Tag: Blue Cross Blue Shield (BCBS)
Updated Clinical Prior Authorization
Assistance Chart Now Available
An update to the Clinical Prior Authorization Assistance Chart is available. The chart identifies which clinical prior authorization each MCO uses and whether the MCO uses all or some of the steps in the evaluation process.
Help Identifying BCBS cards
The following Network IDs only apply to cards that show the TDI indicator.
This shows the plan is fully funded and regulated by TDI (Texas Department of Insuarnce).
- Blue Choice PPOSM= BCA.
- Blue EssentialsSM = HMO.
- Blue Advantage HMOSM = BAV.
- Blue PremierSM = HMH.
- MyBlue HealthSM = BFT.
- Blue High Performance (BlueHPN) = HPN
Example of Blue EssentialsSM
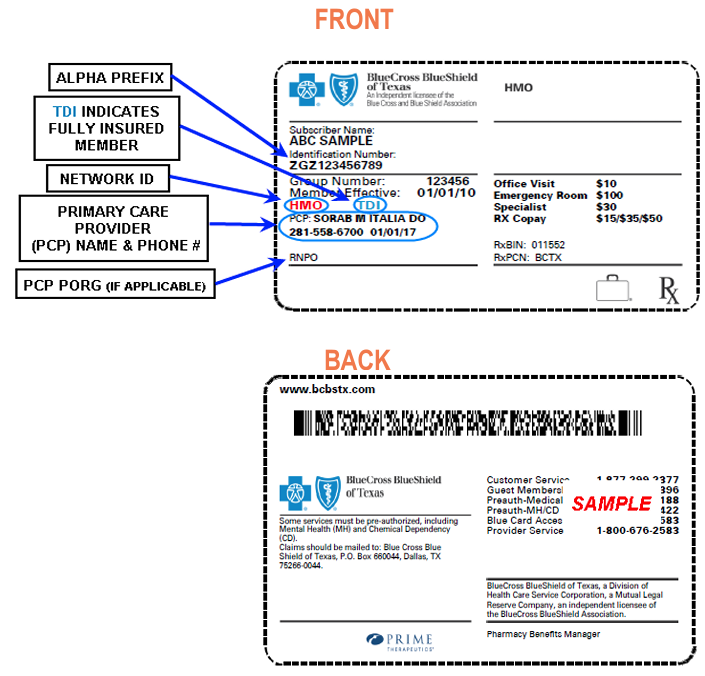
Note the red letters “HMO” and blue letters “TDI” on the card. This is what makes it a Blue Essentials Card.
However, with the ever-changing insurance landscape,
We highly encourage you to check Eligibility and Benefits.
It is advisable to retain any information you view, for your office to have the documentation you
need when a claim does not pay correctly or does not pay at all.
REMEMBER: IT HAS TO HAVE THE TDI INDICATOR
BCBS RSV Vaccine Update
Sept. 1, 2023
RSV Vaccine Coverage Update
Applies to all non-grandfathered groups
Beginning Sept. 1, 2023, we will cover the Respiratory Syncytial Virus (RSV) vaccine without cost sharing for adults, as recommended by the Advisory Committee on Immunization Practices (ACIP).
- This year, the Food and Drug Administration (FDA) approved two new RSV vaccines, Abrysvo and Arexvy, for the prevention of lower respiratory tract disease caused by RSV in those age 60 and older.
- We will cover both RSV vaccines without cost sharing when obtained at a doctor’s office (as a medical claim) or at a participating pharmacy (as a pharmacy claim) for groups that have Prime® Therapeutics as their Pharmacy Benefits Manager (PBM).
- Groups that have carved-out pharmacy benefits should check with their PBM to confirm their coverage and implementation of this update.
- As with any preventive service, the vaccine must be obtained from an in-network provider to be covered without cost sharing.
- This coverage update is effective Sept. 1, regardless of renewal date for all non-grandfathered ACA-compliant plans.
Note: The RSV vaccine for infants (Beyfortus) is a different drug and is covered under the medical plan only.
Blue Cross and Blue Shield of Texas (BCBSTX) contracts with Prime Therapeutics to provide pharmacy benefit management and related other services. BCBSTX, as well as several independent Blue Cross and Blue Shield Plans, has an ownership interest in Prime Therapeutics. MyPrime.com is an online resource offered by Prime Therapeutics.
BCBS Pharmacy Quarterly Update
Changes Effective October 1, 2023
BCBS June 1, 2023 HCPCS Update
POET has had a number of request regarding the BCBS Quarterly HCPCs Update.
You may use Ctrl + F to search or download the entire document.
CHI Has A New Card
It has been reported that CHI has a new name on their card.

