Tag: Reimbursement Updates
UHC December Monthly Overview
Key changes for our Medicare Advantage plan
- In 2026, most UnitedHealthcare Medicare Advantage health maintenance organization (HMO) and point of service (POS) plans are referral plans. You can check plan referral requirements online.
- Starting Jan. 1, 2026, most members enrolled in UnitedHealthcare Medicare Advantage HMO/POS plans will be required to obtain a referral from their primary care provider (PCP) before accessing certain specialist services in outpatient, office or home settings. Referrals must be submitted by the PCP to UnitedHealthcare prior to the specialist visit. This also applies when members of HMO/POS plans are traveling and accessing the National Network. Learn more in our 2026 Medicare Advantage Referral Requirements Guideopen_in_new.
- Effective Jan. 1, 2026, new or existing members of UnitedHealthcare SNPs, including Chronic Special Needs Plans (C-SNP) and Dual Special Needs Plans (D-SNP), need a qualifying chronic condition to access benefits that cover healthy food and/or utilities. Providers may be contacted by UnitedHealthcare to verify a member has at least one qualifying condition to receive benefits. See 2026 Medicare Advantage, CSNP & DSNP Plan Overview Courseopen_in_new for more information.
UHC November Update
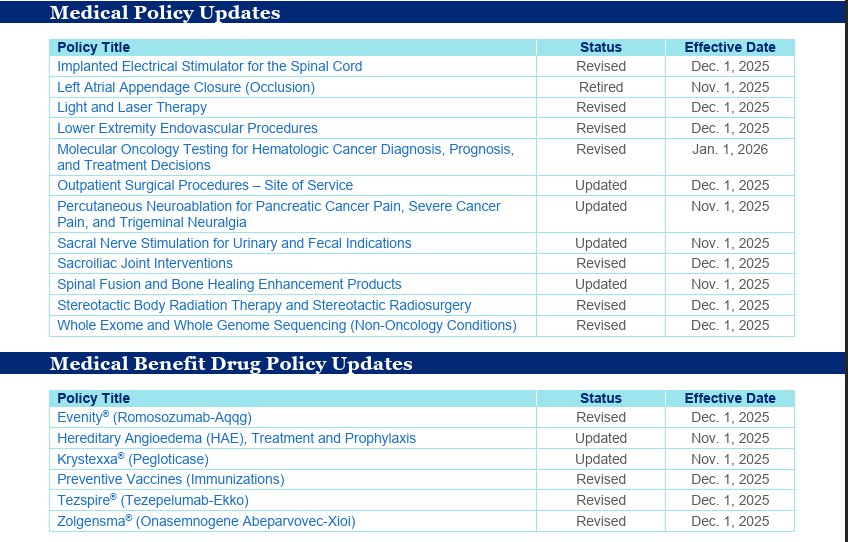
A list of recently approved, revised, and/or retired Medical Policies and/or Medical Benefit Drug Policies is provided below for your reference. For a comprehensive summary of the latest updates, refer to the Medical Policy Update Bulletin: November 2025.
Cigna Comm. New Reimbursement Policy for E/M

Cigna Healthcare® will implement a new reimbursement policy, Evaluation and Management Coding Accuracy (R49), to review professional claims billed with Current Procedural Terminology (CPT®) evaluation and management (E/M) codes 99204-99205, 99214-99215, and 99244-99245 for billing and coding accuracy in alignment with American Medical Association (AMA) E/M services guidelines.
Effective for dates of service on or after October 1, 2025, services may be adjusted by one level to reflect the appropriate reimbursement when the AMA guidelines are not met.
What this means to you
Cigna Healthcare will conduct periodic claim reviews to verify compliance. Based on that review, providers may be eligible to be removed from the program. Supporting documentation will be requested should we determine the established guidelines were not followed.
Reconsideration requests
Providers who believe their medical record documentation supports reimbursement for the originally submitted level for the E/M service should follow the reconsideration and appeals processes.
To request a reconsideration, please submit the customer’s full record of the encounter to the secure Cigna Healthcarefax number 833.392.2092. Should the original determination be overturned, claims will be adjusted, and an updated explanation of payment will be issued.
Administrative appeal rights are available if the original determination is upheld.

Recent Comments