Tag: Physicians Practice
Beware these malpractice landmines!

By Logan Lutton, Chris Mazzolini
~Physicians Practice
EHRs are increasingly leading to malpractice lawsuits. While EHR-related lawsuits still make up only a small number of lawsuits, user error is the cause of 64 percent of EHR-related malpractice claims, according to the Doctors Company. Practices need to focus on eliminating several common problems, mostly tied to user actions, which have led to the majority of EHR-related suits
Many doctors are tempted to copy a note from a prior encounter and make changes as appropriate. This leads to a few potential problems.

“Sometimes physicians forget to update the note with the appropriate changes when copying and pasting” David Troxel, MD, MeD & Sec. Doctor’s Company Brd. of Gov.
Drop-down menus can often be the source of a user error that leads to a malpractice suit. Not only can users click the wrong thing in the menu, such as the wrong patient symptom, but these menus lead to structured information that physicians can easily overlook when reviewing a note

Jeffrey Kagan, MD, a Newington, Ct.-based internist, has experience reviewing malpractice cases for attorneys. One trend he has seen related to EHR-induced malpractice suits comes from template use.

“Templates are supposed to help us do something more comprehensive, but often our templates have a lot of old information that carries forward,” he says. In order to avoid falling into this trap, He advises physicians to proofread and modify templates.

The e-prescribing module in an EHR is a potential landmine for malpractice. Alerts indicating when there is a problem with medication dosage or drug-drug interaction will pop up as practitioners are inputting data into the EHR. As a result, doctors get annoyed and develop alert fatigue, and they just turn the alerts off. While this is understandable, turning off the alerts could mean a potential significant problem could go undetected.

Another prompt that goes ignored, often to the determinant of the patient and the doctor, are clinical decision support (CDS) alerts. These are clinically relevant educational materials that come up as the practitioner is documenting in the EHR. Practitioners should ignore these at their own peril, Troxel says. If anything, physicians should document the reason why they overrode the CDS alert.

The idea of physicians missing a vital piece of information in the EHR can be either a user or a technical error. These types of problems are most likely to crop up when a physician is using a new system.
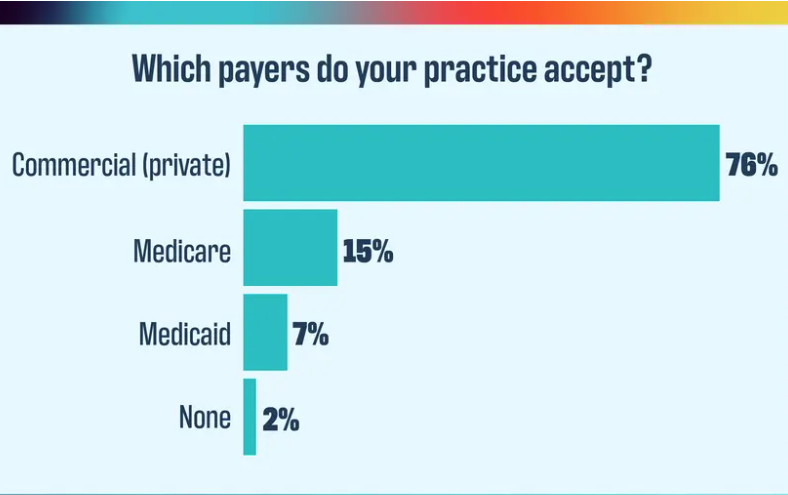
2024 Payer Scorecard: How payers are failing practices and patients
Physicians Practice: November 11, 2024, By Keith A Reynolds

How would you characterize your prior authorization experience in the last year?
We’re doing more prior authorizations
74%
We’re doing fewer prior authorizations
4%
Prior authorizations are about the same
22%

Do you think there should be a CPT code requiring payers to reimburse for prior authorization work?
Yes
97%
No
3%



