Tag: Medicare Learning Network (MLN)
Goverment Shutdown: What you Need to Know
With the government shutdown in effect, the Texas Medical Association is in regular communication with federal colleagues at the American Medical Association on the impact to physician practices, as AMA remains in touch with senior officials at the Centers for Medicare & Medicaid Services (CMS).
The volatility in Washington, D.C. could mean the shutdown lasts days to weeks, and TMA will share additional information via Texas Medicine Today as the situation develops. Here is what physicians need to know so far:
Medicare/Medicaid: The CMS contingency plan states that during a lapse in funding, the Medicare program will continue. CMS also says it has sufficient funding for Medicaid to fund the first quarter of 2026 and is maintaining the staff necessary to make payments to eligible states for the Children’s Health Insurance Program.
Medicare Administrative Contractors (MACs) have been instructed to implement a temporary claims hold of 10 business days, which AMA says should have minimal impact on physicians due to the 14-day payment floor. “The hold prevents the need for reprocessing large volumes of claims should Congress act after the statutory expiration date,” states a CMS Medicare Learning Network Connects special edition email newsletter that, as of this writing, had not yet been publicly posted. Physicians may continue to submit claims during this period, but payment will not be released until the hold is lifted. For the latest information, AMA recommends physicians monitor their MAC’s website (Novitas in Texas) and this CMS webpage.
“In the past, Congress generally has restored lapsed policies back to the effective date of the shutdown. During the shutdown, the AMA is monitoring any potential delays in Medicare claims processing or other Medicare payment problems that could result from federal staffing reductions at CMS, including during the shutdown,” said AMA CEO and Executive Vice President John Whyte, MD, MPH.
Telehealth: Physicians who provide telehealth services to fee-for-service Medicare patients should be aware that the Medicare telehealth flexibilities lapsed on Sept. 30 for most care and congressional action is required to restore that waiver. The exceptions are patients being treated for mental health and/or behavioral health disorder (including substance use disorders), stroke, and monthly end-stage renal disease visits for home dialysis. Otherwise, telehealth services are limited to rural areas as they were before the COVID public health emergency, and patients cannot receive telehealth services in their homes. The ability to provide audio-only services to Medicare patients also lapsed, as did the Acute Hospital Care at Home program.
The CMS newsletter suggests “practitioners who choose to perform telehealth services that are not payable by Medicare on or after Oct. 1, 2025, may want to evaluate providing beneficiaries with an Advance Beneficiary Notice of Noncoverage.”
However, AMA notes physicians in certain Medicare Shared Savings Program accountable care organizations can continue to provide and be paid for telehealth services.
Other services: CMS says it is continuing federal insurance marketplace activities, such as eligibility verification. Other nondiscretionary activities including health care fraud and abuse control and Center for Medicare & Medicaid Innovation activities are also continuing.
However, AMA reports that funding extensions for community health centers, the National Health Service Corps, and teaching health centers that operate graduate medical education programs expired on Sept. 30, and the 1.0 work geographic practice cost index floor extension expired on Oct. 1. Additional programs that have lapsed include: special diabetes programs; public health emergency authorities (e.g., Public Health Emergency Fund); increased inpatient hospital payment adjustment for certain low-volume hospitals; the Medicare-Dependent Hospital program; quality measure endorsement, input, and selection; and outreach and assistance for low-income programs (e.g., area agencies on aging).
TMA wants to hear from you. If you or your practice staff experience Medicare payment delays, telehealth obstacles, or other concerns, please let us know through TMA’s Knowledge Center to help inform advocacy.
Amy Lynn Sorrel
Associate Vice President, Editorial Strategy & Programming
Division of Communications and Marketing
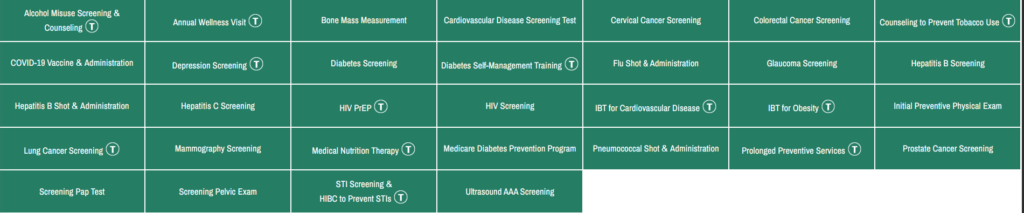
Medicare Preventive Services – Revised
The above link will lead you to MLN Educational Tool, where you can click a service and see the changes.
How to Use Add-on Code G2211
MLN Connects News
2024 Medicare Part B Deductible.
The annual deductible for all Medicare Part B beneficiaries will be $240 in 2024, an increase of $14 from the annual deductible of $226 in 2023.
Discarded Drugs and Biologicals:
When to Use JW and JZ Modifiers.
Read updated JW and JZ Modifier FAQs for additional clarity on billing with these modifiers (see FAQs 7, 8, and 18–22). CMS posted a new list of billing and payment codes only used for single-dose containers that may require the modifiers, depending on the setting:
Your Patient’s MBI may change!

Over 47,000 Medicare Beneficiaries may been involved in a Data Breach that involved Personally Identifiable Information (PII) and/or Protected Health Information (PHI).
New Medicare Cards with a new Medicare Beneficiary Identifier (MBI) are being mailed out.
Ask Your Patients, If They Have A New Medicare Insurance Card!!
Quarterly Update for Clinical Laboratory Fee Schedule (CLFS)
Quarterly Update for Clinical Laboratory Fee Schedule (CLFS) and Laboratory Services Subject to Reasonable Charge Payment
Medicare Claims Rejected
Special Edition of CMS MLN Connects November 12,2019
HICN Claims Reject
We are 50 days out from the end of the Medicare Beneficiary
Identifier (MBI) transition period. Use the MBI on Medicare claims and other
transactions now. Starting January 1, regardless of the date of service:
- We
will reject claims submitted with Health Insurance Claim Numbers (HICNs)
with a few exceptions - We
will reject all eligibility transactions submitted with HICNs
See the MLN Matters Article to learn how to get and
use MBIs.
New Medicare Card: HICN Claims Reject January 1, 2020
from CMS MLN Connects
Starting January 1, you must use Medicare Beneficiary Identifiers (MBIs) when billing Medicare regardless of the date of service:
- We will reject claims submitted with HICNs with a few exceptions
- We will reject all eligibility transactions submitted with Health Insurance Claim Numbers (HICNs)
See the MLN Matters Article to learn how to get and use MBIs.


Recent Comments