Tag: UnitedHealthcare (UHC)
UHC April Monthly Overview

For Texas:
Starting June 1, 2023, Optum will manage prior authorization and step therapy requests for prescription medications for Texas residents with pharmacy coverage.
More on UHC Electronic Submissions

Get to know the basics of electronic submissions
Now that claim reconsiderations and appeals must be submitted electronically,* we want to help make sure you have the how-to information you need to manage them with ease.
How to submit electronically
You have 2 electronic submission options — through the UnitedHealthcare Provider Portal or Application Programming Interface (API). See the Online Reconsiderations and Appeals interactive guide for step-by-step instructions on how to submit reconsiderations and appeals electronically.
TIPS:
- Check the TrackIt Action Required bar regularly to see the status of claims, reconsideration requests and more
- To take action on a specific claim in the portal, go to Claims & Payments and search for a claim. Once you’ve searched for a claim and selected Act on a Claim, a list of actions will appear (e.g., View Claim Reconsideration, File Appeal/Dispute). Based upon the current status of the claim or previously taken actions, the buttons will either be blue or grayed out. If grayed out, that specific action is unavailable.
- Please note: Available actions may vary based on the member’s plan type, provider’s participation status and regulations
- If a claim(s) from your claim search results shows an “Acknowledgement” status, it hasn’t been processed. You’ll be unable to submit requests related to this claim.
- Reminder: Appeal response letters are no longer mailed, but you can view and print them through the portal using Document Library
UHC March Overview is Here.
UHC Network News is published twice a month.
UHC Reconsideration and Appeals Going Digital
This change affects Commercial and MA health care professionals.
UHC Network News
New Claim Tool for UHC
TrackIt
There are many reasons to love TrackIt. But this time of year, its ability to save you time ranks pretty high. Need to add information to a claim or check a prior authorization status? Skip the phone or waiting for the mail. You can find all that and more in TrackIt. The tool makes it easy to stay on top of your UnitedHealthcare tasks by showing what items need attention, so you can take action in real time — and get back to your holiday to‑do list faster.
UHC Relief At Last!!
Finally, Some United HealthCare Relief!
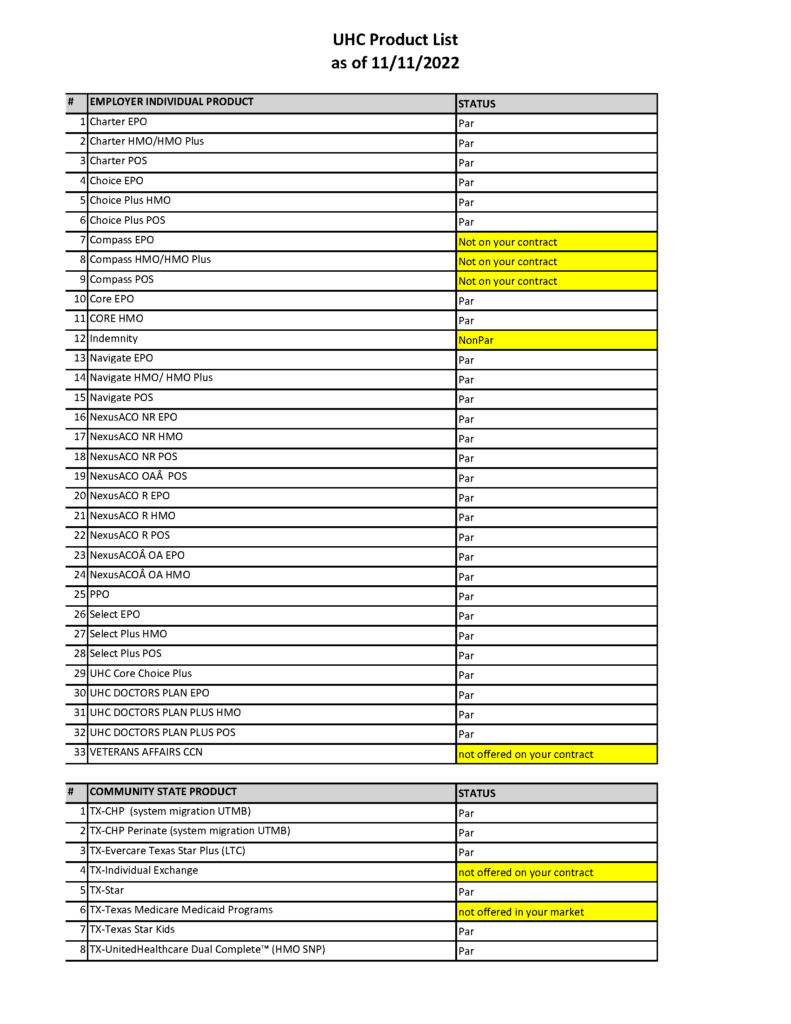
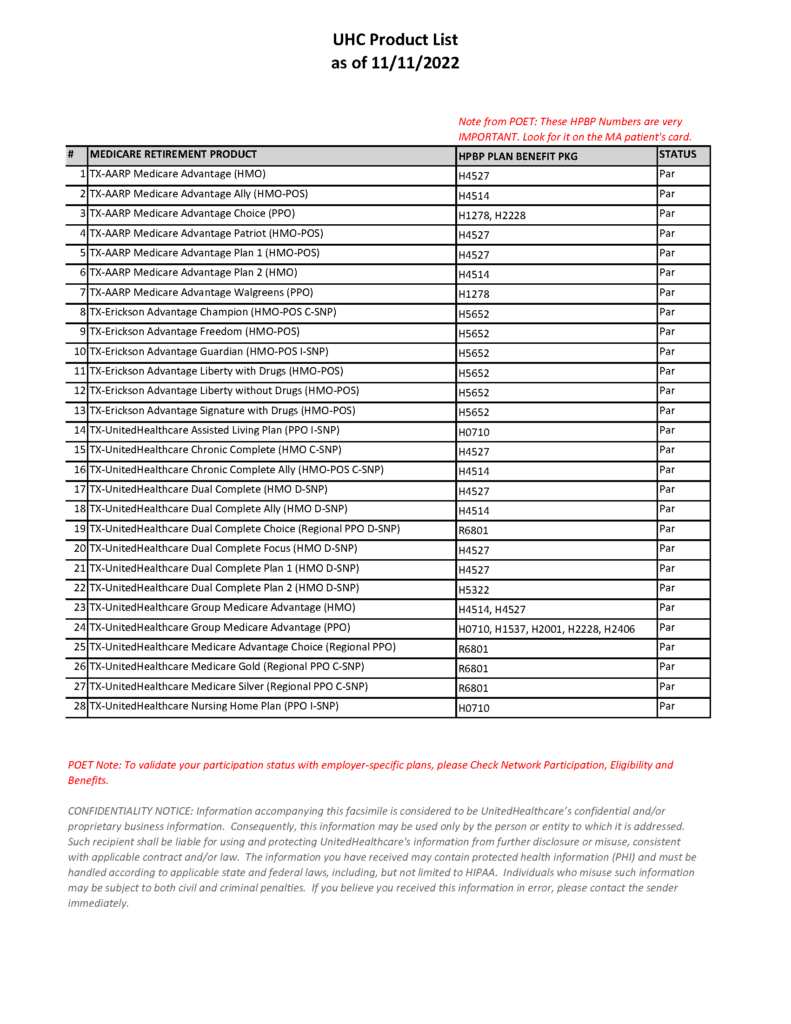
As of this morning POET has acquired a list from UHC regarding the products for our Agreement.
If you are having issues with any par plans on this list. Please email a copy of the card and patients date of birth to [email protected]. Include a brief description of the issue.
Remember this information is confidential and pertains only to the POET Agreement.