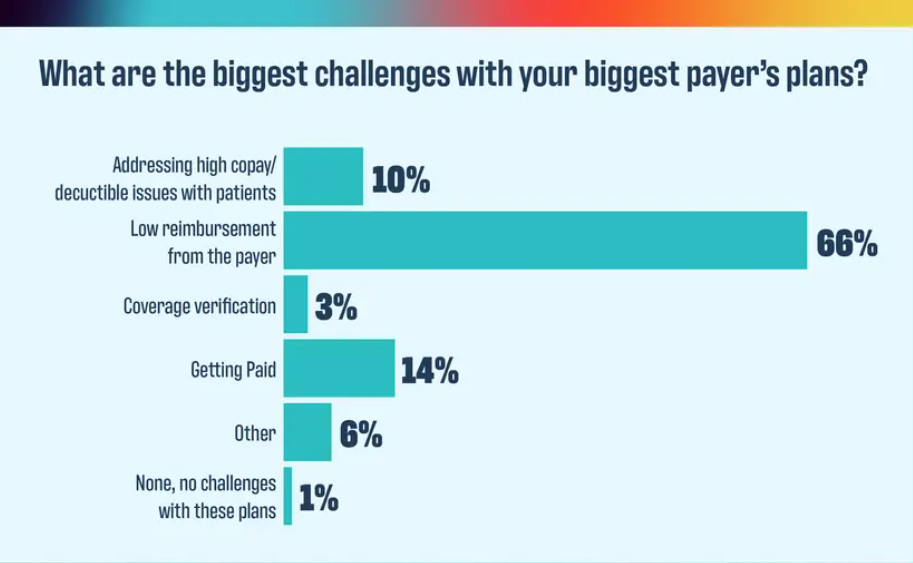
What is your biggest challenge with your biggest payer?
- Current systems don’t interact well with our billing systems requiring office staff to correct claims leading to delayed payment
- Reimbursement stinks. I Quit !!!!!!
- Staff the insurance companies contracted are mostly out of the country and do not know the issues we have and do not like to refer the questions or specific issues to any expert in the field.
- Small practice is ignored. They would not negotiate fees. For more than 15 years no increase in fees, only steady decrease. It is a shame, no respect any longer for providers.
- Prior authorizations waste so much time for what should be a simple process
- Lack of urgency or even motivation to provide basic service
The verdict is in for how practices feel about their payers, and it isn’t good.
How can payers improve their relationship with practices?
- Streamline systems to allow for clean claims the first time
- Have a dedicated Provider Relations contact so we know who to talk to, and who to call to get responses to critical questions, not have to send emails to faceless representatives that have a low rate of resolution.
- Communicate. Show WHY they deny, and what EXACTLY can be done to help the patients who pay them. Do not simply deny with NO guidance.
- Pay us enough to survive. Instead, they raise hospital payments. Paying us more so we could hire more doctors and physicians assistants and keep people OUT of those hospitals.
- Stop putting technology problems and carrier losses on the provider and their patients.
- Instead of looking at me as an expense, look at me as a tool to care for their beneficiaries.
- Stop requiring PAs for generic meds and obviously necessary medications.
Termination of Employee
No matter how much time we spend vetting potential hires, eventually, someone isn’t going to work out.
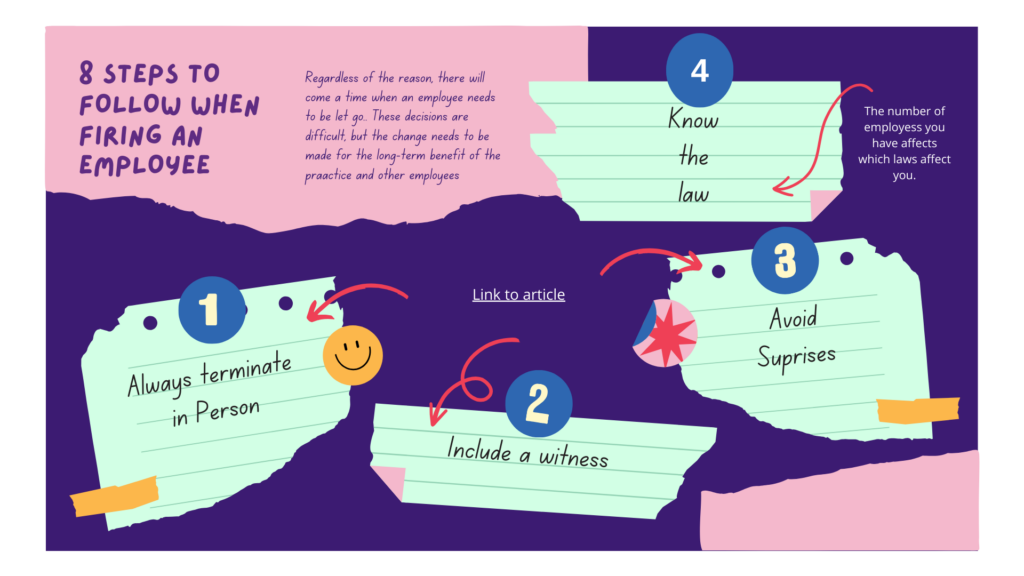
Regardless of the reason, there will come a time when an employee needs to be let go. These decisions are difficult, but the change needs to be made for the long-term benefit of the practice and the other employees.

