HEADS UP! Rider 32 Transition
Effective September 1, 2025
Texas Health and Human Services Commission will implement Rider 32, which will transition Medicaid only services for dually eligible members from a fee-for-service model to a managed care delivery system.
This change affects services provided to members who are eligible for both Medicaid and Medicare. It applies only to those Medicaid services not covered by Medicare.
Providers will bill the MCO for Medicaid wrap-around services provided to dually eligible members.
Wrap-around services include all Medicaid services not covered by Medicare. They are limited to those already covered under managed care for Medicaid-only members.
UHC Claims their new API makes work easier.
UnitedHealthCare’s Application Program Interface (API) is a free digital solution that automates everyday work.
Benefits of using API
- Reduces phone calls and paper
- Automates transactions on your timetable
- Distributes data faster to where you need it
- Get real‑time information
- Supports standard formats and compatible with new technology
- Maximizes efficiency and productivity through workflow integration
Why add API to your practice?
- Flexibility: Allows you to choose the data and API that fit your needs.
- Automation: Incorporates seamlessly into your workflow.
- Security: Ensures data is accessed and transferred securely
Humana
TIPS, TRICKS AND HELPS
PREAUTHORIZATON LISTS (PAL):
Lists of services and medications effective July 1, 2025, that may required preauthorization for members with Medicaid, Medicare Advantage, and dual Medicare-Medicaid coverage are now available.
Easily determine if a prior authorization is required with Humana’s search tool. Search by Current Procedural Terminology (CPT®) codes, procedures or generic drug name(s). Remember to verify benefit coverage in Availity Essentials
Availity Essentials Introduces Check Claim Status Feature:
Availity has enhanced its Eligibility and Benefits (E/B) page by adding a Check Claim Status feature.
What you can expect:
- Improved efficiency and accuracy: The check Claim Status tool pre-populates your patient’s information, ensuring accuracy.
- Time savings: You can access claim status with one click- saving time and effort
Separate Services, Same Date of Service
With health plans increasingly adopting payment protocols that hinder physicians from providing multiple services on the same day – despite previously covering such services – delegates adopted policy calling on TMA to “advocate for legislation or regulation that would prevent Medicaid and commercial payers from denying payment for distinct, separate services provided on the same day.”
Delegates agreed with physicians’ concerns that these payer practices often force patients to forego care.
“This especially hurts patients who either have to travel long distances to see their physician or have transportation issues that prevent them from making multiple trips,” Odessa allergist and immunologist Vivek Rao, MD, wrote in online testimony on behalf of the Lone Star Caucus
Other measures adopted by the house to eliminate payment-related barriers to patient care direct TMA to pursue state-level legislation or regulation that:
- Prohibits insurers, plan sponsors, third party administrators, and other contracted identities from recouping previously paid claims due to retroactive termination of patient coverage;
- Imposes payer communication standards – with penalties – that provide patients, physicians, and others with timely access to a live representative; and
- Expedites prior authorization approvals for hospice care in emergency and acute care settings, eliminates deductibles for hospice care, and provides clear disclosures detailing hospice care benefits in policy documents as well as online.
Mandated CME Requirements Are Shifting
A recent reorganization of Texas Medical Board (TMB) rules has removed certain universal CME obligations. The removal of universal CME requirements could result in a lighter load for physicians but may make it more challenging to determine what is required and when.
Please click the button below to view the entire article from Texas Medical Assocation.
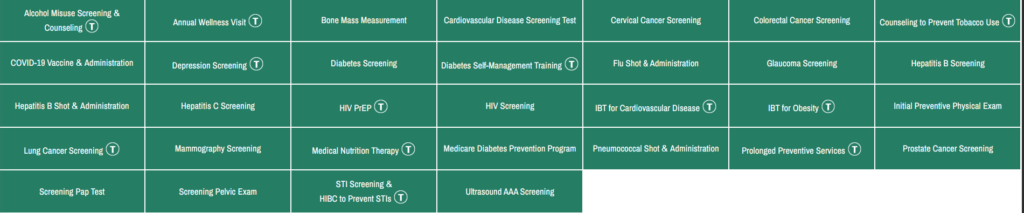
Medicare Preventive Services – Revised
The above link will lead you to MLN Educational Tool, where you can click a service and see the changes.
Bringing Joy to Your Staff
Medical practices run on people, not just physicians.
