Tag: Aetna
Aetna OfficeLink Updates, Oct. 1, 2023
Healthcare Common Procedure Coding System (HCPCS) modifiers FX and FY
Effective January 1, 2024, we will reduce payment for radiology procedures billed with modifiers FX and FY to align with the Centers for Medicare & Medicaid Services (CMS) guidelines.
• Modifier FX (X-ray taken using film): A 20% payment reduction applies to the technical component (and the technical component of the global fee).
• Modifier FY (computed radiography X-ray): A 10% payment reduction applies to the technical component (and the technical component of the global fee).
Reimbursement for code A9279
(monitoring feature/device)
Effective January 1, 2024, Aetna® will no longer reimburse for code A9279, since it is considered statutorily non-covered.
Aetna Claim and Code Review Program
This update applies to Aetna’s Commercial, Medicare and Student Health members.
Beginning September 1, 2023, you may see new claim edits. These are part of our CCRP. These edits support our continuing effort to process claims accurately for our commercial, Medicare and Student Health members. You can view these edits on our Availity provider portal.*
For coding changes, go to Aetna Payer Space > Resources > Expanded Claim Edits
With the exception of Student Health, you’ll also have access to our code edit lookup tools. To find out if our new claim edits will apply to your claim, log in to the Availity provider portal. You’ll need to know your Aetna® provider ID number (PIN) to access our code edit lookup tools
Aetna on Pre-certs

Submitting Precertification Request
Be sure to submit precertification requests at least two weeks in advance. To save time, request precertification online. Doing so is fast, secure and simple.
You can submit most requests online through our Availity provider portal.* Or you can use your practice’s Electronic Medical Record (EMR) system if it’s set up for electronic precertification requests. Use our “Search by CPT® code” search function on our precertification lists page to find out if the code requires precertification.**
Just in Aetna OfficeLink Update
Changes to Aetna’s Commercial drug list BEGIN ON JULY 1st
“On July 1, 2023, we’ll update our pharmacy drug lists. Changes may affect all drug lists, precertification, step therapy and quantity limit programs.
You’ll be able to view the changes as early as May 1. They’ll be on our Formularies and Pharmacy Clinical Policy Bulletins page.”
Ways to request a drug prior authorization:
- Submit your completed request form through our Availity provider portal.*
- For requests for non-specialty drugs, call 1-800-294-5979 (TTY: 711). Or fax your authorization request form (PDF) to 1-888-836-0730.
- For requests for drugs on the Aetna Specialty Drug List, call 1-866-814-5506 or go to our Forms for Health Care Professionals page and scroll down to the Specialty Pharmacy Precertification (Commercial) drop-down menu. If the specific form you need is not there, scroll to the end of the list and use the generic Specialty Medication Precertification request form. Once you fill out the relevant form, fax it to 1-866-249-6155.
For more information, call the Provider Help Line at 1-800-AETNA RX (1-800-238-6279) (TTY: 711).

Aetna Update August 2022

Effective 11/1/2022
Computer-assisted surgical and musculoskeletal navigation coding update.
Aetna® will no longer consider the following codes for separate reimbursement:
• 20985 (Computer-assisted surgical navigational procedure for musculoskeletal procedures, image-less (List separately in addition to code for primary procedure))
• 0054T (Computer-assisted musculoskeletal surgical navigational orthopedic procedure, with image-guidance based on fluoroscopic images (List separately in addition to code for primary procedure)). The use of computer-assisted surgical navigation is considered
integral to the performance of the procedure.
There is a New Player in the Game


EMI Health is proud to provide access to the Aetna network.
Each member will have a medical identification card with the EMI Health and Aetna logos.
Aetna 3rd-Party Claim and Code Review
Beginning June 1, 2022, you may see new claim edits.
According to March 1, 2022 Aetna OfficeLink Updates: These are part of our Third-Party Claim and Code Review Program. These edits support our continuing effort to process claims accurately for our commercial, Medicare and Student Health members. You can view these edits on our Availity provider portal.*
You can view any of these edits on Aetna’s Availity® provider portal.
For coding changes, go to:
- Aetna Payer Space
- Resources
- Expanded Claim Edits
Except for Student Health, you’ll also have access to Aetna’s code edit lookup tools. To find out if our new claim edits will apply to your claim, log in to our Availity provider portal. You’ll need to know your Aetna® provider ID number (PIN) to access our code edit lookup tools
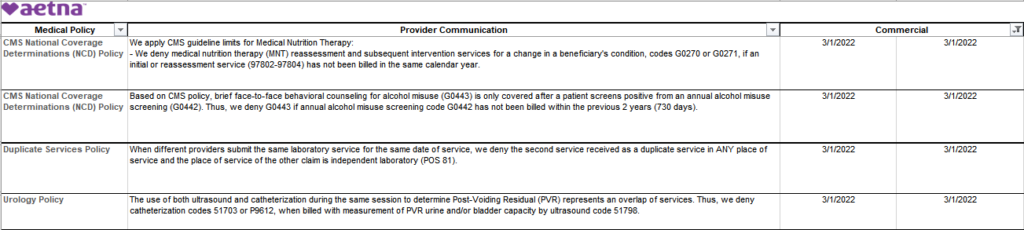
Here is what POET found with 2022 effective dates:
Aetna, No Longer Paying Office Consult

*ALERT*
Starting March 1, 2022, Aetna will no longer pay office consultation codes 99241 – 99245
*ALERT*
Aetna OfficeLink Updates, December 1, 2021
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2021/12/Aetna-Newsletter-2021.12.01.pdf” download=”all” viewer=”google”]
Aetna OfficeLink Updates 9/1/2021

Aetna is going paperless. Here is how to get your electronic EOB Statements and Payments.
Starting in September through 2022, we’re phasing out paper Explanation of Benefits (EOB) statements and checks. Sign up before it’s your turn. If you don’t enroll to receive direct deposit payments, you may receive future payments by virtual credit card. Keep reading to learn more.
Get EOB statements from Availity®
Register for our provider portal on Availity. Get identical copies of your EOB statements from the Availity Remittance Viewer. Then print or save them to your computer. You won’t need to wait for them to arrive in the mail.
Sign up for direct deposit payments
Sign up for direct deposit payments using our new portal, Payer Enrollment Services. Just goto Payer Enroll Services. We’ll stop using EnrollHub® effective September 1. Even if you’re
already enrolled to receive direct deposit payments (or electronic remittance advice), use the new portal to make changes.
Visit AetnaPaperlessOffice to learn more about your options
Third Party Claim and Code Review Program
Beginning December 1, 2021, you may see new claim edits. These are part of our Third Party Claim and Code Review Program. These edits support our continuing effort to process claims accurately for our commercial and Medicare members. You can view these edits on our provider portal.
We may request medical records for certain claims, such as high-dollar claims, implant claims and bundled-services claims, to help confirm coding accuracy.
You’ll have access to our prospective claims editing disclosure tool. To find out if our new claim edits will apply to your claim, log in to the Availity provider portal. Once there, go to Aetna’s Payer Space > Applications > Code Edit Lookup Tools. You’ll need to know your Aetna® provider ID number (PIN) to use the tools.
For all coding changes, go to Aetna Payer Space > Resources > Expanded Claim Edits
Recent Comments