Tag: Drug Coverage
Just in Aetna OfficeLink Update
Changes to Aetna’s Commercial drug list BEGIN ON JULY 1st
“On July 1, 2023, we’ll update our pharmacy drug lists. Changes may affect all drug lists, precertification, step therapy and quantity limit programs.
You’ll be able to view the changes as early as May 1. They’ll be on our Formularies and Pharmacy Clinical Policy Bulletins page.”
Ways to request a drug prior authorization:
- Submit your completed request form through our Availity provider portal.*
- For requests for non-specialty drugs, call 1-800-294-5979 (TTY: 711). Or fax your authorization request form (PDF) to 1-888-836-0730.
- For requests for drugs on the Aetna Specialty Drug List, call 1-866-814-5506 or go to our Forms for Health Care Professionals page and scroll down to the Specialty Pharmacy Precertification (Commercial) drop-down menu. If the specific form you need is not there, scroll to the end of the list and use the generic Specialty Medication Precertification request form. Once you fill out the relevant form, fax it to 1-866-249-6155.
For more information, call the Provider Help Line at 1-800-AETNA RX (1-800-238-6279) (TTY: 711).

Seasonal Influenza Vaccines Pricing
The Medicare Part B payment allowance limits for seasonal influenza (flu) vaccines are 95% of the Average Wholesale Price (AWP), as reflected in the published compendia.
In hospital outpatient departments, payment is based on reasonable cost.
Annual Part B deductible and coinsurance amounts don’t apply for the influenza virus vaccinations. All physicians, non-physician practitioners, and suppliers who administer these vaccinations must take assignment on the claim for the vaccine.
Annual Influenza Vaccine season starts on August 1 and ends on July 31 of the following year.
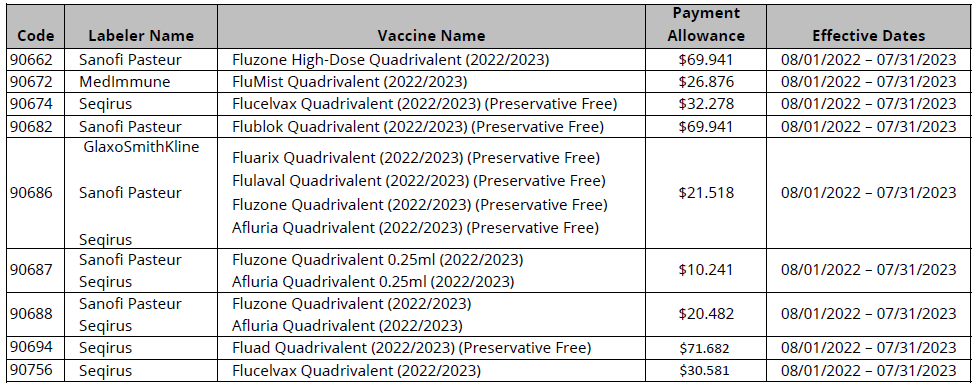
Payment Allowances and Effective Dates by Flu Season
UHC October 2021 Policy & Protocol Updates
UHC Network News Brief 10/1/2021
Catch All the UHC UPDATES
October 2021 Policy and Protocol Updated Overview
- Medical policy update: October 2021
- Pharmacy Updates
- Prior Authorization and Notification Requirement Updates and 2021 Summary of Changes
- Reimbursement Policy Updates: October 2021
- Specialty Medical Injectable Drug Program Updates: October 2021
CPT Code ready for 3rd Dose of Moderna
Flu, Pneumococcal, and Hepatitis B
UHC Network Bulletin Overview 8/2021
Your NOTICE of protocol
and policy changes
from UnitedHealthcare
Medical policy updates: August 2021
This month, you’ll find updates for Medicaid, Medicare, Exchange and commercial plans.
Prior authorization and notification requirement updates
We’re making changes to certain advance notification and prior authorization requirements that are available for you in the 2021 Summary of Changes.
Reimbursement policy updates: August 2021
This month, you’ll find updates for Medicaid and commercial plans.
Specialty Medical Injectable Drug program updates: August 2021
See the latest updates to requirements for Specialty Medical Injectible Drugs for UnitedHealthcare members.
Prior authorization code updates for commercial plans
Effective Nov. 1, 2021, we are adding new codes to the prior authorization list for UnitedHealthcare commercial plans including All Savers, River Valley, Neighborhood Health Partnership, UnitedHealthcare West, MidAtlantic Health Plans






Recent Comments