Tag: Billing
13 Reasons a Claim is Denied

1). A duplicate claim was submitted when a practice hasn’t received reimbursement.
2). The patient isn’t eligible for services because their health plan coverage ended, and the patient hasn’t shown proof of new insurance.
3). The patient hasn’t met his/her deductible for the year.
4). Some services are bundled. For example, laboratory profiles with multiple tests don’t qualify for separate reimbursements, or an all-encompassing rate covers the minor procedures and the pre- and post- procedure visits. The provider receives one combined payment.
5). The benefit has been exceeded, such as the maximum allowed number of physical therapy visits covered by the health plan within a calendar year.
6). The claim form is missing a modifier, or modifier(s) are invalid for the procedure code (as in the case of bilateral codes billed on both sides).
7). An inconsistent place of service is marked on the claim form, such as an impatient procedure billed in an outpatient setting.
8). A particular service isn’t covered under the plan’s benefits, or there appears to be a lack of medical necessity. In another example, there could be a mismatch between the actual diagnosis and the service performed.
9). The claim is deficient in certain information. It may be missing prior authorization or the effective period within which the pre-approved service must be provided for the reimbursement to occur.
10). There is a coding data error with mismatched totals or mutually exclusive codes.
11). It may be necessary to coordinate benefits when dual coverage issues arise, such as with secondary insurance or worker’s compensation.
12). The filing deadline has passed. If a claim isn’t submitted to the insurer within the permitted time frame, it is likely to be rejected. The limit to file can be as short as 90 days from the date of service.
13). Errors or typos were made while collecting pertinent information from the patient or during the data entry process for a claim.
Renewed Form for ABN

The ABN, Form CMS-R-131, and form instructions have been approved by the Office of Management and Budget (OMB) for renewal. The use of the renewed form with the expiration date of 01/31/2026 will be MANDATORY on 6/30/23.
The Advance Beneficiary Notice of Noncoverage (ABN), Form CMS-R-131, is issued by providers to Original Medicare (fee for service – FFS) beneficiaries in situations where Medicare payment is expected to be denied.
The ABN is issued in order to transfer potential financial liability to the Medicare beneficiary in certain instances
CHIP Co-Pay Resumes
At the end of the PHE, May 11, 2023

