Tag: Prior Authorization
AIM Specialty Health (AIM) to Perform Utilization Management for:
Participants with three-character prefixes of T2U and T2S (Group #3850X -last digit varies by plan) who are under 65 years of age and are active employees.
This is referring to TRS ActiveCare Patients.
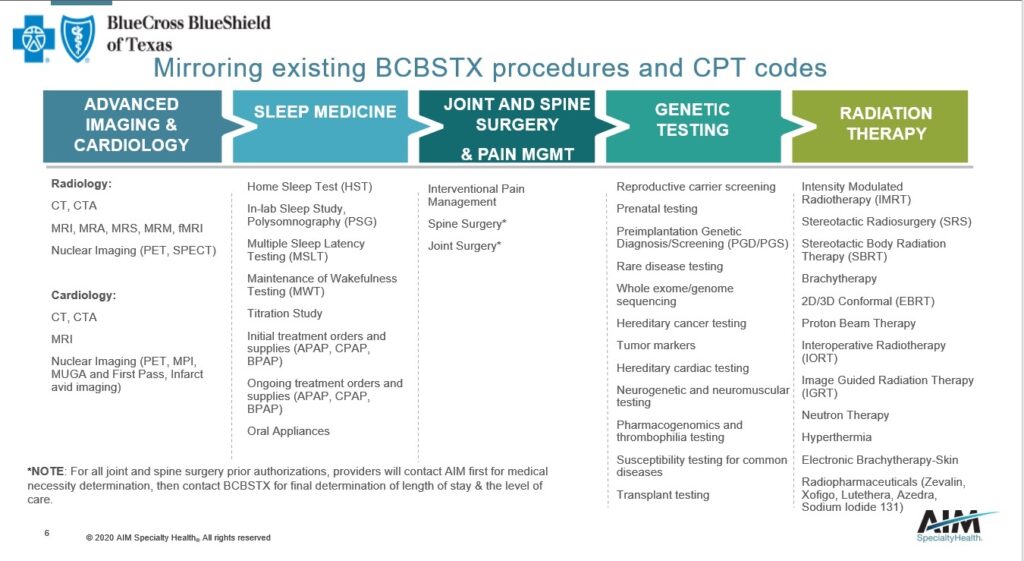
To log in to “AIM” click the blue text.
To review the “AIM” training slide deck, click here.
UPCOMING Provider/Portal Training Dates
- Advanced Imaging & Cardiology: Tuesday, Sept. 15 (10 AM-11 AM)
- Sleep Medicine: Wednesday, Sept. 16 (12 PM-1 PM)
- Joint and Spine Surgery:Thursday, Sept. 17 (12 PM-1PM)
- Pain Management: Tuesday, Sept. 15 (9 AM-10 AM)
- Radiation Therapy: Thursday, Sept. 17 (3 PM-4PM)
- Genetic Testing Services: Tuesday, Sept. 15 (12 PM -1 PM)
UHC Provider Resources Regarding the “Link” Portal. Received by POET on 7/1/2020
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2020/07/Service-Model-Flyer-TX-OK-Rcvd-by-POET-on-07012020.pdf” download=”all” viewer=”google”]
Cigna MA PCP Newsletter June 2020
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2020/06/June-PCP-E-Newsletter-06152020.pdf” download=”all” viewer=”google”]
Cigna HealthSpring PCP Newsletter June 2020
· Social Determinants of Health (SDOH)
· 2020 Medicare Advantage Prior Auth (PA) Requirements
· CoverMyMeds.com
· Valuable Insights:COVID-19 Resources
· CAHPS Corner: COVID-19 Updates
UnitedHealthCare Resourses to Aid Claim Submissions and Processing 04272020
To help you manage the claim submission and reimbursement process with UnitedHealthcare, as well as access the CARES ACT funding available to health care professionals, here’s a summary of resources to address your most common questions and concerns. Use this link to view the list.
UnitedHealthCare Resourses to Aid Claim Submissions and Processing 04272020
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2020/04/UnitedHealthCare-Resourses-to-Aid-Claim-Submissions-and-Processing-04272020.pdf” download=”all” viewer=”google”]
Blue Cross Blue Shield of TX will Manage all Prior Authorizations for HealthSelect, Effective March 1, 2020
There are important changes to the prior authorization requirements for the HealthSelect of Texas and Consumer Directed HealthSelect plans administered by BCBSTX. The list of services requiring prior authorization has not changed; however, beginning March 1, 2020, prior authorizations for services previously managed by eviCore healthcare® will now be managed through BCBSTX.
For more information visit the BCBS file.
BCBS will Manage all Prior Authorizations for HealthSelect, Effective March 1, 2020
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2020/02/HealthSelect-Prior-Auth-Transition-Provider-Communication-02242020.docx” download=”all” viewer=”microsoft”]
Recent Comments