UHC Network News

Policy and Protocol Notice
Get the latest updates, legal mandates, state-specific news, trainings and more for Medicare Advantage, Medicaid and Commercial plans.
UHC Updates October 2022

Policy and protocol notice
Get the latest updates, legal mandates, state-specific news, trainings and more for
Medicare Advantage, Medicaid and Individual and Group Market plans.
UHC Network News August 2022

New Smart Edit for Commercial Plans
Effective Aug. 25, 2022, a new Smart Edit will be available for commercial plans to help with coordination of benefits when you submit a claim.
How the new Smart Edit works
When you submit a claim for a member who has a commercial plan and primary health insurance with another carrier, you’ll receive 1 of the following 3 messages on your 277 Claims Acknowledgement report within 24 hours of submission:
- REJECT – This patient has primary insurance coverage with <other insurance name>, <effective Date>. Please resubmit as electronic secondary once adjudicated by the primary payor.
a. You’ll receive this message if we have the primary health insurer’s name and effective date, but don’t have the other carrier’s EOB. - REJECT – This patient has primary insurance coverage with another carrier with <effective date>. Please resubmit as electronic secondary once adjudicated by the primary payor.
a. You’ll receive this message if we have the effective date, but don’t have the other carrier’s name or EOB. - REJECT – This patient has primary insurance coverage with another carrier. Please resubmit as electronic secondary once adjudicated by the primary payor.
a. You’ll receive this message if we’re missing the carrier’s name, effective date and EOB.
What is the Smart Edits tool?
We developed the Smart Edits tool to identify billing errors within a claim so you can quickly review and repair problematic claims. We send these messages within 24 hours of a claim submission so you can review identified claims in a matter of hours instead of potential claims denials days later.
Claims that are accurately submitted and in compliance with the latest policies and regulations result in less rework, quicker approvals and faster payments.
Learn more
- For information on how to submit the primary payer EOB online, visit UHCprovider.com/ediclaimtips > Secondary/COB or Tertiary Claims and Medicare Crossover > COB Electronic Claim Requirements – Commercial
- Visit UHCprovider.com/smartedits to:
- See the list of all available Smart Edits by selecting Smart Edits Guide
- Take a self-paced training by selecting Smart Edits interactive guides
Questions?
- For information about Smart Edits claims, please contact your electronic data interchange (EDI) vendor or clearinghouse
- For additional help from us, visit our EDI Contacts page on UHCprovider.com

Recent Comments