Prevent Improper Code Bundling
Physicians can take advantage of a new Medicare tool to sort through service codes that can be bundled together for claims payment – and AVOID improper billing.
The CMS recently released the National Correct Coding Initiative (NCCI) procedure-to-procedure (PTP) lookup tool to promote accurate code-bundling and prevent improper payment of Medicare Part B and Medicaid claims when incorrect code combinations are reported.
Available via Texas’ Medicare contractor Novitas Solutions, the tool is further designed to help physicians identify when certain pairs of codes are subject to automated edits.
AND FOR EVEN MORE TOOLS
CLICK ON ANY OF THE BUTTONS BELOW
CIOX What Are Your Options

Did you say Cyclops?
Or was that Sick Ox?
No, Silly. CIOX
Medical records can be submitted through the following options:
1. PROVIDER PORTAL:
Upload the medical records to Ciox’s secure
provider portal at https://www.cioxlink.com
using the following credentials:
Username: C34765843
Password: eeE4^fe8
2. REMOTE EMR Retrieval:
Set up secure remote connection from a
provider site’s EMR directly to Ciox for timely
off-site remote retrieval of records with
trained associates at Ciox by
contacting 1-877-445-9293
3. ONSITE Chart Retrieval:
Schedule on-site retrieval with a complimentary Ciox
Chart Retrieval Specialist or review any aspects of the on-site retrieval services at Ciox by
contacting 1-877-445-9293
4.FAX:
Send secure faxes to 1-972-957-2216
5. MAIL:
Mark “Confidential” on the envelope and mail the medical records to: CIOX Health
2222 W. Dunlap Ave. Phoenix, AZ 85021
Humana Physician News Q1 2023
Just to mention a few topics:
- Financial Assistance for patients
- Real-time Benefit check
- Medication reconciliation for reduced hospital readmission
UHC Reconsideration and Appeals Going Digital
This change affects Commercial and MA health care professionals.
UHC Network News
Cigna 1st Qtr 2023 Network News
Billing Codes Reported to Payor May Differ from Codes Authorized.
Have you ever requested authorization on a particular procedure (CPT Code) only to find out afterward there are additional codes or even a totally different CPT code than you requested?
It doesn’t help that only some payors allow for a retro authorization (auth)
