Tag: EDI Claim Edits
Highlights for Aetna OfficeLink Updates
Claim and Code Review Program (CCRP) update
Starting December 1, you might see new claim edits
This update applies to both our commercial and Medicare members.
Beginning December 1, 2025, you may see new claim edits. These are part of our CCRP. These edits support our continuing effort to process claims accurately for our commercial, Medicare and Student Health members. You can view these edits on our provider portal on Availity.
For coding changes, go to Aetna Payer Spaces > Resources. In the search bar, search for “expanded claim edits.”
Except for Student Health, you’ll also have access to our code edit lookup tools. To find out if our new claim edits will apply to your claim, log in to Availity®. You’ll need to know your Aetna® provider ID number (PIN) to access our code edit lookup tools.
We may request medical records for certain claims, such as high-dollar claims, implant claims, anesthesia claims, and bundled services claims, to help confirm coding accuracy.
Changes to our National Precertification List (NPL)
These changes apply to our commercial and Medicare members, unless otherwise noted.
Effective January 1, 2026, we’ll require precertification for the following:
• Electrophysiological (EP) study (93654)
• Yondelis® (trabectedin, J9352)
• Docivyx™ (docetaxel, J9172) — Medicare members only
Check out the Original Publication, titles like:
- How to secure an authorization
- Urgent requests
- Changes to commercial drug lists begin on January 1
- And More
Aetna 3rd-Party Claim and Code Review
Beginning June 1, 2022, you may see new claim edits.
According to March 1, 2022 Aetna OfficeLink Updates: These are part of our Third-Party Claim and Code Review Program. These edits support our continuing effort to process claims accurately for our commercial, Medicare and Student Health members. You can view these edits on our Availity provider portal.*
You can view any of these edits on Aetna’s Availity® provider portal.
For coding changes, go to:
- Aetna Payer Space
- Resources
- Expanded Claim Edits
Except for Student Health, you’ll also have access to Aetna’s code edit lookup tools. To find out if our new claim edits will apply to your claim, log in to our Availity provider portal. You’ll need to know your Aetna® provider ID number (PIN) to access our code edit lookup tools
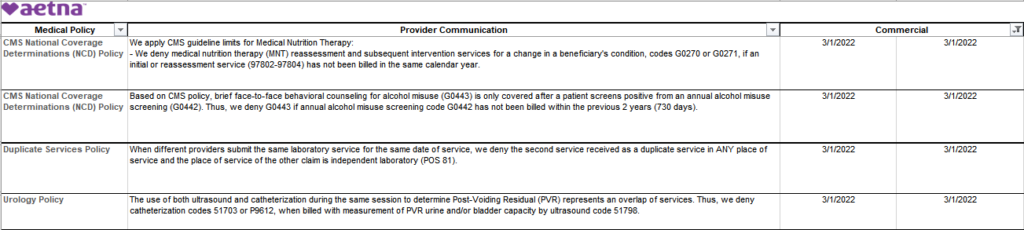
Here is what POET found with 2022 effective dates:
UHC New EDI Edits for MA Claims

EDI claim edits now notify you of missing or mismatched information.
As of Aug. 28, 2021, the new payer-level edits for Electronic Data Interchange (EDI) 837 claim submissions provide alerts of specific information that may be missing or doesn’t match data contained in our systems.
How will you be notified of claim issues?
Claims that are rejected for these edits will appear on your claims rejection report, also known as a 277CA report. UHC is no longer mailing letters about claim submissions that need attention. Instead, your clearinghouse will be responsible for notifying you of any issues.
What do you need to do?
Ensure you are receiving these messages from your clearinghouse. Claims that are rejected should be corrected and resubmitted electronically to be accepted into our processing system for adjudication.
Recent Comments