Tag: Insurance
TRS 2025-2026 Plan Year
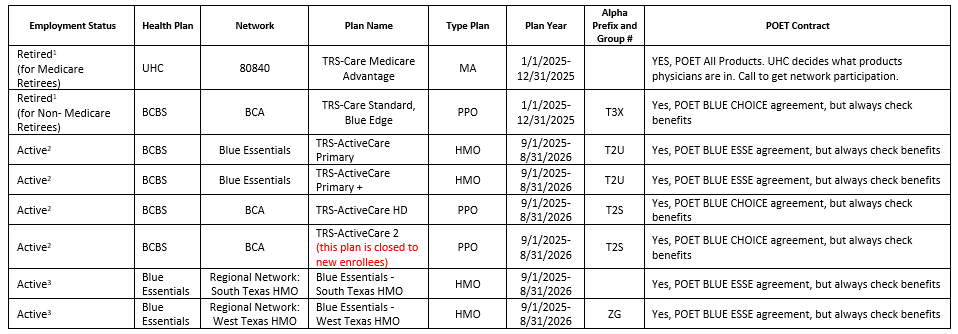
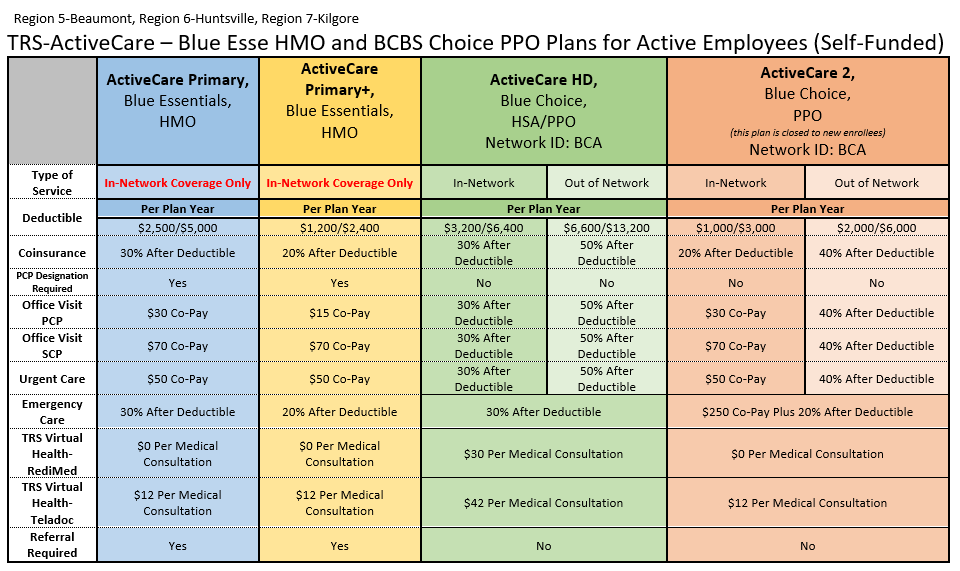
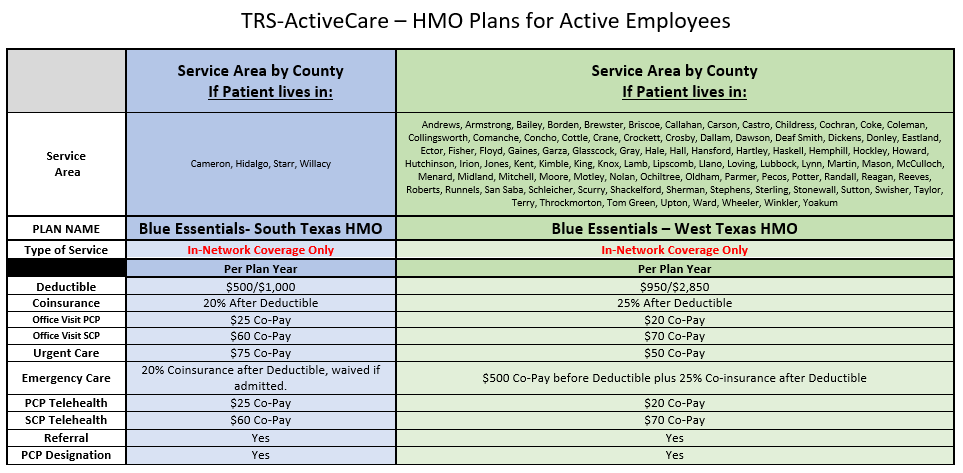
Products for 2025-2026 Plan Year
Please be aware the Retiree Plans are Calendar Year
MRC Contract Term 1/1/2022

Today March 28th, POET has received an official letter terminating the Methodist Retirement Community (MRC) direct contract. Termination was effective 1/1/2022.