Support staff—front‑desk schedulers, billers, MAs, nurses—often shoulder the first wave of patient frustration and the last wave of administrative overload. When joy disappears, turnover follows and patient experience slips.
Here are 10 evidence‑based tactics (offered by “Physician Practice”) to put delight back into the workday and keep your best people.
1. Ask, listen and act on feedback
Move from “suggestion box” to true participative management. Before rolling out any workflow change, solicit frontline ideas in daily huddles, publish the top three suggestions on a whiteboard and close the loop within a week. Employees who see their input reflected in policy score higher on engagement surveys and are more likely to propose innovations that save time and money
2. Recognize great work in real time
Dollar‑free praise beats stale year‑end bonuses. Public shout‑outs at a morning huddle or via an oversized card signed by peers reinforce behaviors that improve patient flow and safety. Tie each kudo to a specific accomplishment so staff connect the dots between effort and outcome
3. Celebrate small wins and birthdays
Micro‑celebrations trump a lone holiday party. The classic “Cinco de Mayo taco bar” or an impromptu cupcake run after a spotless audit tells staff you notice the grind. Those light moments strengthen social bonds that translate into better teamwork when the waiting room is overflowing.
4. Offer genuine scheduling flexibility
Extra PTO, rotating early‑out Fridays or seasonal compressed shifts cost less than recruiting a replacement. Flexible scheduling keeps mid‑career parents in the workforce and can even delay retirements, preserving institutional knowledge while lifting morale.
5. Make the break room a refuge
Healthy snacks, natural light and a phone‑free policy turn 15 minutes of downtime into true recovery. Keeping the refrigerator stocked with fruit and yogurt is a low‑budget perk that employees consistently list among their favorite morale boosters.
6. Invest in professional growth
Stagnation is the enemy of joy. Map a modest CME budget to every role, fund at least one conference or certification per employee each year, and spotlight success stories at staff meetings. Practices that budget for training report higher morale and fewer costly coding errors.
7. Delegate with purpose, not desperation
Match assignments to strengths and clarify roles so no one feels set up to fail. Clear expectations create “psychological safety,” a proven driver of high‑performing medical teams and a buffer against burnout.
8. Lead with transparency and empathy
Trust grows when leadership shares key metrics, explains tough decisions and asks, “How can we help?” Thoughtful, two‑way communication is one of the quickest ways to boost engagement and cut gossip that erodes culture.
9. Give employees a voice in quality‑improvement projects
Invite schedulers, billers and medical assistants to co‑design process fixes—whether a new triage script or a quicker prior‑auth checklist. Staff who help craft solutions adopt them faster and police the workflow themselves, freeing managers to lead rather than chase compliance.
10. Inject fun into routine days
Ugly‑sweater contests, step‑count challenges or “puppy‑visit Fridays” (partner with a local shelter) deliver quick dopamine hits that last long after the prize. Practices that weave lighthearted events into the calendar report lower absenteeism and higher patient‑experience scores.
Check Your BCBS Flu Test Claims
BCBSTX explained in correspondence with TMA’s Physician Payment Resource Center (PPRC) – which reached out for clarification earlier this month on the payer’s new flu testing policy – that some claims for certain labs, including those offering flu testing, were unintentionally denied due to a vendor error.
TMA’s Director of Physician Payment Services Carra Benson says physicians do not need to take action to receive payment. However, she recommends physicians review flu testing claims filed between Jan. 1 and Feb. 13 to ensure correct reprocessing.
Aetna OfficeLink Updates May 2025
May 2025
This month’s reminders:
We regularly review and adjust our clinical, payment and coding policies. Review our policies and claim edits on our provider portal on Availity®.* Just go to Payer Space > Resources > Expanded Claim Edits. Or you may visit Aetna.com to see them.
Coding/billing update: To align with CMS, starting August 1, 2025 we’ll no longer cover 88305 (Level IV surgical pathology, gross and microscopic examination) when billed with 55700 and/or 55706 (prostate incision procedures) on the same date of service. We’ll also allow G0416 (surgical pathology, gross and microscopic examinations) once per date of service.
Note to Texas providers: Changes described in this article will be implemented for fully insured plans written in the state of Texas only if such changes are in accordance with applicable regulatory requirements. Changes for all other plans will be as outlined in this article

Recent Comments