30, 2024
Providers may begin collecting co-pays for COVID-19 vaccines, testing, and treatment rendered to CHIP eligible members for dates of service on or after October 1, 2024.
Providers may not charge co-pays for mental health and substance use disorder outpatient office visits
Co-pays have been permanently removed for mental health and substance use disorder outpatient office visits to comply with federal regulations.
Information for Medicaid Providers
Upcoming Changes to STAR+PLUS
Effective September 1, HHSC is transitioning contracts for the STAR+PLUS program. Below are a few resources that may help.
If you need help with….
Try…
Managed Organization Complaints.
Knowing how this transition will impact my billing.
Please reach out to the MCO to understand their billing process.
Helping your clients through the transition.
See the HHSC Star+Plus webpage for transition resources.
For any STAR+PLUS transition related issues, please contact the STAR+PLUS Go Live Inbox.
And as always, contact POET if you have any concerns.
BCBSTX to Require E/M Codes for Consultation Services
Starting Nov. 18, Blue Cross and Blue Shield of Texas (BCBSTX) will no longer pay physicians for outpatient or inpatient consultations when they report those services with Current Procedural Terminology (CPT) codes 99242 – 99245 and 99252 – 99255.
Instead, the payer says physicians will need to report consultation services with an appropriate office outpatient or inpatient evaluation and management (E/M) code representing where the visit occurred and its level of complexity.
According to the health plan, consultation claims reported with CPT codes after Nov. 18 will be denied.
Updated 12/10/2024, to add BCBS website information
Evaluation and Management Coding – Professional Provider Services
Policy Number: CPCP024
Version 1.0
Enterprise Clinical Payment and Coding Policy Committee Approval Date:
August 7, 2024
Plan Effective Date: November 18, 2024
(Blue Cross and Blue Shield of Texas Only
Consultation(s) CPT Codes 99242-99245 ,99252-99255 Effective 11/18/2024, the plan will no longer reimburse for office/outpatient consultation codes (CPT codes 99242–99245) and inpatient consultation codes (CPT codes 99252–99255). Consultation services should be reported with an appropriate office/outpatient or inpatient E/M code representing the location where the visit occurred and the level of complexity of the visit performed, such as code ranges 99221-99223, 99304-99306, and 99202-99215.
Recent Comments