Tag: CMS (Medicare and Medicaid)
Prevent Improper Code Bundling
Physicians can take advantage of a new Medicare tool to sort through service codes that can be bundled together for claims payment – and AVOID improper billing.
The CMS recently released the National Correct Coding Initiative (NCCI) procedure-to-procedure (PTP) lookup tool to promote accurate code-bundling and prevent improper payment of Medicare Part B and Medicaid claims when incorrect code combinations are reported.
Available via Texas’ Medicare contractor Novitas Solutions, the tool is further designed to help physicians identify when certain pairs of codes are subject to automated edits.
AND FOR EVEN MORE TOOLS
CLICK ON ANY OF THE BUTTONS BELOW
2023 Medicare Physician Fee Schedule Final Rule

On November 01, 2022, the Centers for Medicare & Medicaid Services (CMS) issued a final rule that includes updates and policy changes for Medicare payments under the Physician Fee Schedule (PFS), and other Medicare Part B issues, effective on or after January 1, 2023.
TX Resources for Family

Physicians who frequently refer patients to no- and low-cost state services like health insurance and child care will find that easier now that the state has launched familyresources.texas.gov, a website that puts links to those services all in one place.
Who ya’ gonna call?
HAVING ISSUES WITH MEDICARE CALLS?
Who do you call? A source from MGMA shared this information.

They suggest you file a complaint and email CMS leadership. Because complaints go to “low-level” administrative staff whose entire goal is to close them.
Create a complaint letter detailing your experience. Email it to CMS Administrator Chiquita Brooks-LaSure Administrator and CC to the relevant CMS leadership as follows:
CMS Administrator: Chiquita Brooks-LaSure [email protected]
Deputy Chief Operating Officer: Karen Jackson [email protected]
Director Office of Program Operations & Local Engagement: Nancy O’Connor [email protected]
Deputy Administrator and Director Center for Medicare: Meena Seshamani, M.D., PhD [email protected]
Deputy Administrator & Director Center for Medicare & Medicaid Innovation: Elizabeth Fowler [email protected]
Deputy Administrator and Director Center for Consumer Information & Insurance Oversight: Dr. Ellen Montz [email protected]
Deputy Director: Cheri Rice [email protected]
Seasonal Influenza Vaccines Pricing
The Medicare Part B payment allowance limits for seasonal influenza (flu) vaccines are 95% of the Average Wholesale Price (AWP), as reflected in the published compendia.
In hospital outpatient departments, payment is based on reasonable cost.
Annual Part B deductible and coinsurance amounts don’t apply for the influenza virus vaccinations. All physicians, non-physician practitioners, and suppliers who administer these vaccinations must take assignment on the claim for the vaccine.
Annual Influenza Vaccine season starts on August 1 and ends on July 31 of the following year.
Payment Allowances and Effective Dates by Flu Season
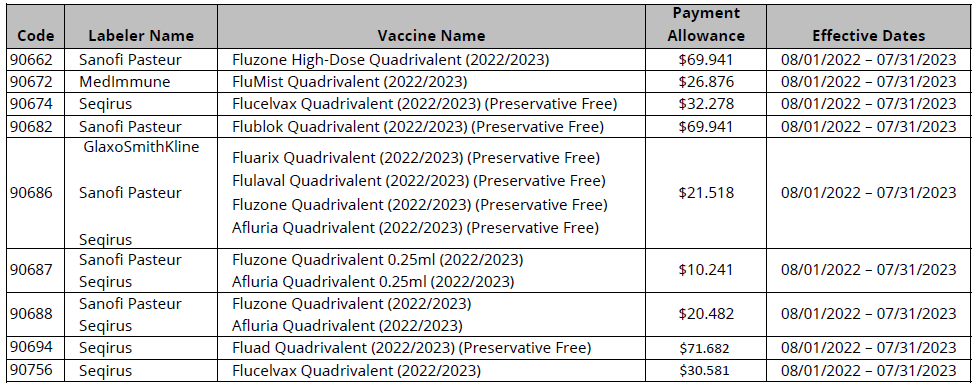
2% Medicare Sequester
Back to the ax!

July 1, 2022, CMS will begin sequestering the full 2% off your Medicare payment.
Paying to Get paid!

The Centers for Medicare & Medicaid Services (CMS) released new guidance that seeks to clarify requirements
for electronic funds transfers (EFT).
Although this guidance does not address all of MGMA’s questions and concerns (see MGMA’s letter to CMS), we are encouraged that CMS heeded our call to issue additional guidance and that CMS acknowledged in this guidance that a health plan may not adversely affect or attempt to adversely affect a provider, should a provider desire to receive EFT using a standard transaction
MGMA has voiced concerns to CMS that the business associates that health plans use to render payments to practices levy fees on the transaction. We are adamant that these ‘pay to get paid’ schemes are unacceptable and that CMS should prohibit these abuses. Although the guidance does not explicitly address these fees, it does clearly state that health plans cannot require providers to receive payment from its business associates. In essence, as we understand it, the fact that a plan cannot require a practice to agree to receive payment from its business associates should allow practices to forgo interacting with these vendors and thus avoid the fees.
MGMA is seeking further clarity on this guidance and stands firm on our belief that health plans and their business associates should be forbidden from levying these fees on medical groups.
Federal Judge Ruled in favor of TMA
Published 2/25/2022, Written by Kelsey Hagg, Associate Director Government Affairs MGMA
“In late 2021, the Texas Medical Association filed a lawsuit against the U.S. Department of Health and Human Services (HHS) alleging that the interim final rule establishing the qualifying payment amount (QPA) as the assumed out-of-network rate went against congressional intent and stating that all criteria (including the QPA) considered by the independent dispute resolution (IDR) entity should be weighted equally.
This morning a federal judge in Texas issued a motion for summary judgement ruling in favor of the Texas Medical Association.
The court determined that HHS violated the Administrative Procedures Act (APA) when issuing rulemaking establishing the QPA as the assumed out-of-network rate in the federal IDR process. This ruling means that if the higher courts don’t overturn or pause implementation pending appeals, we expect the IDR process to begin without the portions of the rule that were vacated.
Specifically, we expect the IDR process to begin without the QPA as the established out-of-network amount. Under this ruling, IDR entities do not have to select the payment amount that is closest to the QPA, nor do IDR entities have to describe the credible information that determined the QPA was materially different from the chosen out-of-network rate.
Additionally, we wanted to share information we received from CMS. In a call with the agency, a CMS spokesperson stated that they intend to open the federal IDR portal on Monday, February 28, 2022. However, this information is subject to change and we will keep you posted on any additional information we receive from the agency. Questions for CMS about the federal IDR process can be directed to: [email protected].
Please let us know if you have any additional questions.

Recent Comments