Tag: Medical Group Management Association (MGMA)
The Most Asked Questions About Medical Coding Audits Following the 2021 E/M and MDM Changes ~MGMA
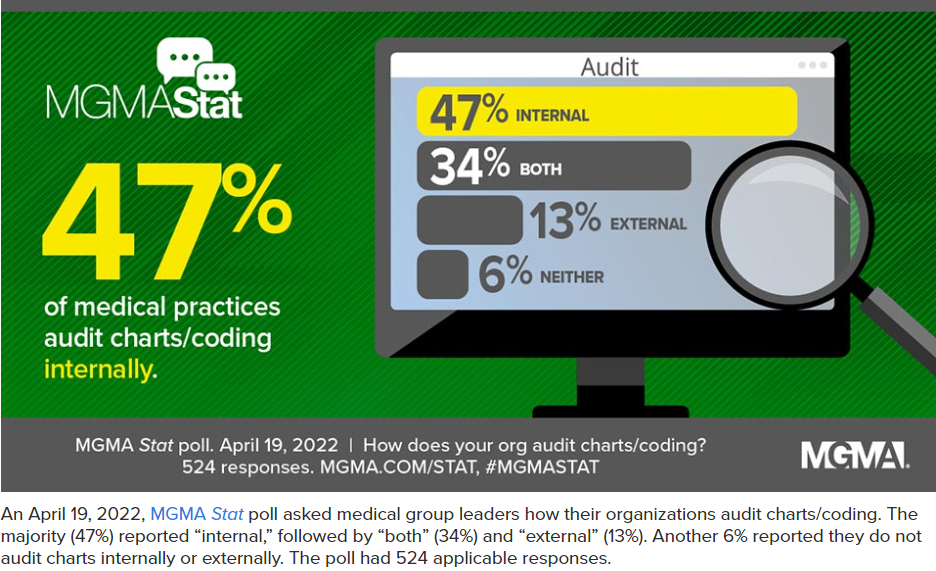
In the above linked article you will find:
- What E/M Updates to Watch
The definition of “external” for purposes of reviewing data as part of MDM.
What is time-based coding?
Documentation Tips
- And More

Paying to Get paid!

The Centers for Medicare & Medicaid Services (CMS) released new guidance that seeks to clarify requirements
for electronic funds transfers (EFT).
Although this guidance does not address all of MGMA’s questions and concerns (see MGMA’s letter to CMS), we are encouraged that CMS heeded our call to issue additional guidance and that CMS acknowledged in this guidance that a health plan may not adversely affect or attempt to adversely affect a provider, should a provider desire to receive EFT using a standard transaction
MGMA has voiced concerns to CMS that the business associates that health plans use to render payments to practices levy fees on the transaction. We are adamant that these ‘pay to get paid’ schemes are unacceptable and that CMS should prohibit these abuses. Although the guidance does not explicitly address these fees, it does clearly state that health plans cannot require providers to receive payment from its business associates. In essence, as we understand it, the fact that a plan cannot require a practice to agree to receive payment from its business associates should allow practices to forgo interacting with these vendors and thus avoid the fees.
MGMA is seeking further clarity on this guidance and stands firm on our belief that health plans and their business associates should be forbidden from levying these fees on medical groups.
It’s Only Money

APRIL 1, 2022
$$$
Medicare sequester begins to phase back in at 1%
$$$
Surprise Billing FAQs, MGMA
Still confused about Good Faith Estimates (GFE)?
Does Qualifying Payment Amount (QPA) sound like Greek?
Question Posed Regarding New POS 10
One Person Reaches out to MGMA for Advice:
“I need confirmation regarding the new POS 10. The new POS code 10 and the revision to POS code 02 goes into effect on April 4, 2022 (Medicare), and January 1, 2022, respectively. After the effective date, POS code 10 will be used if a patient receives telehealth at home, and POS code 02 will only be used for the other eligible originating sites (in other words, other places besides a patient’s home where a patient may be located and receive telehealth services that may be reimbursed by Medicare).
It is my understanding that the POS 10 would only be used for mental health/substance abuse telehealth services as they are the only services that will be covered if provided at home.
Should practices continue to use POS 02 until the PHE officially ends or should they begin using POS 10 (January 1, 2022 for all payers except for Medicare) and April 4, 2022 for Medicare? “
Claire Ernst J.D., Government Affairs Director MGMA, Washington DC. Responds:
“Thank you for your question. When I saw CMS’ notice about the revised POS codes in October, I had the same question. My assumption is that POS 10 should be used for the new mental health telehealth services, but most likely once the COVID-19 PHE ends. The mental telehealth expansion provided in the Consolidated Appropriations Act, 2021 (CAA) and subsequently codified in the 2022 final Medicare Physician Fee Schedule (PFS) allows for mental health services to be rendered to patients in their homes (with some conditions). Although this was covered in the 2022 PFS, the mental telehealth expansion provision in the CAA was meant to allow for providers to continue treating patients for mental health conditions from the home following the conclusion of the PHE. Practitioners can continue providing care to patients in their homes through the end of the PHE and will be reimbursed at the in-person rate if the 95 modifier is used.
I reached out to the staff at CMS to confirm, but have not heard back yet. I will follow up with them again and provide any feedback in this thread”
CoVid Vaccine Mandate, Update

ADVOCACY RESOURCE – DECEMBER 2, 2021

Claire Ernst J.D.
Government Affairs Director MGMA
Washington DC
MGMA Legislative Alert
POSTED 12/9/2021 6:51 PM


Coding and Billing Compliantly for APPs, MGMA
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2021/12/MGMA-2021-billing-for-APPs.pdf” download=”all” viewer=”google”]
MGMA, Update on the Court Cases Involving CoVid-19 Vaccination Mandates.
Per Claire Ernst J.D., Government Affairs Director MGMA
“I wanted to provide a quick update on the court cases involving the COVID-19 vaccination mandates. As many of you have seen, both the OSHA vaccination and testing emergency temporary standard (ETS) and the CMS facilities vaccination mandate were quickly challenged in court. Below is a quick overview of where the mandates currently stand – this is subject to change:
- OSHA vaccination and testing ETS: On Nov. 12, 2021, the U.S. Circuit Court of Appeals for the Fifth Circuit granted a motion to stay (or halt) the ETS. After that decision, OSHA suspended enforcement pending future developments in the litigation. More information about OSHA’s announcement can be found on the ETS landing page. The U.S. Court of Appeals for the Sixth Circuit now has jurisdiction over the challenges and will issue its decision. However, it is certainly possible that following the Court’s ruling, the decision could get appealed to the U.S. Supreme Court.
- CMS facilities vaccination mandate: On Nov. 30, 2021, the U.S. District Court for the Western District of Louisiana issued a preliminary injunction halting the mandate. The ruling comes one day after the U.S. District Court for the Eastern District of Missouri halted implementation of the rule for 10 states. Together, the decisions apply to all states. However, this decision is likely to get appealed as well.
MGMA will continue to monitor this evolving situation and provide updates.”

Recent Comments