Tag: Texas Department of Insurance (TDI)
ERISA or maybe TPA?
Let’s play pretend:
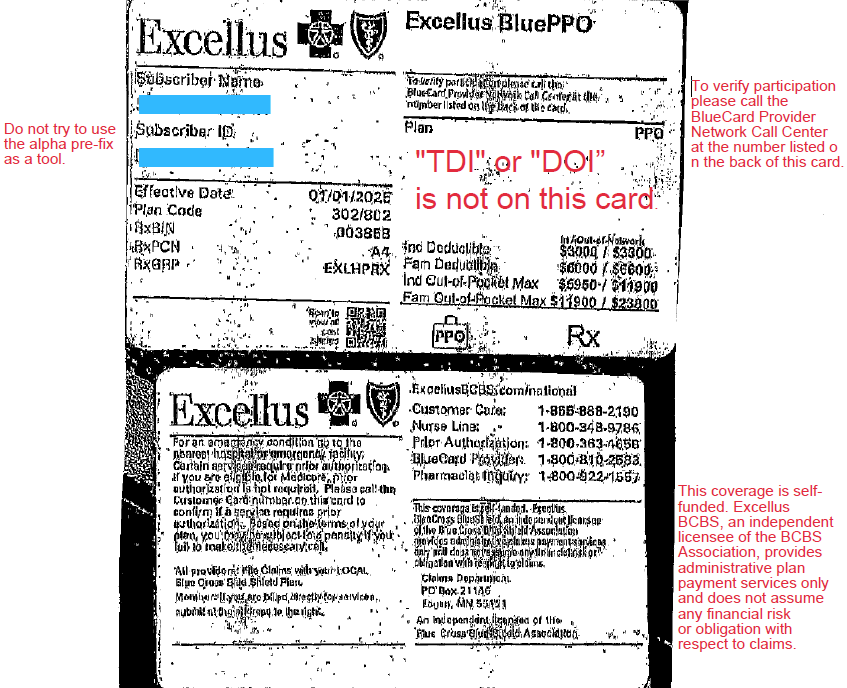
Some one gives you this card and wants to make an appointment.
They seem to want an answer right now.
You know your physician takes Blue Choice, but have never seen this card before. How would you know?
Look at the front of the card. Blue Cross is written all over it. BCBS must be the insurer? STOP!
Do you see any insurance regulation language? Is “TDI” or “DOI” on this card?
NO. This is your 1st clue. The employer may be the insurer.
Scan the front of the card intently. Are there any other clues. Look for what you know, not what you don’t know.
If not flip it over. What do you see? READ ALL THE TINY WRITING.
On this card: phone numbers, addresses, where to file, prior auth info. But what else?
“This coverage is self-funded Excellus BlueCross BlueShield, and independent licensee of the BlueCross BlueShield Association provides administrative claims payment services only and does not assume any financial risk or obligation with respect to claims.”
What does that mean:
- The employer is the insurer (self-funded plan)
- Excellus BCBS is acting as a Third-Party Administrator (TPA)
Is this a Lease Network?
Very likely — yes.
On the front of the card it says:
“To verify participation, please call the BlueCard Provider Network.”
That suggests:
- The plan is using the BlueCard network
- Excellus is providing network access + claims processing. The employer is leasing the BCBS network
That’s what we commonly call a lease network arrangement.
But — this is important — don’t assume, Verify
Why you may still get a “Yes” when you call
When you call provider services:
- The rep may simply see “In Network”
- They may not understand lease networks
- They may not understand the difference between:
- Payor
- TPA
- Repricer
- Network administrator
So we need to ask better questions.
Instead of just asking “Is Dr. Smith in network?”
Tell the representative you would like to check network participation.
Ask:
- Is this plan self-funded? (if it is self-funded it is not a lease network)
- Is Excellus the payor, or the administrator?
- Is this a leased network?
- Who bears the financial risk?
- Is Excellus repricing the claims?
- What network applies to this patient?
And always get:
✔ Representative name
✔ Date/time
✔ Call reference number
If the claim denies, that reference number becomes your leverage.
Why this matters
In lease network plans:
- The employer controls the benefits.
- The employer may carve out services.
- The employer may override network rules.
- The plan can be patient-specific.
Basically they can make up their own rules.
In practical terms — They have more flexibility than a fully insured DOI-regulated plan.
Protect Yourself when speaking to the patient.
Never speak in absolutes.
Use language like:
- “It looks like this is a self-funded plan…”
- “Based on the card wording…”
- “According to the representative I spoke with…”
- “At the time of verification…”
Never say:
- “Yes, you are definitely covered.”
- “This will pay.”
- “You are in network.”
Employer Group PPO/EPO Hybrid
Interpreting insurance cards has never been easy, but with the constant changes in today’s insurance landscape, it has become nearly impossible.
Every week seems to bring a new insurance company—or an established insurer that has acquired several others, rebranded, and rewritten the rules.
On top of that, there are hybrid plans like POS and EPO, along with discount cards, medical cost-sharing programs, limited-benefit plans, and the growing model of Direct Primary Care.
The one pictured below is an ultimate example!
It takes hybrid to a new level of complexity.
By mixing the rules of PPO and EPO in one plan.
Therefore, I, Sir Seymore, have taken my red pen in hand in an effort to make sense of it all.