STOP BACK OFFICE THEFT

5 Tips to Help Stop Theft in Your Back Office
It’s unfortunate, but even in today’s era of two-factor authentication and hyper-alert security, we still hear stories of physicians being defrauded by their employees. To help protect yourself from financial fraud, consider adopting these five approaches in your practice.
1) Cross-Train Your Employees
The most common place for fraud to occur is in the back office of small businesses where only one person handles the cash and books. Train more than one person on the cash conversion cycle. Rotate people through the various processes, too, so that no single person operates in a silo. When multiple people know the process, they can check each other’s work for mistakes and anomalies. Cross-training employees helps to create an open and transparent environment. It also reduces the chance of theft by assuring no one person wields too much power. Ultimately, it would be best if you also knew the process, so you can be an effective leader and fiscally responsible business owner
7 Tips to Combat Embezzlement
Reducing medical practice embezzlement risk with cash controls
13 Reasons a Claim is Denied

1). A duplicate claim was submitted when a practice hasn’t received reimbursement.
2). The patient isn’t eligible for services because their health plan coverage ended, and the patient hasn’t shown proof of new insurance.
3). The patient hasn’t met his/her deductible for the year.
4). Some services are bundled. For example, laboratory profiles with multiple tests don’t qualify for separate reimbursements, or an all-encompassing rate covers the minor procedures and the pre- and post- procedure visits. The provider receives one combined payment.
5). The benefit has been exceeded, such as the maximum allowed number of physical therapy visits covered by the health plan within a calendar year.
6). The claim form is missing a modifier, or modifier(s) are invalid for the procedure code (as in the case of bilateral codes billed on both sides).
7). An inconsistent place of service is marked on the claim form, such as an impatient procedure billed in an outpatient setting.
8). A particular service isn’t covered under the plan’s benefits, or there appears to be a lack of medical necessity. In another example, there could be a mismatch between the actual diagnosis and the service performed.
9). The claim is deficient in certain information. It may be missing prior authorization or the effective period within which the pre-approved service must be provided for the reimbursement to occur.
10). There is a coding data error with mismatched totals or mutually exclusive codes.
11). It may be necessary to coordinate benefits when dual coverage issues arise, such as with secondary insurance or worker’s compensation.
12). The filing deadline has passed. If a claim isn’t submitted to the insurer within the permitted time frame, it is likely to be rejected. The limit to file can be as short as 90 days from the date of service.
13). Errors or typos were made while collecting pertinent information from the patient or during the data entry process for a claim.
Difficult Patients
Seems We All Have THAT One.
It’s confusing to refer to a patient as “difficult.”
Difficult?
Are we talking Multiple Comorbidities that are tough to manage?
Maybe they question your medical judgement?
Is it that one that derails your whole day, by telling you their life story?
Or is it just possible they were just born: Angry, Frustrated, and noncompliant?
Whatever the reason for your “difficult” patient, click on the button to view Amanda Hill, JD’s article in Physicians Practice to get some strategies to help deal
HIPAA: Back to the Basics with the BAA, Physician Practice, 2021.08.12
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2021/08/HIPAA-Back-to-basics-with-the-BAA-2021.08.12.pdf” download=”all” viewer=”google”]
HIPAA: Back to Basics with the BAA
With cybersecurity and criminal government actions involving protected health information (PHI), now is a good time to understand the importance of the required Business Associate Agreement (BAA).
HIPAA: Back to basics with the BAA
Defined: “business associate” is a person or entity, other than a member of the workforce of a covered entity, who performs functions or activities on behalf of, or provides certain services to, a covered entity that involve access by the business associate to protected health information. A “business associate” also is a subcontractor that creates, receives, maintains, or transmits protected health information on behalf of another business associate. (emphasis added).
Business Associates encompasses a wide range of persons, which include, but are not limited to: accountants, attorneys, private equity firms, technology companies, app developers, independent contractors, medical device companies, and pharmaceutical companies. Bottom line—if you or your company “creates, receives, maintains, or transmits” protected health information in an electronic form, a BAA is required. This is not new—the requirement existed long before the HIPAA Final Omnibus Rule was published in the Federal Register on January 25, 2013.
HIPAA compliance is not optional and depending on the facts and circumstances, may lead to significant civil and/or criminal liability.
HIPAA, like the Federal Anti-Kickback Statute (AKS), has criminal penalties available to HHS. The DOJ is responsible for criminal prosecutions, as HHS states on its website.
36 Guidelines to Evaluate Practice Management, Practice Management 11/10/2020
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2020/11/36-Guidelines-to-Evaluate-a-Practice-Management.docx” download=”all” viewer=”microsoft”]
Recent Comments