and usually they have a short turnaround time.
Below are some tips from the MGMA Community.
From a Surgical Practice:
- Have the Surgical attendee to inform the Prior Auth. Manager or Coder as soon as the procedure is completed.
- The coder should compare procedure notes to the auth prior to billing.
From an ENT Practice:
- Have the physician give you all the possible CPT codes that could be performed and precert. them to be on the safe side.
From a Gastro Practice:
- Again request an auth. for all possible code combinations from the payor.
From an Ortho:
- Create a report that compares billed codes to approved codes.
- Then hold the claim for business days to make certain you have time to reach out to insurers and make adjustments.
- They have found that most insurers want it updated before they process the claim. Which is what the office wants also because it prevents refiling. Even if it takes additional months to get the prior auth. changed.
Summarized:
- Authorize all possible codes for the procedure.
Work with your insurance follow up team to identify our opportunities. This may lead to updates on how you order certain procedures. An update to both system and workflow.
- Timely charge capture. Because retro auth windows are short for some payors, it is imperative to understand if the codes being captured is different from codes authorized.
Same as #1. You have to assess how the charge lag is contributing to the denials.
- A process to compare codes being captured vs authorized and request retro auth.
This concept is for review before charges are submitted. Compare codes in charge sessions vs the codes authorized and flag sessions that have discrepancies so retro auth can be pursued.
PRINT THIS!
For Easy Access
Click the blue box for a printable download.
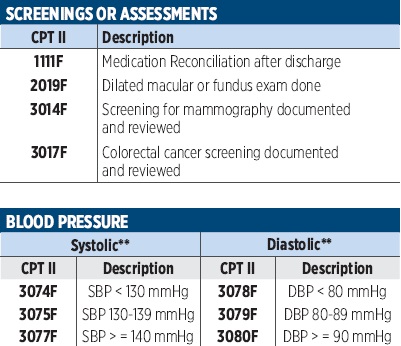
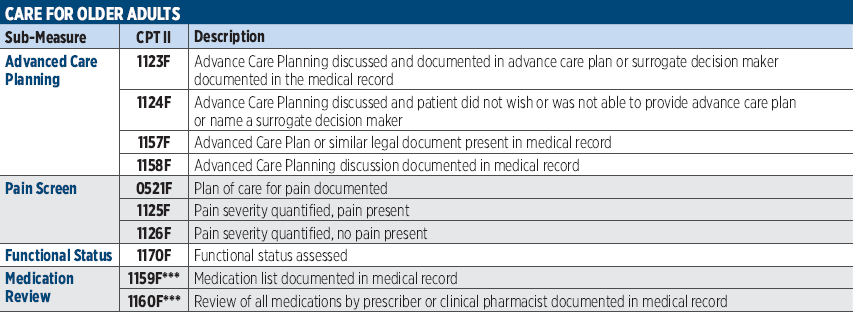
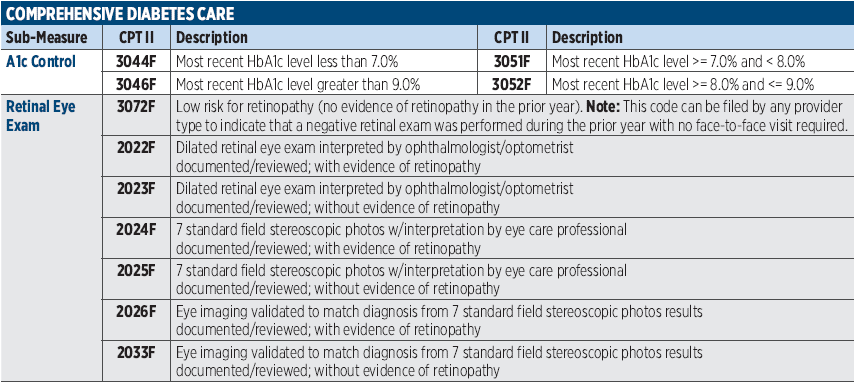
Is CIOX a Pain?
If you are having issues with CIOX, please let POET know.
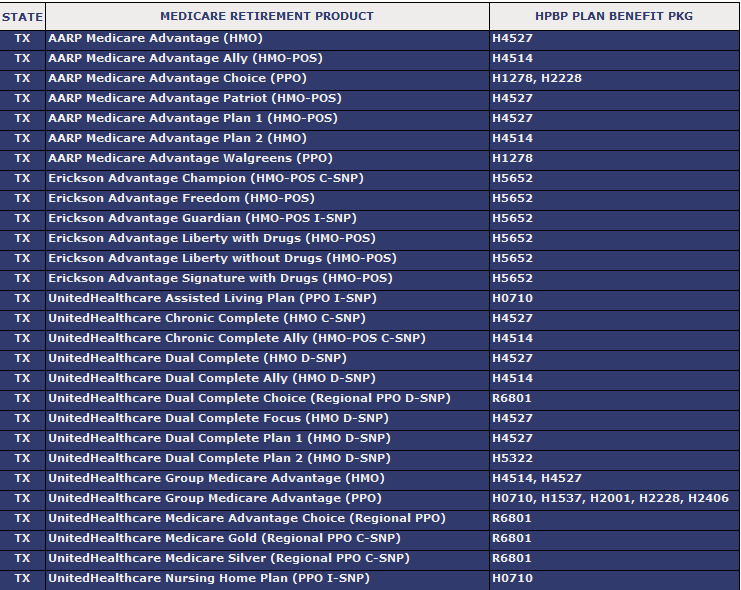
UHC MA Plans

The below list is for Provider use only. Not to be distributed to Patients.
Information Provided by Melissa Boyd, UHC Network Account Manager


Recent Comments