MRC is now utilizing BCBS of Texas
Check Those Checks!!!

- Don’t get caught in this dirty deal.
- Know what you are endorsing.
- If you receive payment with no patient information this should be a red flag.
- By endorsing you could be agreeing to accept whatever payment they wish to send.
- Your endorsement could also serve as an authorized signature for contract.
6 Keys to Addressing Denials
6 keys to addressing denials in your medical practice’s revenue cycle
MGMA STAT – MARCH 18, 2021
The Medical Group Management Association’s most recent MGMA Stat poll asked healthcare leaders, “Has your organization seen denials increase in 2021?”
- 69% said “yes.”
- 31% said “no.”
Common responses from respondents included payers not reimbursing for codes related to COVID-19 supplies, critical care claims and imaging CTs.
For those healthcare leaders who reported an increase in denials, the average increase in denials was 17%.
- Half responded that they increased by 1% to 10%.
- 34% said 11% to 20%.
- 12% who stated 21% to 30%.
The poll was conducted March 16, 2021, with 576 applicable responses.
For great tips and strategies to use, follow this link or visit “The Business End” folder located in the InK files.
Reimbursement Policy Update Bulletin: UHC March 2021
UHC releases revised reimbursement policies for: Outpatient Hospital, Laboratory Services and Emergency Department E/M.
Health Plan Representatives
Health Plan Representatives Updated 2/25/2021
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2021/02/Health-Plan-Representatives-2021.02.25.pdf” download=”all” viewer=”google”]
Humana PPO (POET) Plan Breakout
Humana PPO Plans have National Network Reciprocity, allowing members to travel with the comfort of knowing they can use any Humana ChoiceCare PPO Network Provider across the county for in-network services.
Humana PPO Plan Breakout 10/1/2020
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2020/10/Humana-Plan-Breakout-10012020-1.pdf” download=”all” viewer=”google”]
Senate Bill 1264: Protecting consumers from surprise medical bills
Texas Insurance Commissioner Kent Sullivan is reminding insurers of their obligations under the state’s new baseball-style arbitration law to resolve disputes on many out-of-network medical bills.
In a letter Tuesday addressed to “the health plans of Texas,” Mr. Sullivan said the Texas Department of Insurance (TDI) will monitor how health plans implement Senate Bill 1264, passed during last year’s session of the Texas Legislature and now in effect.
“We expect you to be proactive to meet both the letter and spirit of SB 1264,” Mr. Sullivan said. “Review your policies and procedures and address potential issues quickly.”
The letter highlighted several of the plans’ responsibilities in relation to the law. The commissioner’s letter noted that:
- State law requires plans to cover medical screenings necessary to rule out the presence of an emergency condition;
- For emergency care, claim denials based on failure to meet the prudent-layperson standard must be based on the patient’s presenting symptoms, not on the later diagnosis code;
- Plans must meet required deadlines to promptly adjudicate clean claims; and
- Plans must be ready to provide accurate information about the new law, including required notices about mediation and arbitration, on explanations of benefits. The plans must be able to quickly respond to questions from policyholders and practitioners.
Mr. Sullivan’s letter noted that TDI has set up an SB 1264 page on its website, which includes a link to the state’s new portal for mediation and arbitration requests.
The Texas Medical Association has published a brief overview of the new law for physicians.
Last Updated On
January 09, 2020
Joey Berlin
Recent Comments