UHC December Monthly Overview
Key changes for our Medicare Advantage plan
- In 2026, most UnitedHealthcare Medicare Advantage health maintenance organization (HMO) and point of service (POS) plans are referral plans. You can check plan referral requirements online.
- Starting Jan. 1, 2026, most members enrolled in UnitedHealthcare Medicare Advantage HMO/POS plans will be required to obtain a referral from their primary care provider (PCP) before accessing certain specialist services in outpatient, office or home settings. Referrals must be submitted by the PCP to UnitedHealthcare prior to the specialist visit. This also applies when members of HMO/POS plans are traveling and accessing the National Network. Learn more in our 2026 Medicare Advantage Referral Requirements Guideopen_in_new.
- Effective Jan. 1, 2026, new or existing members of UnitedHealthcare SNPs, including Chronic Special Needs Plans (C-SNP) and Dual Special Needs Plans (D-SNP), need a qualifying chronic condition to access benefits that cover healthy food and/or utilities. Providers may be contacted by UnitedHealthcare to verify a member has at least one qualifying condition to receive benefits. See 2026 Medicare Advantage, CSNP & DSNP Plan Overview Courseopen_in_new for more information.
BCBS Pharmacy Qtrly Updates for January 2026
Pharmacy Program Quarterly Update Changes Effective Jan. 1, 2026 – Part 1
Scheduling Webinar
“Every patient experience begins with the people who deliver care — and scheduling is what brings providers, nurses, and staff together at the right time. More than a staffing tool, scheduling is the backbone of modern healthcare.
In an era of workforce shortages, rising burnout, and increasing regulatory scrutiny, healthcare leaders are being called to go all in on strategies that unify scheduling, build workforce resilience, and seamlessly connect every member of the care team around the patient’s needs.
In this session, you’ll hear from a panel of healthcare innovators who have tackled the challenges of scheduling across providers, nurses, staff, and physical resources. They’ll share proven approaches you can apply to balance flexibility, fairness, and resilience while strengthening compliance confidence and improving visibility across your organization. You’ll leave with practical insights into how a holistic approach to scheduling can boost workforce engagement, improve access to care, and deliver stronger financial and patient outcomes.
Learning Objectives:
- Recognize the schedule as a strategic asset for care team coordination, compliance, and patient access.
- Learn how clinical and operations leaders can collaborate to unify scheduling, communication, and credentialing strategies.
- Explore practical approaches to strengthening compliance confidence (e.g., EMTALA, ACS standards, audit requirements) through improved workforce coordination.
- Recognize the enterprise value of going “all in” on workforce scheduling strategies to reduce risk, optimize resources, and improve patient and financial outcomes.”
The Definition of G0136 is Changing
Another Great Article from CodingIntel
November 2025
|
BCBS CIR Cheat Sheet
“The Claim Inquiry Resolution (CIR) tool within the Electronic Refund Management (eRM) portal accessed via Availity® Essentials only accepts inquiry submissions related to High-Dollar, Pre-Pay Review requests for most Host (BlueCard® out-of-area) claims (Medical Records and/or Itemized Bills). The other inquiry options that were available via CIR have transitioned to the Availity Claim Status Tool’s Dispute Claim or Message This Payer features.” Per BCBS Provider Education.
WHAT CAN BE DOWNLOADED TO eRM?