Feel free to download this card for your records.
Texas Law Requires Practitioners to Disclose AI Use
Texas is imposing new transparency regulations on electronic health records (EHRs) and the diagnostic use of artificial intelligence (AI) under a new state law physicians must begin complying with as of Sept. 1.
Texas Senate Bill 1188, passed during Texas’ 2025 regular legislative session, requires physicians and health care practitioners who use AI for diagnostic purposes – including for any recommendations on a diagnosis or course of treatment based on a patient’s medical records – to, effective Sept. 1:
- Disclose such use of AI to their patients; and
- Review all records created by AI in a manner consistent with medical records standards.
Additionally, entities covered by the bill – businesses, including physician practices, that assemble, collect, analyze, use, evaluate, store, or transmit protected health information – to:
- Automatically allow a minor patient’s parent, guardian, or conservator to obtain “complete and unrestricted access” to the minor’s EHR, unless access to all or part of the record is restricted under state or federal law or by court order, also effective Sept. 1; and
- Physically maintain their EHRs only within the U.S. or a territory of the U.S. and only allow their data to be accessed by those who require the information to perform duties within their scope of their job related to treatment, payment, and other health care operations by Jan. 1, 2026. Covered entities have until Jan. 1, 2026 to ensure compliance relating to EHRs prepared before Sept. 1.
However, Texas physicians are now allowed three days to communicate the results of certain sensitive or serious test results to patients, including minors and their guardians, before they are made available via EHRs thanks to the passage of Senate Bill 922.
SB 1188 also prohibits covered entities from amending on an EHR an individual’s biological sex as recorded by a health care practitioner at birth and documented in the EHR, except to correct a clerical error, or, if the individual is diagnosed with a sexual development disorder, to change the individual’s listed biological sex to the opposite biological sex, in which case, information on the disorder must be also included in the EHR.
SB 1188 states regulatory agencies – including the Texas Medical Board, the Texas Department of Licensing and Regulation, and the Texas Department of Insurance – may take disciplinary action against a covered entity that violates the order three or more times in the same manner. The disciplinary action may include “license, registration, or certification suspension or revocation for a period the agency determines appropriate,” per the law.
Violations of SB 1188 can also result in civil penalties ranging from $5,000 to $250,000 per violation, depending on the violator’s intent and whether the violator used protected health information for financial gain.
Physicians should monitor for future guidance and check with their EHR vendor about compliance, especially as related to where patient data is stored, says Shannon Vogel, the Texas Medical Association’s associate vice president of health information technology.
For more information on health information technology, visit TMA’s related webpage.
ALERT: BCBS Not All PPO in the Suitcase Cards Follow the Rule
SAY IT ISN’T SO!
Things to look for: But remember cards are so tricky these days, what applies to one, may not apply for another:
Is the “Texas Department of Insurance” acronym TDI on the card? If a health insurance card does not have “TDI” on it, it is likely an ERISA plan, meaning it is a self-funded plan regulated by federal law and not by the Texas Department of Insurance (TDI) because the employer directly pays claims instead of relying on an insurance company; the absence of “TDI” indicates the plan is self-funded and therefore likely falls under ERISA regulations. (resource tdi.texas.gov)
Look for these phrases, usually on the back of the card:
“BCBS provides administrative services only and assumes no financial risk for claims.”
“JBS will utilize Anthem to handle member contract for Health plan administration”
“Anthem Blue Cross and Blue Shield provide administrative claims payment services only and does not assume any financial risk or obligation with respect to claims”
“BCBST provides administrative services only and assumes no financial risk for claims.”
2/11/25 Amended to add Cigna. Look for these terms on Cigna Commercial cards:
- Shared Administration (S)
- Benefits are not insured by Cigna or Affiliates
Scrutinize each member’s card on an individual patient basis. No rule is across the board.
Network Adequacy Waiver Hearings
TDI will hold virtual public hearings to consider insurers' requests to waive network adequacy standards. Health care providers and consumers can share information for TDI's consideration.
TMA Welcomed Unanimous Passage of House Bill 3359.

A major win for medicine in that it codifies the state’s network adequacy rules by putting them into statute and strengthens their enforcement by the Texas Department of Insurance (TDI).
“HB 3359 restricts insurers from making unilateral contract changes and tackles the problematic waiver process which leaves patients unprotected and in the dark.”
TMA now looks to the rulemaking process. TDI has indicated it likely will rewrite the state network adequacy rules impacted by HB 3359
Texas Prepares to Inplement “GOLD CARD”
HAD YOUR FILL OF BURDENSOME PRIOR AUTHORIZATIONS?
For the Nitty Gritty of how House Bill 3459 is supposed to make your life easier follow this link to the TMA article by Joey Berlin.
Verify Which Health Plans Are Exempt from Prompt Pay Laws 1/4/2021
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2021/02/Verify-Which-Health-Plans-Are-Exempt-from-Prompt-Pay-Laws-2021.01.04-1.pdf” download=”all” viewer=”google”]
How to File a Complaint 12/15/2020
[embeddoc url=”https://community.poetllc.org/wp-content/uploads/2020/12/How-to-file-a-complaint-TDI-BBB-Attorney-General-12152020.pdf” download=”all” viewer=”google”]

Recent Comments