BCBS Drug Fee Schedule
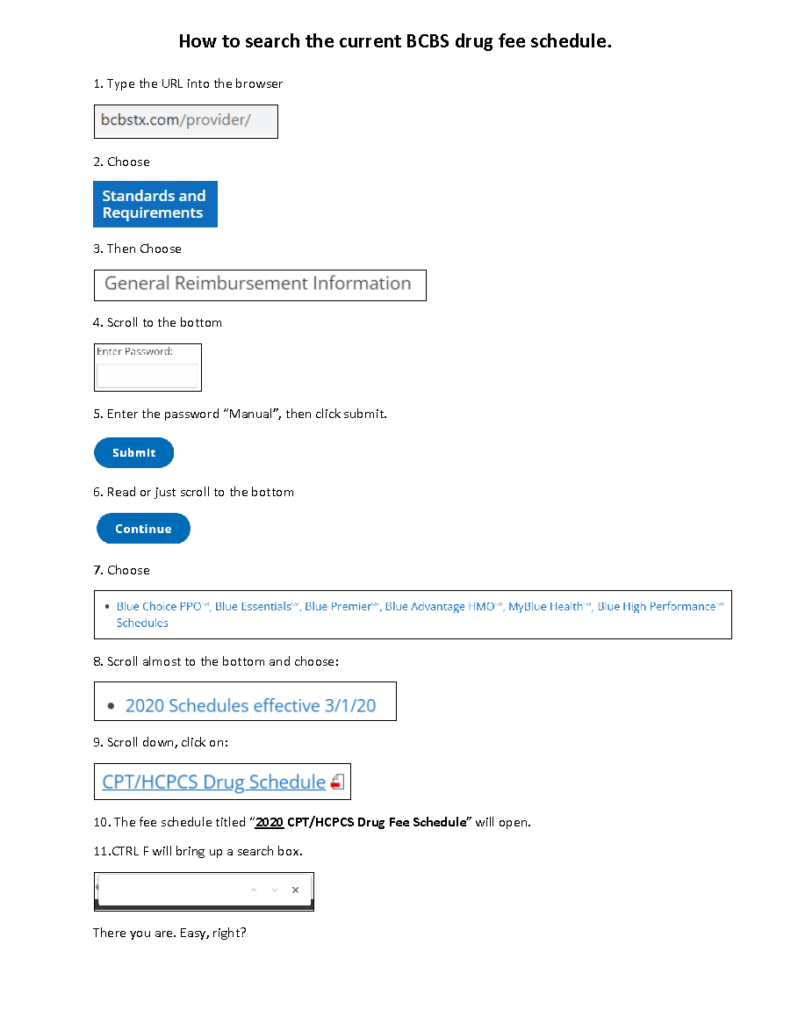
HOW TO SEARCH THE CURRENT BCBS DRUG FEE SCHEDULE (UPDATED QUARTERLY)
Updated 5/2/2022. You can use CTRL F to bring up a search box. Then just enter the code you are looking for.
BCBS News for Employer Groups
HealthSelect ERS

Effective Sept. 1, 2021, HMO plans will no longer be an enrollment option under the Texas Group Benefit Program. All current subscribers and dependents enrolled in one of the HMO plans will be automatically enrolled in HealthSelect of Texas administered by Blue Cross and Blue Shield of Texas, unless they elect otherwise during their summer enrollment period
Participants who are transitioning from an HMO plan will have a 90-day referral grace period and will receive in-network benefits if they see an in-network specialist without a referral during this timeframe. After Nov. 30, 2021, if there is not a referral on file with BCBSTX, the specialist visit will be covered at the out-of-network benefit level, even if the specialist is in-network.
Effective Sept. 1, 2021, certain procedure codes are being removed from the list of services that require prior authorization for HealthSelect of Texas® & Consumer Directed HealthSelectSM participants. You can review a list of the codes being removed here ![]() . BCBSTX is currently working on system updates to reflect this change.
. BCBSTX is currently working on system updates to reflect this change.
Remember to use Availity®![]() or your preferred vendor to check eligibility and benefits before rendering services. This will help you confirm coverage details and prior authorization requirements and determine if you are in-network for the member’s policy. Refer to Eligibility and Benefits for details.
or your preferred vendor to check eligibility and benefits before rendering services. This will help you confirm coverage details and prior authorization requirements and determine if you are in-network for the member’s policy. Refer to Eligibility and Benefits for details.



Recent Comments