See Example Below —

UHC November Update
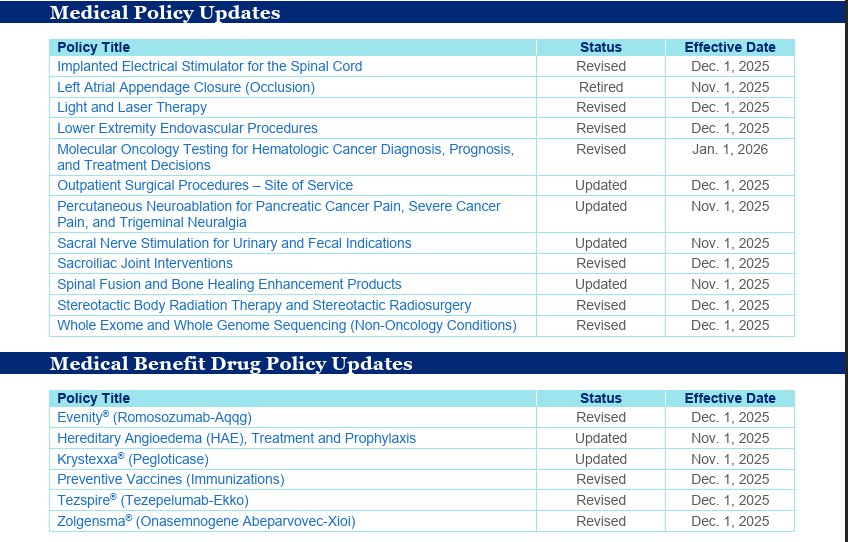
A list of recently approved, revised, and/or retired Medical Policies and/or Medical Benefit Drug Policies is provided below for your reference. For a comprehensive summary of the latest updates, refer to the Medical Policy Update Bulletin: November 2025.
Medicare Beneficiaries Involved in CMS Data Breach
CMS Notifies Individuals Potentially Impacted by Data Incident
Approximately 103,000 beneficiaries may have been impacted.
POET has been told by several offices, they are seeing beneficiaries who have been assigned a new number by CMS.
CMS Instructs MACs to Lift Claims Hold

Special edition – courtesy of Novitas Solutions
Claims Hold Update
CMS instructed all Medicare Administrative Contractors (MACs) to lift the claims hold and process claims with dates of service of October 1, 2025, and later for certain services impacted by select expired Medicare legislative payment provisions passed under the Full-Year Continuing Appropriations and Extensions Act, 2025 (Pub. L. 119-4, Mar. 15, 2025). This includes claims paid under the Medicare Physician Fee Schedule, ground ambulance transport claims, and Federally Qualified Health Center (FQHC) claims. This includes telehealth claims that CMS can confirm are definitively for behavioral and mental health services. CMS has directed all MACs to continue to temporarily hold claims for other telehealth services (i.e. those that CMS cannot confirm are definitively for behavioral and mental health services) and for acute Hospital Care at Home claims.
Beginning October 1, 2025, for services that are not behavioral health services, many of the statutory limitations on payment for Medicare telehealth services that were, in response to the COVID-19 Public Health Emergency, lifted, and subsequently extended, through legislation again took effect. These include prohibition of many services provided to beneficiaries in their homes and outside of rural areas, and hospice recertifications that require a face-to-face encounter. In the absence of Congressional action, practitioners who choose to perform telehealth services that are not payable by Medicare on or after October 1, 2025, may want to evaluate providing beneficiaries with an Advance Beneficiary Notice of Noncoverage (ABN). Further information on use of the ABN, including ABN forms and form instructions: https://www.cms.gov/medicare/forms-notices/beneficiary-notices-initiative/ffs-abn. Practitioners should monitor Congressional action and may choose to hold claims associated with telehealth services that are currently not payable by Medicare in the absence of Congressional action. For further information: https://www.cms.gov/medicare/coverage/telehealth.
CMS notes that the Bipartisan Budget Act of 2018 (Pub. L. 115-123, Feb. 9, 2018), which added section 1899(l) to the Social Security Act, allows clinicians in applicable Medicare Shared Savings Program Accountable Care Organizations (ACOs) to provide and receive payment for covered telehealth services to certain Medicare beneficiaries without geographic restrictions and in the beneficiary’s home. Separate from requirements to participate in the Medicare Shared Savings Program, there is no special application or approval process for applicable ACOs or their ACO participants or ACO providers/suppliers to offer these covered telehealth services. Clinicians in applicable ACOs can furnish and receive payment for covered telehealth services under these special telehealth flexibilities. For clinicians in applicable ACOs, telehealth claims that CMS can confirm are definitively for behavioral and mental health services will be paid. At this time, claims for some telehealth services will continue to be held. For more information, including information on to which ACOs these flexibilities apply: https://www.cms.gov/files/document/shared-savings-program-telehealth-fact-sheet.pdf.
