Tag: Insurance Cards
Information relating to Insurance cards
CIGNA MA Information Update from POET

POET has received a few calls regarding the Cigna MA PPO plan that came into effect January 1, 2022.
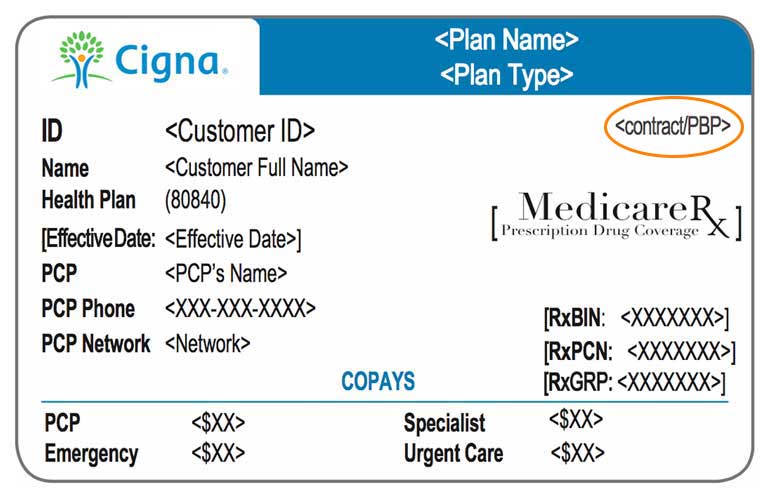
- To the left is a screen shot of one PPO product’s card. (I’m sorry it is not to pretty.)
- No PCP is required.
- Referrals are not required
- Providers are still responsible for receiving PRIOR AUTHORIZATION.
You may have noticed the Cigna MA insurance card no longer sports the “HealthSpring” Logo.

The below list are for Provider use only. Not to be distributed to Patients
HMO Customer Benefit Plans for Our Service Area
PPO Customer Benefit Plans for Our Service Area
- Cigna Preferred Medicare HMO
- H4513-061-001
- CignaTotalCare HMO D-SNP
H4513-060-001 - Cigna Fundamental Medicare HMO H4513-009-000
- Cigna Preferred Savings Medicare HMO
H4513-066-000
- Cigna True Choice Medicare PPO
H7849-038-000 - Cigna True Choice Plus Medicare PPO
H7849-062-000
HealthSpring Insurance Card

You may have noticed the Cigna MA (HMO) insurance card no longer sports the “HealthSpring” name.
Here is a tip.
There are only three customer benefit plans (HMO) for our service area.
- 2021-TX-H4513-061-Preferred (HMO) – Medicare A, B, & D coverage
- 2021-TX-H4513-060-TotalCare (HMO DSNP) – Medicare/Medicaid A, B, & D coverage
- 2021-TX-H4513-009-Fundamental (HMO) – Medicare A & B coverage only (no part D); formerly known as the Advantage plan
Where you see “contract/PBP” with the orange circle around it, the card for our service area should have either H4513-061, H4513-060 or H4513-009. Any other number would suggest the patient is out of their service are.
More on Medicare MBI
New Medicare Card: If an MBI Changes
From CMS MLN Connects November 2019
Medicare beneficiaries or their authorized representatives can ask to change their Medicare Beneficiary Identifiers (MBIs); for example, if the MBI is compromised. CMS can also change an MBI. It is possible for your patient to seek care before getting a new card with the new MBI.
If you get an eligibility transaction error code (AAA 72) of “invalid member ID,” your patient’s MBI may have changed.
- Do a historic eligibility search to get the termination date of the old MBI.
- Get the new MBI from your Medicare Administrative Contractor’s secure MBI look-up tool. Sign up for the Portal to use the tool.
Reminders about using the old or new MBIs:
Fee-For-Service (FFS) claims submissions with:
- Dates of service before the MBI change date – use old or new MBIs
- Span-date claims with a “From Date” before the MBI change date – use old or new MBIs
- Dates of service that are entirely on or after the effective date of the MBI change – use new MBIs
FFS eligibility transactions when the:
- Inquiry uses new MBI – we will return all eligibility data.
- Inquiry uses the old MBI and request date or date range overlap the active period for the old MBI – we will return all eligibility data. We will also return the old MBI termination date.
- Inquiry uses the old MBI and request date or date range are entirely on or after the effective date of the new MBI – we will return an error code (AAA 72) of “invalid member ID.”
See the MLN Matters Article for more information on how to get and use MBIs.
Recent Comments