Superior announcing the CHIP Co-Pay will resume.
Superior Risk Adjustment Training
Superior will be hosting a series of webinars to assist providers with Risk Adjustment Documentation and Coding. All levels of clinicians and billing and coding staff are encouraged to attend.
Prevent Improper Code Bundling
Physicians can take advantage of a new Medicare tool to sort through service codes that can be bundled together for claims payment – and AVOID improper billing.
The CMS recently released the National Correct Coding Initiative (NCCI) procedure-to-procedure (PTP) lookup tool to promote accurate code-bundling and prevent improper payment of Medicare Part B and Medicaid claims when incorrect code combinations are reported.
Available via Texas’ Medicare contractor Novitas Solutions, the tool is further designed to help physicians identify when certain pairs of codes are subject to automated edits.
AND FOR EVEN MORE TOOLS
CLICK ON ANY OF THE BUTTONS BELOW
Billing Codes Reported to Payor May Differ from Codes Authorized.
Have you ever requested authorization on a particular procedure (CPT Code) only to find out afterward there are additional codes or even a totally different CPT code than you requested?
It doesn’t help that only some payors allow for a retro authorization (auth)
and usually they have a short turnaround time.
Below are some tips from the MGMA Community.
From a Surgical Practice:
- Have the Surgical attendee to inform the Prior Auth. Manager or Coder as soon as the procedure is completed.
- The coder should compare procedure notes to the auth prior to billing.
From an ENT Practice:
- Have the physician give you all the possible CPT codes that could be performed and precert. them to be on the safe side.
From a Gastro Practice:
- Again request an auth. for all possible code combinations from the payor.
From an Ortho:
- Create a report that compares billed codes to approved codes.
- Then hold the claim for business days to make certain you have time to reach out to insurers and make adjustments.
- They have found that most insurers want it updated before they process the claim. Which is what the office wants also because it prevents refiling. Even if it takes additional months to get the prior auth. changed.
Summarized:
- Authorize all possible codes for the procedure.
Work with your insurance follow up team to identify our opportunities. This may lead to updates on how you order certain procedures. An update to both system and workflow.
- Timely charge capture. Because retro auth windows are short for some payors, it is imperative to understand if the codes being captured is different from codes authorized.
Same as #1. You have to assess how the charge lag is contributing to the denials.
- A process to compare codes being captured vs authorized and request retro auth.
This concept is for review before charges are submitted. Compare codes in charge sessions vs the codes authorized and flag sessions that have discrepancies so retro auth can be pursued.
PRINT THIS!
For Easy Access
Click the blue box for a printable download.
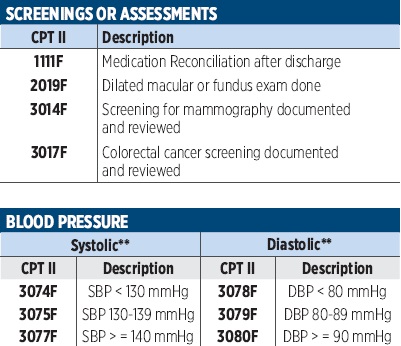
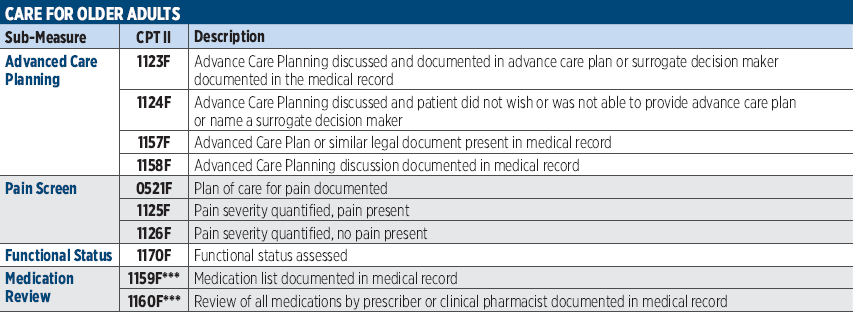
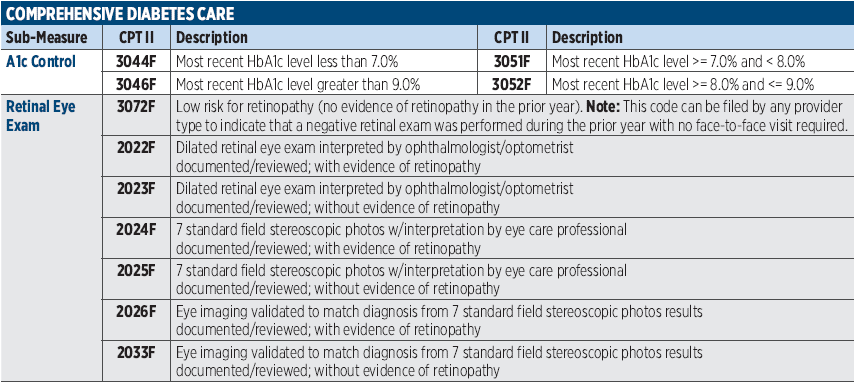
Imagine 360 – POET Alert!
Please notify POET if you are having issues of any kind with claims from Imagine 360.
If you have submitted paper or electronic claims to Imagine 360, please check to see if they have been received by them.
Thank You.
New Claim Tool for UHC
TrackIt
There are many reasons to love TrackIt. But this time of year, its ability to save you time ranks pretty high. Need to add information to a claim or check a prior authorization status? Skip the phone or waiting for the mail. You can find all that and more in TrackIt. The tool makes it easy to stay on top of your UnitedHealthcare tasks by showing what items need attention, so you can take action in real time — and get back to your holiday to‑do list faster.
Is it Posssible, Well and Sick Same Day?
Having Trouble Closing Those Gaps?
Check out these two articles from the POET InK files.
How to Code a Well Visit with a Sick Visit.
HEDIS News You Can Use
Recent Comments