Tag: CMS (Medicare and Medicaid)
When the PHE Expires, What then?
How to Reverify Patients’ Medicaid Eligibility
When the Public Health Emergency Ends
With the federal public health emergency (PHE) slated to expire at the end of 2021, millions of Medicaid patients across the U.S. are at risk of losing their coverage. Texas physicians should prepare by scheduling services as soon as possible for such patients and evaluating the financial impact of potential increases in uncompensated care. They also should expect to reverify patients’ Medicaid eligibility when the PHE expires.
Physicians can reverify patients’ eligibility electronically through the Texas Medicaid & Healthcare Partnership (TMHP) Electronic Data Interchange, TexMedConnect, or the Medicaid Client Portal. They can also call the TMHP Automated Inquiry System at (800) 925-9126.
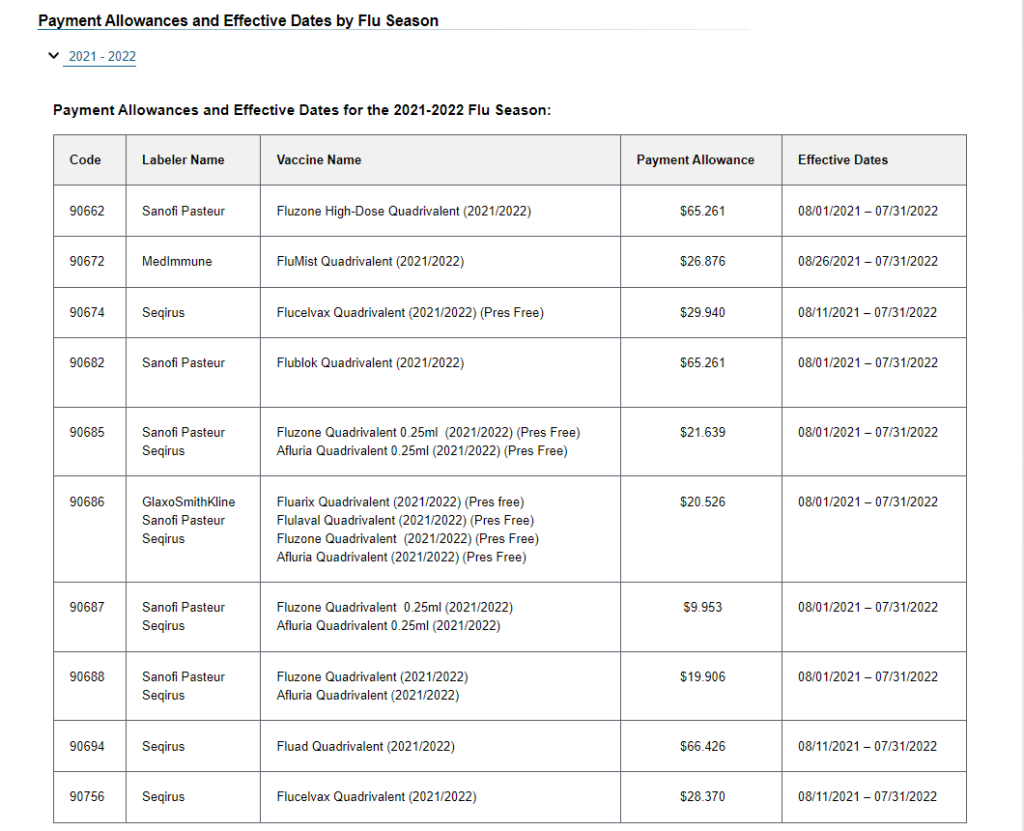
Seasonal Influenza Vaccine Pricing
CMS Web-Based Learning
Have you and your staff completed your Annual Fraud, Waste and Abuse (FWA) training for 2021 as outlined in the 2021 Medicare Compliance Program Guidelines Attestation for Downstream Entities?
- Fraud, Waste and Abuse (“FWA”) Training
Fraud, Waste and Abuse Training was provided in 2021 to all of our employees, contractors and downstream entities who are assigned to work on Medicare business. This occurred initially during the orientation period and annually thereafter. Records of Fraud, Waste and Abuse Training completion are maintained for at least 10 years

CMS has recently revised their Multimedia Web-based Training.
And it’s free
Flu, Pneumococcal, and Hepatitis B
Prior Auth Changes, Superior

Prior Authorization Changes,
Effective September 1, 2021

New Codes Requiring Auths:
- 33270
- 33271
- 33274
Prior Auths Removed:
- 33273
- 93287
- 93290

In Accurate Medicare Claim DENIALS!!
Novitas Solutions, the Medicare payer for Texas, announced that a system error has caused the improper rejection of Medicare Part B claims submitted on or after July 6. Physicians who received a claim rejection message should not resubmit claims at this time. Novitas says it is researching a claims processing system fix. TMA is monitoring the problem.
HOSPITALS ARE REQUIRED!!

As of May 1, hospitals are now REQUIRED to electronically share their admit, discharge, and/or transfer (ADT) notices with the patient’s established primary care physician (pcp), group, or other practitioner identified by the patient.
As part of the same rule, PHYSICIANS ARE REQUIRED to update their digital contact information in the National Plan and Provider Enumeration System so hospitals have the information they need to electronically send the ADT notices.
From CMS.Gov
Critical Care Evaluation & Management Services: Comparative Billing Report in May
In late May, CMS will issue a second letter in the Special Edition Comparative Billing Report (CBR) series on Part B claims for critical care evaluation & management services. Use the data-driven tables to compare your billing and payment patterns with peers in your state and across the nation.
The public can’t view CBRs. Look for an email from [email protected] to access your report. Update your email address in the Provider Enrollment, Chain, and Ownership System to ensure delivery.
More Information:
- View a webinar recording
- Visit the CBR website
- Register for a live webinar on June 9 from 3-4 pm ET
SEP for Individuals Affected by a Disaster or Emergency, Humana 2021
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2021/06/2021-Compliance-Communication.pdf” download=”all” viewer=”google”]

Recent Comments