Telehealth Waivers that are tied to the PHE
~Claire Ernst J.D. Government Affairs Director MGMA
On March 15, 2022, President Biden signed the $1.5 trillion omnibus spending package into law, which extended certain telehealth flexibilities related to the PHE. The following waivers will be in effect for an additional 151 days following the conclusion of the PHE:
- Originating site and geographic location: Patients can continue to be treated via telehealth anywhere, including their homes
- Qualifying providers: Physical therapists, occupational therapists, speech language pathologists, and audiologists can furnish distant site telehealth services
- Audio-only services: CMS must continue covering and reimbursing these services
- Federally Qualified Health Centers (FQHCs) and Rural Health Clinics (RHCs): FQHCs and RHCs can be distant sites and be reimbursed
As a reminder, the PHE is in effect until April 16, 2022. It is likely that it will be renewed at least one more time for 90 days.
It’s Only Money

APRIL 1, 2022
$$$
Medicare sequester begins to phase back in at 1%
$$$
POET has a new way of encryption

Sometimes stuff happens that you really didn’t plan on.
Encrypted emails from POET will look a little different.
If you have any problems opening an encrypted email from us please let us know.
Below is a screenshot of what it will look like.
UHC Prior Auth Going Paperless
UHC won’t be sending prior authorization and clinical decision letters by mail starting April 1.
This includes:
- Pre-service/prior authorization decision letters
- Inpatient review letters, including concurrent, retrospective, length of stay and level of care
- Extension for lack of clinical information letters
- Complex care management and OrthoNet letters available in Document Library
Instead, you can view them exclusively online 24/7 through either the UnitedHealthcare Provider Portal or an Application Programming Interface (API) system-to-system data feed.
UHC Policy Updates for March 2022
Just click the button to check out the latest from UHC.
Aetna 3rd-Party Claim and Code Review
Beginning June 1, 2022, you may see new claim edits.
According to March 1, 2022 Aetna OfficeLink Updates: These are part of our Third-Party Claim and Code Review Program. These edits support our continuing effort to process claims accurately for our commercial, Medicare and Student Health members. You can view these edits on our Availity provider portal.*
You can view any of these edits on Aetna’s Availity® provider portal.
For coding changes, go to:
- Aetna Payer Space
- Resources
- Expanded Claim Edits
Except for Student Health, you’ll also have access to Aetna’s code edit lookup tools. To find out if our new claim edits will apply to your claim, log in to our Availity provider portal. You’ll need to know your Aetna® provider ID number (PIN) to access our code edit lookup tools
Here is what POET found with 2022 effective dates:
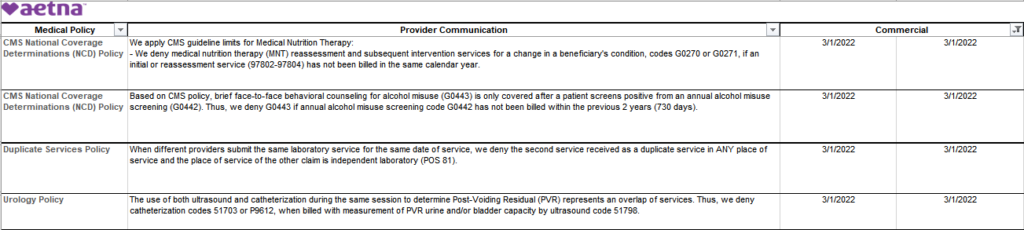
Reference Material for Your Staff that needs it.

Don’t cross your fingers or bring your rabbit foot.
Just download, print and keep a current copy of POET’s Provider Roster and Directory at your desk to make the Referral and Authorization process a bit easier.
File a Complaint
If a provider, believes a health plan isn’t complying with the dispute resolution process, then they may contact the No Surprises Help Desk at 1-800-985-3059 from 8 a.m. to 8 p.m. EST, 7 days a week, to submit a question or complaint. Or, they can submit a complaint online, below. Supporting documentation may be required. We’ll send a confirmation email to the provider when we receive their complaint to notify them of next steps and let them know if we need any additional information. To check on the status of a complaint, or to see what documentation is needed, contact the No Surprises Help Desk.
Recent Comments