More Telehealth Waivers Set to Expire Dec. 31
As TMA monitors the government shutdown and the coinciding expiration of certain telehealth waivers as of Sept. 30, physicians should take notice of another series of telehealth waivers set to expire at the end of this year.
TMA staff note that Medicare Advantage plans don’t have to follow Medicare’s policy on the waiver expirations.
The following waivers enacted during the COVID-19 public health emergency (PHE) are currently expected to expire Dec. 31 unless Congress acts:
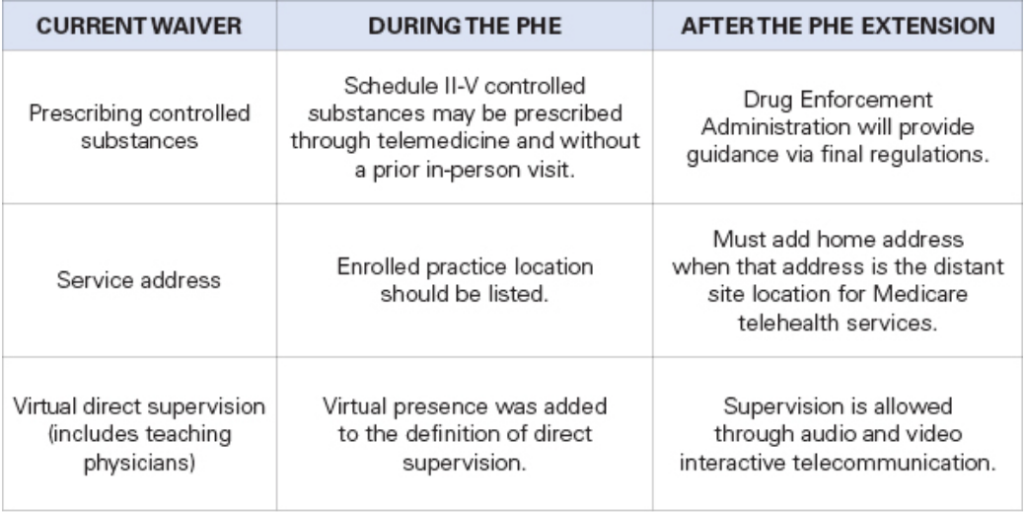
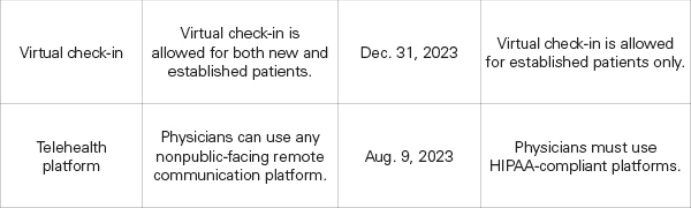
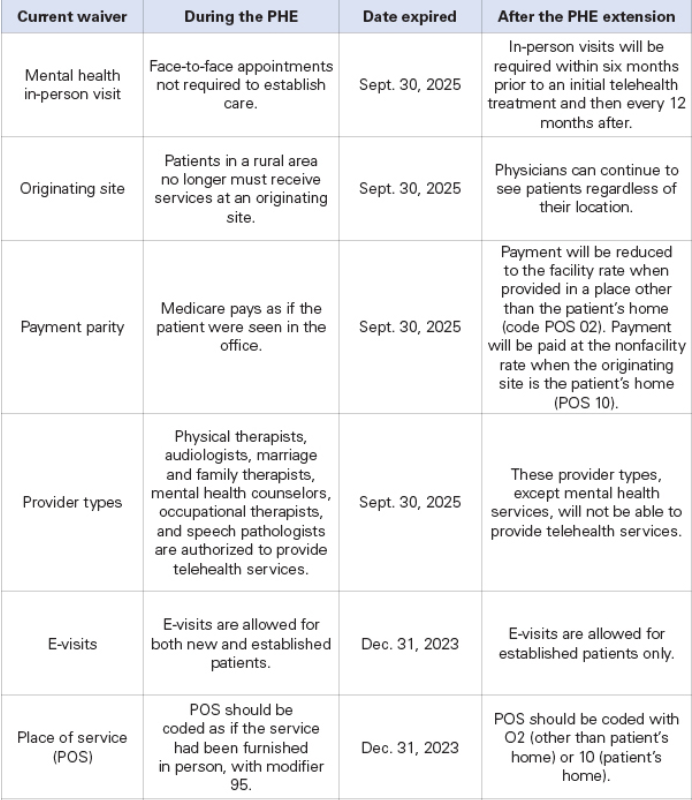
The following waivers have already expired:

TMA Coming to Tyler
Local Medicine Matters Conference Tyler, Texas
October 24-25, 2025

The Local Medicine Matters Conference is a new regional event, part of the Texas Medical Association’s initiative to hold events beyond the Texas metro areas. This inaugural conference is being hosted by the Smith County Medical Society in conjunction with TMA. The one-day event features topics of broad interest across all physician members, including practical uses of augmented intelligence in medicine, updates to billing and coding, and how physicians fared following the 2025 Texas legislative session.
Friday Night Mixer Oct. 24th
5:00 PM – 7:PM
Guest and Members Free
Saturday Conference Oct. 25th
7:30 AM – 4:00 PM
TMA Members Free
Registration
Registration for TMA members, CMS and association staff, and Alliance members is FREE – one of the many benefits of annual membership!
A $25 registration fee will be charged for on-site registrants.
Registration Fees:
Nonmember physicians: $200
Guests of members and medical staff: $150
Conference Agenda
Friday, Oct. 24 | The Grove Kitchen and Gardens
5 pm – 7 pm | Regional Membership Happy Hour
Saturday, Oct. 25 | Brookshire Conference Center
7:30 am – 1:00 pm | Registration Open
8:00 am – 8:30 am | Walk-with-A-Doc in the Tyler Rose Garden
8:15 am – 9:00 am | Breakfast
9:00 am – 9:15 am | Opening Remarks
Jayesh Shah, MD, President, Texas Medical Association
9:15 am – 10:15 am | Augmented Intelligence: Policies, Procedures, and Preparation
Explore how augmented intelligence (AI) is being practically applied in medicine to enhance efficiency and ease for healthcare professionals.
Shannon Vogel, AVP, Health Information Technology, Texas Medical Association
10:25 am – 11:25 am | P.R.O.A.C.T.I.V.E
In billing, your best practice is to be proactive. When you are reactive, payment delays, denials, and loss of revenue are more likely to occur. This presentation will review key points and best practices for being proactive to assist with efficiency and minimize unnecessary delays.
Carra Benson, Director, Physician Payment Services, Texas Medical Association
11:30 am – 12:30 pm | Lunch
12:30 pm – 1:30 pm | 2025 Legislative Wins: Texas Edition
Jayesh “Jay” Shah, MD, President, Texas Medical Association
Matt Dowling, Director of Public Affairs, Lobbyist, Texas Medical Association
1:40 pm – 2:40 pm | Lawsuits and TMB Investigations: How to Avoid Them (Ethics CME)
Lajuana Acklin, JD, Senior Associate, Bertolino Law Firm
2:50 pm -5:00 pm | Media Training
Brent Annear, Associate Vice President, Media Relations and Leadership Advancement, Texas Medical Association


Recent Comments