Category: Business
Non-performers Impact on Performers

When an employee’s performance is consistently good, it becomes expected and may unknowingly be taken for granted.
I have seen people in leadership positions manipulate high-performing employees to produce more take on the burden of others while nothing is done to address the significant shortfall in the performance of other team members. At some point, this person will get burned out and lose all inspiration to continue performing at such a high level.
According to Tim McClure, when passionate employees become quiet, it usually signals that the work environment has become very dysfunctional. As a leader, this is something you must observe and act on immediately.
Please don’t push your most loyal people to the point that they no longer care. When you have people passionate, inspired, and motivated to help the company achieve its vision while fulfilling its purpose, you must do everything in your power to ensure that this team keeps this vibe. Otherwise, you run the risk of pushing away great talent while settling for mediocrity.
From LinkIn – Leadership First
The Power of the First Phone Call
“Patient satisfaction has become a key criterion by which to evaluate the
quality of healthcare services.
How make every call work for you.
Planning to Test for COVID?
You’ll Need a CLIA Waiver or Certification.
The fast-spreading omicron variant has pumped up demand for COVID-19 testing, and that means physician offices need to make sure they have obtained the correct waiver or certification from the U.S. government to administer those tests.
CoVid-19 News from UHC
Beginning Jan. 15, 2022, UnitedHealthcare is covering the cost of Food and Drug Administration (FDA)-authorized or approved over-the-counter (OTC) at-home COVID-19 diagnostic tests for Individual and Family Plan and Individual and Group Market health plan members.
- The national public health emergency has been extended from Jan. 15, 2022 to April 15, 2022. See how that extension affects temporary provisions for COVID-19 testing and testing-related visits:
- Currently there are 2 monoclonal antibody and 3 antiviral treatment options authorized or approved for use.
- Reminder: CMS Billing change effective 1/1/2022.
- Health care professionals who administer the COVID-19 vaccine serum or monoclonal antibody treatment to Medicare Advantage members should submit medical claims through the UnitedHealthcare standard claims process.
- For services rendered through Dec. 31, 2021, claims should be billed to the applicable Centers for Medicare & Medicaid Services (CMS) Medicare Administrative Contractor (MAC), as previously established for reimbursement of these claims
Employee Vaccinations
TMA Ask the Expert: Employee Vaccinations
“The rule does not apply to independent physician practice settings”
2022 Tech Trends from Iconic IT
The pandemic has sped everything up.
Here’s some of the big trends Iconic believes you’ll be seeing a lot more of in 2022:
1. Companies will invest more in cybersecurity insurance than ever before.
2. Cloud-based desktop software like Microsoft’s Cloud PC will grow in popularity.
3. Companies of all sizes will rely on SIEM cybersecurity defenses.
4. Mobile devices will become a bigger target for hackers.
With more employees than ever working remotely, they’re more likely to use poorly protected cell phones and computers on unsecured wifi. According to Digital Information World, 40 percent of mobile phones are prone to attack, and in need of better authentications and cybersecurity software.
5. AI-enabled cybersecurity software will help companies mitigate network threats in their networks, and the Internet of Things.
UnitedHealthCare Network News
Effective Feb. 4, 2022, UHC will no longer print and mail paper provider remittance advice (PRAs) for medical claims to network health care professionals.
UHC has updated their codes for the Outpatient Procedure Grouper (OPG) mapping. They have deleted 30 old codes and added 31 new codes. For more information follow this link.
Cigna Continues CoVid Accommodations
Over-the-counter testing
Consistent with new federal guidelines for private insurers, Cigna commercial will cover up to eight over-the-counter (OTC) diagnostic COVID-19 tests per month (per enrolled individual) with no out-of-pocket costs for the tests. This coverage began January 15, 2022 and continues through the end of the PHE (currently through April 15, 2022).
Please note that while Cigna Medicare Advantage plans do fully cover the costs for COVID-19 tests performed in a clinical setting, costs of at-home COVID-19 tests are not a covered benefit at this time.
Additionally, we encourage you to remind your patients that the Federal Government is now offering four free at-home test kits per household with no cost. Your patients can order the free at-home COVID-19 testing kits at COVIDtests.gov.
Coverage of COVID-19 treatments
As a reminder, Cigna commercial and Cigna Medicare Advantage cover FDA emergency use authorized (EUA) treatments of COVID-19, including monoclonal antibody treatments. This includes new antiviral medications PaxlovidTM and molnupiravir, as well as Remdesivir infusions when administered in an inpatient or outpatient setting.
Get all the most up-to-date information
We updated our dedicated COVID-19 provider web page on January 21, 2022 to highlight these updates more. You can also access the latest Cigna Medicare Advantage billing guidelines from this page. Please visit the site often to get the latest information.

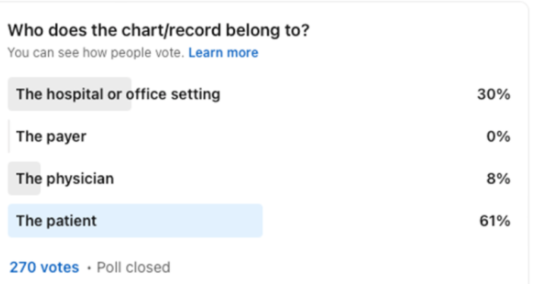
Recent Comments